INTRODUCTION
The Chinese bellflower (Platycodon grandiflorum, family Campanulaceae), also known as the balloon flower, or doraji, in Korean, is distributed throughout the wilderness of northeast Asia, including Korea, Japan, and China. It is cultivated for food and medical purposes. In Korea, people usually gather Chinese bellflower roots in spring and autumn to use in seasoned salads or as a cooked potherb. In addition, because it is known to have a mucolytic and antitussive effect, Chinese bellflower is used in Oriental medicine for the treatment of acute or chronic bronchitis, tonsillitis, and asthma [1]. Although widely used in Asian countries, food allergy to Chinese bellflower, especially anaphylaxis, had not been previously reported. We describe a case of anaphylaxis induced by Chinese bellflower, its IgE-binding components, and a possible cross-reactivity with mugwort (Artemisia vulgaris) and birch.
CASE REPORT
A 56-year-old man experienced recurrent generalized urticaria and an oral burning sensation after eating several cooked herbs for 3 months. He, however, did not know the exact cause of his symptoms. The patient also complained of rhinorrhea and sneezing that occurred in spring and autumn and stated that his mother suffered from asthma. His serum total IgE level was elevated (375 IU/mL) and the eosinophil count in his peripheral blood was 222 cells/┬ĄL. A skin prick test with common inhalant and food extracts showed a positive response (allergen/histamine ratioŌēź1 and wheal sizeŌēź3 mm) to the two-spotted spider mite; various tree, grass, and weed pollens (birch, beech, oak, velvet, orchard, rye, timothy, kent, mugwort, chrysanthemum, and dandelion); and several food extracts (celery, Chinese bellflower, and arrowroot). He denied arrowroot intake, and oral provocation with raw, unprocessed celery and Chinese bellflower was conducted to identify the cause of urticaria in an open-challenge manner using careful, incremental dosing and a low starting dose [2]. Celery did not provoke urticaria or any other symptoms, but during the oral provocation test with Chinese bellflower, the patient complained of a burning sensation in the oral cavity and on his face and both hands, as well as itching in both ears and in the parietal area that was later generalized to his entire body. Physical examination revealed soft palate erythema, mild eyelid swelling with erythema, and subsequent generalized multiple urticarias throughout his entire body. Forty-five minutes after the study, 45.5 mg of pheniramine maleate and 40 mg of methylprednisolone were administered parenterally to control his symptoms. However, he complained of dizziness 4 hours after the study and his systolic and diastolic blood pressures were found to be 70 and 50 mmHg, respectively. Epinephrine (0.3 mL, 1:1000) was injected intramuscularly once and his blood pressure recovered.
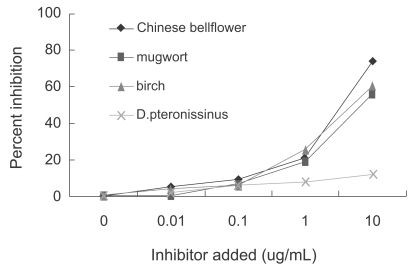
The presence of specific IgE antibody to Chinese bellflower was determined by ELISA and its specific IgE-binding components were analyzed by SDS-PAGE and immunoblot assay using the patient's serum according to a previously described method [3]. The Chinese bellflower-specific IgE ELISA OD value was 1.547. An ELISA inhibition test was performed to determine the specificity of IgE binding to Chinese bellflower antigen as previously described [3]. Significant inhibition of IgE binding to Chinese bellflower extract was observed in response to the addition of Chinese bellflower, mugwort, and birch pollen extract. This occurred in a dose-dependent manner, although it was not inhibited by the addition of the European house dust mite, Dermatophagoides pteronyssinus (Fig. 1).
Analysis using 12% SDS-PAGE and an immunoblot assay with Chinese bellflower revealed the presence of nine IgE-binding components (14, 17, 22, 30, 33, 45, 55, 65, and 170 kDa) in the patient's serum that were not found in the control sera. Immunoblot with Chinese bellflower, mugwort, and birch pollen extract revealed common protein bands binding to the patient's serum IgE antibody in the range of 40~55 kDa. Another common protein band was also detected in the 14 kDa area between Chinese bellflower and birch (Fig. 2).
DISCUSSION
In areas of northeast Asia such as Korea, China, and Japan, various herb roots are widely used for food and medicine, and a few cases of food allergy induced by the ingestion of herbs, including arrowroot and ginseng, have been reported [4,5]. However, no food allergies to the Chinese bellflower had to date been reported; to the best of our knowledge, this is the first report of anaphylaxis induced through ingesting Chinese bellflower root and its IgE-binding components.
In the ELISA inhibition assay, which was performed to investigate the IgE-binding specificity of Chinese bellflower, we found that the IgE binding of Chinese bellflower was inhibited by mugwort and birch, both of which showed positive responses to the skin prick test, indicating possible cross-reactions between these substances. Although Chinese bellflower belongs to the family Campanulaceae and mugwort belongs to the Asteraceae, both belong to the order Asterales and they are systematically related [6]. Mugwort pollen contains several allergens, including Art v 1, Art v 2, Art v 3 (lipid transfer protein), and Art v 4 (profilin), and has IgE cross-reactivity with various kinds of food [7,8]. Pollen-related food allergy syndrome is a clinical entity that describes pollinosis and food allergy manifestation to fruits, vegetables, and spices such as in birch-fruit syndrome, celery-mugwort-spice syndrome, and latex-fruit syndrome. In pollen-related food allergy syndrome, various food ingestion symptoms occur according to the characteristics of specific allergens and their stability during the digestive process. These range from a mild oral reaction, typical of birch-fruit syndrome, to anaphylactic shock, which is not uncommon in celery-mugwort-spice syndrome [8]. Mugwort is an important weed pollen associated with pollen-food syndrome and is linked to various foods such as celery, carrots, Apiaceae spice, mustard, peaches, and mangos [8]. Art v 4 (profilin), Art v 3 (lipid transfer protein), and a high-molecular-weight allergen (40~60 kDa) are reported to be key molecules involved in the cross-reactions of mugwort and these foods [8]. Birch (genus Betula) is also an important pollen associated with food allergy, and more than 70% of individuals allergic to birch pollen develop allergic reactions to stone fruits, nuts, or certain vegetables [9]. The major birch allergen, Bet v 1, is the relevant sensitizing protein in these associations. However, minor allergens such as Bet v 2 (profilin), Bet v 5, and Bet v 6 are also involved [9]. Note that birch pollinosis and celery hypersensitivity share common antigenic determinants and this association with birch is very important in celery-mugwort-spice syndrome. Several spectra of allergens are known to be involved in celery-birch-mugwort-spice syndrome [8]. For example, Bet v 1 homolog senstitization is related to IgE reactivity to celery Api g 1. In addition, the pan-allergen profilin present in birch, Bet v 2, may display IgE cross-reactivity with celery Api g 4 and mugwort Art v 4 profilin. High-molecular-weight allergens and glycoallergens are also part of an important cross-reactive structure in this syndrome [8].
This patient suffered from seasonal rhinitis symptoms such as rhinorrhea and sneezing that were aggravated in the spring and autumn. Immunoblotting with Chinese bellflower, birch, and mugwort revealed a common 40~55 kDa protein band that was very similar to the high-molecular-weight allergen involved in celery-birch-mugwort-spice syndrome [8]. Although we did not identify this protein component and its immunologic activity, consideration of these experimental findings together with the patient's clinical manifestations suggest the possibility of another new type of pollen-food syndrome, such as a birch-mugwort-Chinese bellflower association or a celery-birch-mugwort-Chinese bellflower association. The 40~55 kDa high-molecular-weight protein is presumably related to this association. Another common band protein between Chinese bellflower and birch was detected in the 14 kDa area, which may be a profilin. However, further study is needed to show the nature of the cross-reactive protein bands, including analysis of the amino acid sequence.
In summary, Chinese bellflower root may cause a severe systemic allergic reaction after ingestion including anaphylaxis, and it may have cross-reactivity with mugwort and birch pollen.




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





