INTRODUCTION
Agranulocytosis is a rare, but potentially serious complication of vancomycin therapy1,2). In drug-induced agranulocytosis, renal insufficiency is associated with a poor prognosis. This is especially true in end stage renal disease (ESRD), a life-threatening condition that is likely to be caused by agranulocytosis, because it is associated with the comorbid conditions related to uremia3). It has been reported that therapy with hematopoietic growth factors, such as granulocyte- and granulocyte-monocyte colony-stimulating factor, may be beneficial in the management of nonchemotherapeutic drug-induced agranulocytosis4ŌĆō7)
We describe an ESRD patient on continuous ambulatory peritoneal dialysis (CAPD) who developed agranulocytosis during the long-term administration of vancomycin. In our patient, agranulocytosis was rapidly resolved by the administration of granulocyte colony-stimulating factor (G-CSF) and the discontinuation of vancomycin. To our knowledge, this is the first reported case of the development of vancomycin-induced agranulocytosis in a CAPD patient.
CASE REPORT
The patient was a 66-year-old man with ESRD due to diabetic nephropathy treated with CAPD. He was admitted because of external cuff infection and severe pneumonia.
On admission, purulent discharge occurred from the exit site of the peritoneal catheter. His total WBC count was 11,750/mm3 and contained 83% neutrophils; the hemoglobin level was 8.2 g/dL, hematocrit 24.3%, and platelets 386,000/mm3. Chest X-ray revealed a pneumonic consolidation on the right upper lobe.
On the 12th hospital day, 1.0 g intraperitoneal (IP) vancomycin was administered every 7 days to treat the infection due to a methicillin-resistant Staphylococcus aureus (MRSA), which was isolated from both sputum and the purulent discharge at the exit site of the peritoneal catheter. Aztreonam, 1.0 g/day, was used simultaneously with vancomycin. Oral rifampin, 600 mg/day, was added on 24th hospital day to treat an external cuff MRSA infection, because no improvement occurred despite the vancomycin therapy. The external cuff infection was not resolved by prolonged vancomycin therapy, but surgical interventions, such as deroofing, cuff shaving, or catheter removal, were not performed because the patient did not consent to a surgical approach. Deroofing and outer-cuff shaving were performed later on the 82th hospital day with the patientŌĆÖs consent. The external cuff infection was cured completely, but vancomycin therapy was continued to treat the MRSA-associated pneumonia. Ceftazidime, 1.0 g qod, was also added because aspiration pneumonia newly developed on the 58th hospital day. The concomitant medications the patient received without discontinuation during hospitalization were; irbesartan, felodipine, carvedilol, ranitidine, domperidone, and multivitamin.
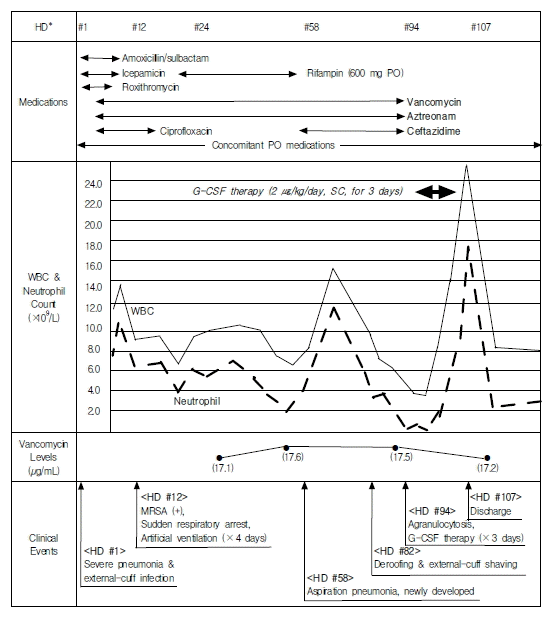
On the 94th hospital day (the 82th of vancomycin and aztreonam therapy and the 36th day of ceftazidime therapy), agranulocytosis developed: the WBC count decreased to a nadir of 4,730/mm3, with 72% lymphocytes and no demonstrable neutrophils (Figure 1). At this time, the hemoglobin level was 8.3 g/dL, the hematocrit 24.8%, and platelets 320,000/mm3. The serum level of vancomycin remained within an acceptable range during vancomycin therapy: with a peak of 17.6 μg/mL and a trough of 17.1 μg/mL. Vancomycin, ceftazidime and aztreonam were discontinued and G-CSF therapy was begun immediately after detecting the agranulocytosis on the 94th hospital day. G-CSF (Neutrogin®) was then subcutaneously administered at 150 μg/day (2 μg/kg/day) for three days. Concomitant oral medications were continued without change during the period of agranulocytosis. The absolute neutrophil count (ANC) improved to a normal level of 3,735/mm3 within 3 days of initiating G-CSF therapy. Four days after initiating of the G-CSF therapy, the peak level of ANC level was 16,815/mm3.
Thereafter, the aspiration pneumonia improved without the administration of antibiotics. One month after discharge, his WBC count was 6,510/mm3 with 55.8% neutrophils.
Six months after discharge, he was readmitted due to CAPD peritonitis. IP cefazolin, 1.0 g/day, and ceftazidime, 1.0 g/day, were administered empirically to treat his CAPD peritonitis. Beta-hemolytic streptococcus was cultured from the dialysate effluent, and ceftazidime was discontinued on the 5th hospital readmission day. Agranulocytosis did not recur despite the rechallenge with ceftazidime.
DISCUSSION
We describe a typical CAPD patient with agranulocytosis, which developed during prolonged vancomycin therapy.
Vancomycin was considered as the cause of the agranulocytosis in our patient, although other medications such as ceftazidime and aztreonam have been used with vancomycin until agranulocytosis was detected. There are several reasons why we believe that the agranulocytosis was induced by vancomycin therapy in our patient. First, agranulocytosis is a rare but well-known complication of prolonged vancomycin therapy1,2,8,9). Second, the agranulocytosis did not recur despite the readministration of ceftazidime, which had been used simultaneously with vancomycin until the agranulocytosis was detected. Had ceftazidime been the cause of the agranulocytosis, it would probably have recurred during the second course of treatment with ceftazidime. Moreover, ceftazidime-induced agranulocytosis has not been reported according to our closed survey by Medline, although it has been reported as a complication of some cephalosporins, which produced rare instances of myelosuppression, characterized by granulocytopenia10,11). Agranulocytosis induced by aztreonam has not been reported either, but one case of aztreonam-induced neutropenia was reported in 199112). Thus, we consider that vancomycin was the cause of agranulocytosis in our patient.
Vancomycin-induced agranulocytosis is a rare complication of vancomycin therapy, and has rarely been reported. However, the condition may occur more frequently in the future, because of the increased use of this antibiotic in ESRD patient on CAPD. Neutropenia related with vancomycin therapy is usually observed after relatively long courses of vancomycin therapy. In most reported cases, neutropenia was not detected 15ŌĆō40 days after the initiation of vancomycin therapy, and resolved spontaneously within a few days of vancomycin discontinuation1, 2, 9)
However, according to previous reports, the clinical features of vancomycin-induced neutropenia in ESRD patients on hemodialysis differ from those in patients with normal renal function, as the neutropenia persisted for up to 4 weeks despite vancomycin withdrawal, in addition, the appearance of agranulocytosis was delayed after the initiation of vancomycin therapy13ŌĆō15). Prolonged neutropenia may be associated with the non-removal of vancomycin by dialysis, and its long half-life. In addition, agranulocytosis or neutropenia is a more serious condition in ESRD patients than in non-uremic patients, because of the comorbidities related to ESRD. Renal insufficiency is associated with a poor prognosis in drug-induced agranulocytosis. Therefore, it is important to shorten the duration of agranulocytosis in ESRD patients3). It had been reported that G-CSF therapy shortens the duration of drug-induced agranulocytosis5ŌĆō8). Indeed, agranulocytosis developed on the 82th day of vancomycin therapy in our patient, and the agranulocytosis was rapidly resolved by G-CSF therapy and by the discontinuation of possible causative medications.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





