 |
 |
| Korean J Intern Med > Volume 27(2); 2012 > Article |
|
To the Editor,
Toxoplasma gondii is an intracellular protozoan parasite. Immunocompetent persons with primary infection are usually asymptomatic, but latent infection can persist for the life of the host [1]. In immunocompromised patients, however, a risk exists of reactivating the infection, which may become life-threatening [1].
Toxoplasmosis appears to be a rare opportunistic infection after hematopoietic stem cell transplantation (HSCT). The most frequently involved organ was the central nervous system (CNS), with 48% of patients having isolated cerebral infection and 76% of patients with disseminated disease showing brain involvement. Little is known about toxoplasmosis after HSCT in Korea. Here, we describe a Korean patient with isolated cerebral toxoplasmosis following allogeneic HSCT.
A 37-year-old woman was admitted because of headache, myalgia, and fever. She had been well until 1 week before admission, when her headache developed. Myalgia and fever occurred 5 days before admission and her headache worsened. Fifty days prior to admission, she had undergone HLA-matched sibling, non-T cell-depleted allogeneic HSCT for aplastic anemia. Her conditioning regimen included cyclophosphamide (50 mg/kg a day for 4 consecutive days) and antithymocyte immunoglobulin (3 mg/kg a day for 3 consecutive days), and prophylaxis against graft-versus-host disease (GVHD) consisted of short-course methotrexate (15 mg/m2 on day 1 and 10 mg/m2 on days 3, 6, and 11) and cyclosporine (4 mg/kg beginning 1 day before transplant). The pre-transplant T. gondii serostatus of both donor and recipient was not known, but the recipient had been treated with clindamycin for toxoplasma uveitis 10 years previously, at which time she was initially positive for toxoplasma IgM and negative for IgG, but became IgG-positive 5 months later.
Soon after HSCT (day 40, 2 weeks before admission), she developed grade II acute GVHD of the skin, and immunosuppressive therapy (i.e., methyl prednisone 48 mg) was started. At the same time, gancyclovir (10 mg/kg/day) therapy was initiated because she was cytomegalovirus (CMV) antigenemia-positive (41/200,000 white blood cells). Fluconazole and acyclovir were administered as prophylaxis against candidiasis and herpes simplex infection, and pentamidine nebulizer was administered once monthly as prophylaxis against Pneumocystis jirovecii.
On admission (day 57), her blood pressure was 124/84 mmHg, her pulse was palpable at 94 beats per minute, and her temperature was 38.8Ōäā. At admission, she had a white blood cell count of 1,200/mm3 with an absolute neutrophil count of 880/mm3, a hemoglobin level of 9.2 g/dL, a hematocrit of 30.6%, a platelet count of 59,000/mm3, and a C-reactive protein concentration of 4.29 mg/dL. She took methyl prednisone 6 mg, which had been tapered from the initial dose of 48 mg, for treatment of acute GVHD. Brain magnetic resonance imaging (MRI) revealed focal high signal intensity (SI) in the right caudate nucleus and right thalamus on T2 weighted images and combined subtle ring-enhancement of the lesions (Fig. 1A and 1B). Toxoplasma serology revealed an equivocal IgG titer (7 IU/mL) and negative IgM titer on hospital day (HD) 1. She was negative for serum galactomanan. A lumbar puncture yielded clear cerebrospinal fluid (CSF) with a white blood count of 2/mm3, including 3% neutrophils and 63% lymphocytes, a protein concentration of 24 mg/dL, and a glucose concentration of 72 mg/dL. Bacterial, fungal, and mycobacterial cultures of her CSF were negative. Microbiologic or molecular tests in CSF for viruses such as herpes simplex virus, human herpes virus-6, CMV, and Epstein-Barr virus were not performed because multiple ring-enhancing lesions are unusual in viral encephalitis. Ophthalmic examination revealed only pseudophakia in the right eye and no evidence of inflammation. Bronchoalveolar lavage was not performed because chest computed tomography (CT) showed no abnormal findings in lung parenchyma and lymph nodes. Abdominal CT and electrocardiogram showed nonspecific findings, except underlying Woff-Parkinson-White syndrome. On HD 4, her serum was tested for T. gondii using an in-house specific polymerase chain reaction (PCR) assay [2]. She began empirical treatment with meropenem + vancomycin + itraconazole and pyrimethamine (200 mg loading then 75 mg daily) + sulfadiazine (6 g daily) for T. gondii. On HD 11, 6 days after initiation of anti-toxoplasma therapy, her headache had slightly improved, and MRI of her brain showed that the lesions in the right caudate nucleus and right thalamus had decreased in size. On HD 15, serum PCR amplification of the sample taken on HD 4 showed T. gondii-specific bands (Fig. 2 and 3). We therefore discontinued other antibiotics and antifungal agents and continued antitoxoplasma therapy only. T. gondii-specific bands were not detected 10 days after initiation of anti-toxoplasma therapy.
Because MRI of the brain showed that the lesions had nearly disappeared 50 days after initiation of anti-toxoplasma therapy (Fig. 1C and 1D) and her headache had mostly improved, she was discharged from the hospital and continued maintenance anti-toxoplasma therapy with pyrimethamine (50 mg daily) + sulfadiazine (3 g daily) for 2 months, and trimethoprim-sulfamethoxazole (TMP-SMX) (5-25 mg/kg/day) for 10 months. Twelve months later, all symptoms related to toxoplasmosis had disappeared.
HSCT has been associated with several neurologic complications secondary to the underlying disease and to prolonged myelosuppression. The most common neurologic complications are CNS infection, marked by early onset within the first 4 months after HSCT (87%), diagnostic difficulties, and a high mortality rate (47%). These infections consisted primarily of cerebral toxoplasmosis, fungal infections, and viral encephalitis [3].
Humans can acquire toxoplasmosis in four ways: ingestion of infectious oocytes from the environment (usually from soil contaminated with feline feces), ingestion of tissue cysts in meat from an infected animal, vertical transmission from an infected mother to her fetus, and blood transfusion or organ transplantation from an infected donor [1]. Our patient had anti-toxoplasma IgG antibody prior to HSCT, and she had grown up with many animals in her garden, including cats. Since the pre-transplant T. gondii serostatus of both donor and recipient was not known, whether in this case toxoplasmosis was due to reactivation of a latent infection or primary infection from an infected donor is unclear.
Diagnosis of toxoplasmosis in transplant recipients is often difficult because of the nonspecific signs and symptoms of the infection. Sensitive and specific noninvasive methods for detection of T. gondii are needed, since invasive procedures in HSCT recipients carry a high risk of complications. In our patient, stereotactic brain biopsy was attempted for histological assessment, but failed because the lesions were located in vital regions of the brain or inaccessible to biopsy, as well as being small enough to render biopsy infeasible.
PCR techniques have been developed for noninvasive diagnosis of cerebral toxoplasmosis in patients with acquired immune deficiency syndrome (AIDS), and have contributed to the rapid diagnosis and monitoring of treatment efficacy and may improve patient outcomes [4]. PCR analysis of the serum of our patient showed initial positivity for T. gondii, with negativity observed 10 days after initiation of anti-toxoplasma therapy. According to the proposed definitions for toxoplasmosis after HSCT [5], the diagnosis in our patient was probable toxoplasma disease, defined as clinical and radiologic evidence suggestive of organ involvement plus at least one positive PCR test from blood, CSF, or bronchoalveolar lavage, but no histology confirmation, and absence of another pathogen that may explain findings. Although histological confirmation failed in this case, tissue biopsy for histological assessment is necessary for confirmation in patients with suspected cerebral toxoplasmosis.
Another noninvasive diagnostic method is MRI. Most neuroradiological studies on toxoplasma have been performed in patients with AIDS, with typical findings including multiple, ring-enhancing brain lesions often associated with edema. However, CNS lymphoma and other infections, including cryptococcus, aspergillosis, and tuberculosis, should be differentiated as they cause similar lesions [2].
Prophylaxis prior to HSCT should be considered for all recipients who are seropositive for toxoplasma and have risk factors for reactivation (e.g., GVHD). TMP-SMX or pyrimethamine/sulfadoxine prophylaxis may be effective in preventing T. gondii and P. jirovecii infection. In two patients from Korea, including this one and another with bilateral toxoplasma choroidoretinits after allogeneic HSCT, a monthly pentamidine inhalation was prophylactic against P. jirovecii after HSCT, but this agent has no effect on T. gondii. Given that our patient had previous toxoplasma uveitis with positive anti-toxoplasma IgG antibody 10 years prior to HSCT, such a prophylactic regimen was inappropriate. After our experience with these two patients with cerebral toxoplasmosis after allogeneic HSCT, the prophylaxis regimen in our hospital changed from a pentamidine nebulizer to TMP-SMX.
In summary, we describe here a Korean patient with cerebral toxoplasmosis following HSCT. This patient was diagnosed with probable cerebral toxoplasma disease by clinical and radiologic evidence suggestive of brain involvement and a positive blood PCR test.
References
1. Tenter AM, Heckeroth AR, Weiss LM. Toxoplasma gondii: from animals to humans. Int J Parasitol 2000;30:1217ŌĆō1258PMID : 11113252.



2. Luft BJ, Hafner R, Korzun AH, et al. Toxoplasmic encephalitis in patients with the acquired immunodeficiency syndrome: members of the ACTG 077p/ANRS 009 study team. N Engl J Med 1993;329:995ŌĆō1000PMID : 8366923.


3. Denier C, Bourhis JH, Lacroix C, et al. Spectrum and prognosis of neurologic complications after hematopoietic transplantation. Neurology 2006;67:1990ŌĆō1997PMID : 17159106.


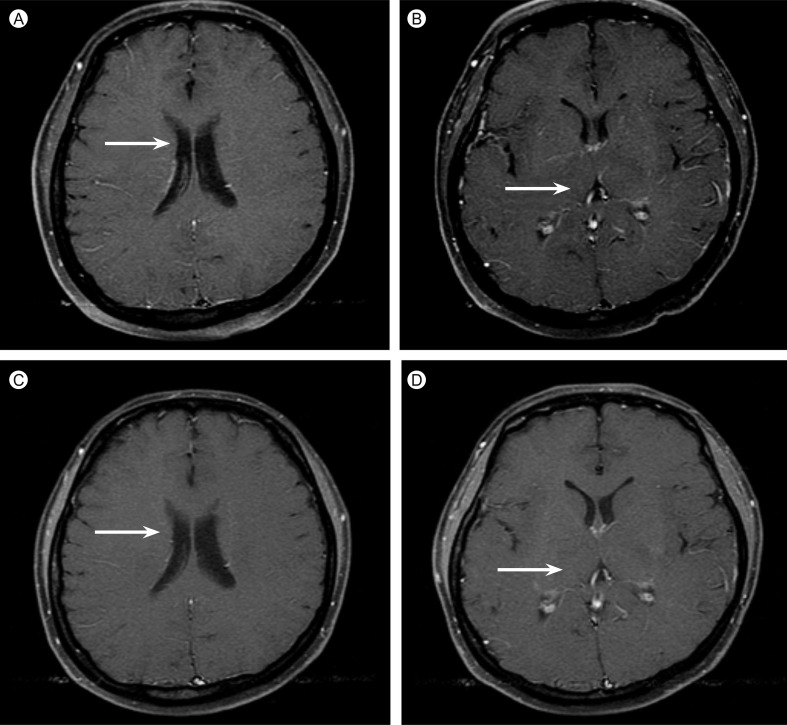
Figure┬Ā1
Magnetic resonance imaging of the brain. Focal high signal intensity in the right caudate nucleus (A) and the right thalamus (B) on combined subtle ring-enhancement of the lesions was observed. Fifty days after initiation of anti-toxoplasma therapy, the lesions had nearly disappeared (C and D).
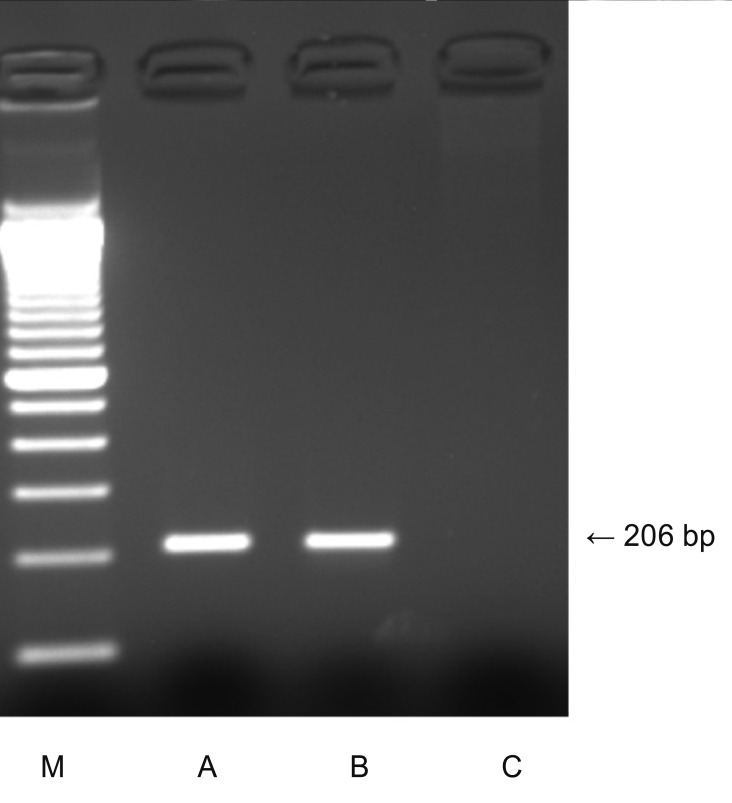
Figure┬Ā2
Polymerase chain reaction analysis for detection of Toxoplasma gondii. M, DNA marker; A, positive control; B, patient; C, negative control.
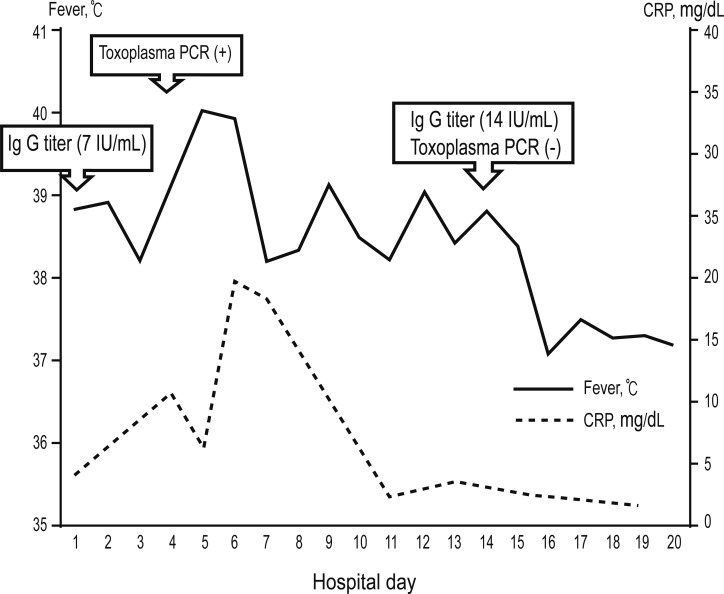
Figure┬Ā3
Flowchart of the patient's clinical progress. Fever and C-reactive protein (CRP) decreased after initiation of anti-toxoplasma therapy, antibiotics, and antifungal agents. Only anti-toxoplasma therapy was continued after confirmation by Toxoplasma gondii-specific polymerase chain reaction (PCR). T. gondii-specific bands were not detected 10 days after initiation of anti-toxoplasma therapy.
-
METRICS

-
- 0 Crossref
- 1 Scopus
- 8,923 View
- 73 Download
- Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print


