INTRODUCTION
Myasthenia gravis (MG) is a chronic autoimmune neuromuscular disease. MG is characterized by autoantibody attack of acetylcholine receptors at the motor end plate of striated muscles, which results in variable muscle weakness made worse by exercise [1]. Patients with MG commonly experience respiratory failure. However, most patients have respiratory failure during the late course of MG and usually have additional neurological symptoms. We treated a woman with MG who presented with isolated respiratory failure as the first symptom of MG. Here we report this case.
CASE REPORT
A 68-year-old woman presented to the emergency department with dyspnea for one week. She denied a cough, sputum, chest pain or other respiratory symptoms. She also denied symptoms of upper and lower extremity weakness, blurred vision or swallowing difficulty. Sixteen years previously, she was diagnosed with diabetes mellitus, hypertension and depression. Eleven years ago, she underwent total thyroidectomy for a papillary thyroid carcinoma. The patient was taking selective serotonin reuptake inhibitor, zolpidem, alprazolam and methylphenidate for insomnia and depression, levothyroxin and alfacalcidol for thyroid disease, a calcium channel blocker for hyper-tension, and sulfonylurea and metformin for type 2 diabetes mellitus.
On the initial physical examination, the patient was not in acute respiratory distress. The vital signs were normal: blood pressure was 170/90 mmHg, pulse rate was 92 beats/min, respiratory rate was 24 breaths/min, and body temperature was 36℃. The mental status was intact, the patient was alert and the neurological examinations of cerebral function, cerebellar function and both extremities were normal. Pretibial pitting edema and neck vein engorgement were absent. On the chest auscultation, there were mild crackles at both lower lung fields. The body mass index was 24.2 kg/m2.
The laboratory evaluation showed a white blood cell count of 6,580/µL, hemoglobin of 12.0 g/dL and platelet count of 325,000/µL. Other blood chemistries were within normal limits: BUN/Cr 12.2/0.9 mg/dL, AST/ALT 25/25 units/L, NT-proBNP 107.2 pg/mL, and glucose 92 mg/dL. Thyroid function testing showed: T3 0.73 ng/mL, FT4 1.71 ng/dL and TSH < 0.003 µIU/mL. The arterial blood gas analysis, on room air, was pH 7.441, PaCO2 39.9 mmHg, PaO2 64.7 mmHg, oxygen saturation 93.2%, and D(A-a)O2 36.
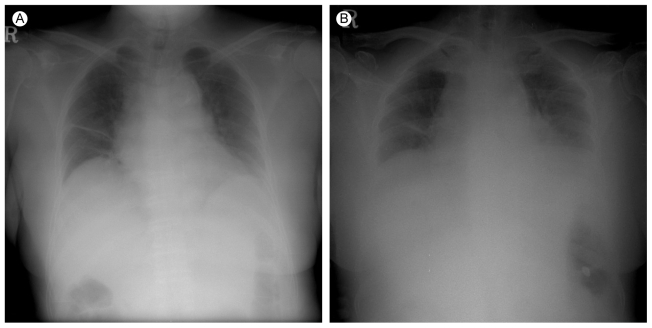
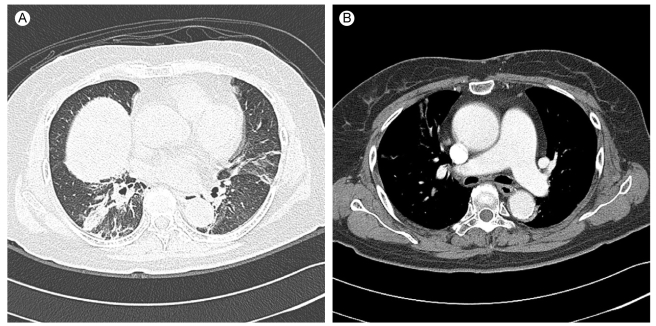
The initial chest X-ray showed a slightly reduced lung volume (Fig. 1A). The chest computed tomography (CT) scan showed no evidence of pulmonary thromboembolism, but there was bibasilar atelectasis (Fig. 2). Echocardiography revealed normal systolic and diastolic heart function.
During the next five days, her dyspnea became more severe. On the sixth day of hospitalization, the patient had severe respiratory distress with labored breathing. The respiratory rate was 40 breaths/min and the mental status was confused. The arterial blood gas analysis on an O2 mask with 10 L was pH 7.324, PaCO2 54.9 mmHg, PaO2 94.4 mmHg, and oxygen saturation 96.6%. The chest X-ray revealed no definite infiltration but the lung volume was reduced (Fig. 1B). The patient was transferred to the intensive care unit and mechanically ventilated.
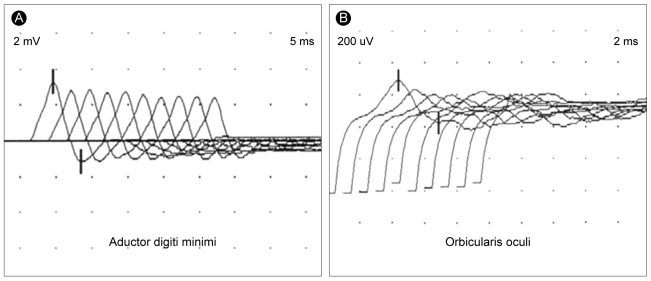
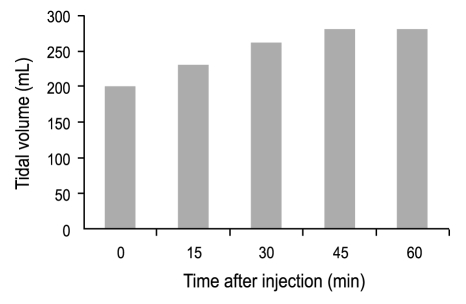
We considered other causes of respiratory failure such as neuromuscular disorders, Guillain-Barre syndrome or myasthenia gravis. The physical and neurological examination and cerebrospinal fluid analysis were normal. A diagnosis of MG was made based on the neurophysiological studies. The electromyography showed a decrement in response to repetitive nerve stimulation in various muscles (Fig. 3). The pharmacological Jolly test revealed incremental responses of tidal volume of ventilation (Fig. 4). The repeated acetylcholine antibody titers were 8.9 nmol/L and 12.4 nmol/L.
Pyridostigmine bromide, 720 mg/day and prednisolone, 30 mg/day was prescribed and intravenous gamma-globulin, 27 g/day for 5 days were administered. Weaning from the ventilator failed over the next 2 weeks; therefore, a tracheostomy was performed. However, the patient was eventually successfully weaned from the ventilator and 2 months later, she was discharged.
DISCUSSION
MG is an autoimmune disorder. In about two thirds of patients, extrinsic ocular muscle abnormalities present as the initial symptoms or bulbar weakness may also be the initial symptoms. The symptoms usually progress to include the limb muscles [1]. Respiratory failure can be a complication during the late course of MG in about 3 to 8% of cases, known as a myasthenic crisis [2]. However, isolated respiratory failure as the presenting symptom, as in the present case, is very unusual and this patient is the first case reported in Korea.
Recently, several cases of MG with respiratory failure as a first manifestation have been reported [3-6]. In these studies, respiratory failure as an initial symptom was observed in 14 to 18% of the patients. Most of the patients presented with ocular and bulbar muscle involvement [7]. However, our patient showed no other neurological symptoms associated with MG. Therefore, we did not suspect MG initially. We tried to determine the cause of the respiratory failure. We did not find any evidence of a hypoxemic respiratory failure; there were no definite infiltrations, edema, effusion or pneumothorax on chest X-ray. There was no evidence of pulmonary thromboembolism on the chest CT scan and no evidence of intracardiac shunting or congestive heart failure on the echocardiography. Therefore, we suspected an acute ventilatory failure. Drugs or trauma that could cause ventilatory failure was ruled out. The electrolyte levels were within normal limits. Based on these results, we investigated the possibility of a neuromuscular disease, especially Guillain-Barre syndrome and myasthenia gravis, the most common and the second most common cause of neuromuscular disease, respectively. However, the cerebrospinal fluid was normal, and the neurophysiological studies showed evidence of myasthenia gravis.
Generally patients with neuromuscular disease present with hypoxia and a normal D(A-a)O2 due to hypoventilation, but in the present patient there was an increased D(A-a) O2. Patients with MG occasionally have atelectasis [8], which could result in this finding.
The patient had negative results on multiple tests for the evaluation of respiratory failure. It is difficult to consider a neuromuscular disorder, especially myasthenia gravis, unless there are other neurological symptoms such as ocular or bulbar symptoms. Unlike previous cases, our patient presented with only respiratory symptoms, the patient had no other symptoms generally associated with MG during her 6-month follow-up visits.
We report the case of a 68-year-old woman who presented with respiratory failure as the only symptom of myasthenia gravis. As seen in this case, MG can manifest as isolated respiratory failure. Therefore, one should consider neuromuscular disorders in cases of unexplained respiratory failure.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





