INTRODUCTION
Hepatitis C virus(HCV) which leads to chronic liver diseases, including liver cirrhosis and hepatocellular carcinoma in most cases1,2), is a single-stranded RNA virus and similar to pestivirus and flavivirus in the genomic structure. HCV contains a long open reading frame(ORF) encoding a polyprotein of approximately 3000 amino acids which is subsequently cleaved via the proteolytic process to yield smaller functional proteins, core(C), envelopes(E1 and E2/NS1) and six nonstructural proteins (NS2, NS3, NS4A, NS4B, NS5A and NS5B)3,4). Although theoretically, these functional proteins should be generated equivalently, individually processed functional proteins have shown the discrepancies in the eliciting immune response and/or its time of appearance following infection5). To detect HCV antibodies, immunoassays are developed and are utilized primarily in clinical settings. However, as a confirmation of the HCV infection with diversity for diagnosis6,9), recombinant immunoblot assay(RIBA) and reverse transcription-polymerase chain reaction(RT-PCR) are employed.
HCV genotype and HCV RNA replication have been extensively studied in their relationship to clinical backgrounds. Recently, Simmonds et al. proposed the classification of HCV variants into six major genotypes (types 1 to 6) and further subtypes10). Previously, we demonstrated that the prevalent HCV genotypes in Korean patients with HCV infection were that of genotype 1b and followed by genotype 2a11,12). It has previously been reported that HCV genotype may be an important factor influencing the natural course of chronic liver disease and the response to interferon(IFN) therapy in chronic hepatitis C13ŌĆō16). HCV RNA titers which reflect HCV replication is also another virological factor affecting the efficacy to IFN therapy, antibody response to HCV proteins and persistent infection following liver transplantation14,17,18).
In this study, we investigated antibody responses to regional specific proteins of HCV in relationship to HCV replication and HCV genotypes.
MATERIALS AND METHODS
1. Subjects
We studied a total of forty-five patients with chronic HCV infection, consisting of 30 males and 15 females between the age of 25 to 76. All of the patients were positive for both anti-HCV and HCV RNA, and were negative to hepatitis B surface antigen (HBsAg). None of the patients showed any evidence of autoimmune, drug-induced or alcoholic liver disease. All patients, consisting of 33 chronic hepatitis(CH) and 12 hepatocellular carcinoma(HCC), were diagnosed by liver biopsy.
2. Methods
Serological Assays
Anti-HCV assay was determined by second-generation enzyme immunoassay (Abbott Laboratories, Chicago, ILL., USA). HBsAg was tested with a radioimmunoassay (Abbott Laboratories, Chicago, ILL, USA). The antibodies to the four recombinant HCV antigens, C22-3, C33C, C5-1-1 and C100-3, immobilized as individual bands on nitrocellulose strips, were detected in the RIBA-2 test (Ortho Diagnostic System Co., Ltd. Tokyo, Japan). This assay was performed according to the manufacturerŌĆÖs instructions. The immunoreactivity to each recombinant protein was determined visually by comparing the intensity of each band with that of two internal control bands (high and low IgG) incorporated in each strip. The intensity was expressed (ŌłÆ), (+/ŌłÆ) as negative and (+1 to +4) as positive.
Detection of seum HCV RNA
HCV RNA was extracted from 100 ╬╝ L of serum as described previously19). After synthesis of cDNA with Moloney Murine Leukemia Virus reverse transcriptase (MMLV-RT, GIBCO BRL, Gaithersburg, MD, USA) from HCV RNA samples, double-nested PCR was carried out using two sets of primers deduced from highly conservative 5ŌĆ▓-untranslated region (5ŌĆ▓-UTR) of HCV19). The sequences of the primers used were: 5ŌĆ▓-CTG TGA GGA ACT ACT GTC TT-3ŌĆ▓ (sense, nucleotides 28 to 47) and 5ŌĆ▓-CTG TGA GGA ACT ACT GTC TT-3ŌĆ▓ (antisense, nucleotides 229 to 248) as an outer primer set; 5ŌĆ▓-TTC ACG CAG AAA GCG TC TAG-3ŌĆ▓ (sense, nucleotides 46 to 65) and 5ŌĆ▓-GTT GAT CCA AGA AAG GAC CC-3ŌĆ▓ (antisense, nucleotides 171 to 190) as an inner primer set.
HCV Genotyping
HCV genotypes were determined with type specific primers on second round PCR following first amplification of the NS5 gene with universal primer pair as described elsewhere20,21). The nomenclature of HCV genotype was expressed according to the scheme proposed by Simmonds et al.10). The oligonucleotide primer sequences that were used are listed here: universal primers, sense-5ŌĆ▓-TGG GGA TCC CGT ATG ATA CCC GCT GCT; universal primers, antisense- 5ŌĆ▓-GGC GGA ATT CCT GGT CAT AGC CTC CGT GAA-3ŌĆ▓; genotype 1a, sense-5ŌĆ▓-CGA CAT CCGT ACG GAG GAGG-3ŌĆ▓; genotype 1a, antisense-5ŌĆ▓-CAG GCT GCC CGG GCC TTG AT-3ŌĆ▓; genotype 1b, sense-5ŌĆ▓-TGA CAT CCG TGT TGA GGA GT-3ŌĆ▓; genotype 1b, antisense-5ŌĆ▓-CGG GCC GCA GAG GCC TTC AA 3ŌĆ▓; genotype 2a, sense-5ŌĆ▓-TAT GTT CAA CAG CAA GGG CCA GA-3ŌĆ▓; genotype 2a, antisense-5ŌĆ▓-CCT GGT CAT AGC CTC CGT GAA-3ŌĆ▓. The 10╬╝L of synthesized cDNA was amplified on double nested PCR as described previously11). The product of the nested PCR was electrophoresed in 1% agarose gels, and HCV genotypes were identified by the length of the amplified sequence.
Quantification of serum HCV RNA level
Serum HCV RNA level was quantified by a competitive RT-PCR using a synthetic mutant HCV RNA as a competitive template, which was kindly provided by Dr. Ryu W-S (Biotech Research Institute, LG Chemical Ltd/Research Park, Taejon, Korea). Briefly, HCV RNA was extracted from 50 ╬╝L of serum as described above. cDNA was synthesised by reverse transcription; following that, an equal amount of sample RNA was put into a set of microtubes that already had serially 10-fold diluted mutant RNA plus annealing mixture, including primer KL70. After cDNA synthesis, second stage PCRs were performed. The sequences of primers used were: HCV QC1, sense-5ŌĆ▓-CCA CCA TAG ATC ACT CCC CTGT-3ŌĆ▓ and HCVL70, antisense-5ŌĆ▓-TTG AGG TTT AGG ATT CGT GCT CAT-3ŌĆ▓ for first PCR; HCVQC2, sense-5ŌĆ▓-CTG TGA GGA ACT ACT GTC TTCA-3ŌĆ▓ and HCVQC3, antisense-5ŌĆ▓-ACT CGC AAG CAC CCT ATC AGGC-3ŌĆ▓ for second PCR. The first PCR was carried out for 40 cycles of steps at 95┬░C for 1 min, at 55┬░C for 1 min and at 72┬░C for 2 min, and then the second PCR was carried out for 25 cycles of steps at 94┬░C for 1 min, at 55┬░C for 45 seconds and 1 min at 72┬░C. A 10╬╝l of second PCR products was analyzed by electrophoresis on 2.5% agarose gel containing ethidium bromide and visualized by ultraviolet trans illuminator. The titer of circulating HCV RNA was defined log10 (copy numbers of HCV RNA per milliliter of serum).
RESULTS
All sera from the forty-five patients with chronic HCV infection were tested for antibodies to regional specific HCV peptides by RIBA-2. The frequencies of seropositivity to the four antigens were 91.1%, 91.1%, 64.4% and 53.3% directed to C22-3, C33C, C100-3 and 5-1-1, respectively.
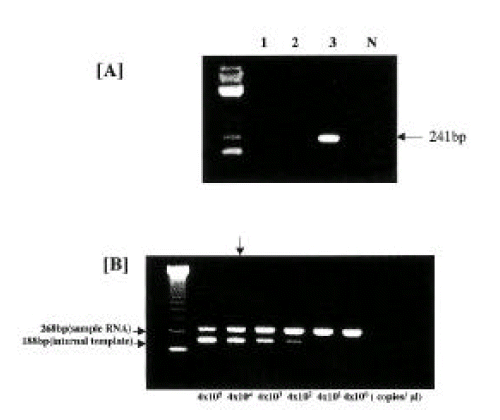
The clinical characteristics were compared between the positive group and the negative group for antibody response to each regional specific protein (Table 1). No significant difference was seen in sex or age between each pair of groups. The antibody responses between core or NS3 proteins and NS4 proteins showed more discrepancy in the HCC group than that in the CH group. HCV genotypes following HCV RNA detection were determined in the HCV RNA-positive sera. Each genotype was identified by the size of amplified fragments of the second PCR products: 216 bp for genotype 1a, 216 bp for genotype 1b and 241 bp for genotype 2a (Figure 1A). Of the forty-five patients, twenty-four patients (53.4%) were infected with genotype 1b, twenty (44.4%) with genotype 2a and one (2.2%) with undetermined genotype, respectively.
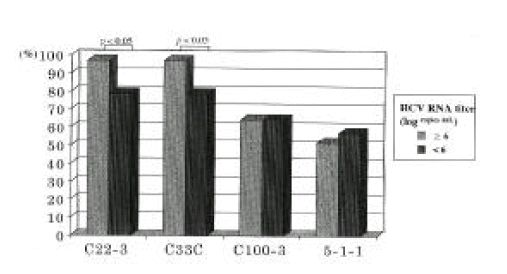
Circulating HCV RNA levels through competitive RT-PCR assay were determined by comparing the signal intensities of two bands on agarose gel electrophoresis, as shown in Figure 1B. Amplified PCR products derived from the target HCV RNA in sera and the mutant HCV RNA as internal template were 268 base pairs (bp) and 188bp respectively. In this study, the logarithmic HCV RNA levels varied from 4 to 8 copies/mL of serum. Serum HCV RNA levels in CH and HCC group were 6.36┬▒0.81 and 6.12┬▒0.83 copies/mL, respectively, but no significant difference was seen in both groups. The antibodies to C22-3, C33C, C100-3 and 5-1-1 were detected in 41 of 45 (91.1%), 41 of 45 (91.1%), 29 of 45 (64.4%) and 24 of 45 (53.3%), respectively. In regard to the frequency of antibodies detected according to HCV viremic levels in the sera, the detection rate of antibodies to C22-3, C33C, C100-3 and 5-1-1 was 96.8%, 96.8%, 64.5% and 51.6%, respectively in 31 patients with high viremic levels of 106 copies/mL, whereas in 14 patients with low viremic levels of <106 copies/mL, was 78.6%, 78.6%, 64.3% and 57.1%, respectively. From these results, seropositivity of antibodies to C22-3 and C33C was higher than those to C100-3 and 5-1-1 in all of the patients. Furthermore, each seropositivity of antibody to C22-3 and C33C showed a significant difference between patients with high HCV titers and with low HCV titers(p<0.05). However, no significant difference in each seropositivity of antibody to C100-3 and 5-1-1 was seen between both groups (Figure 2).
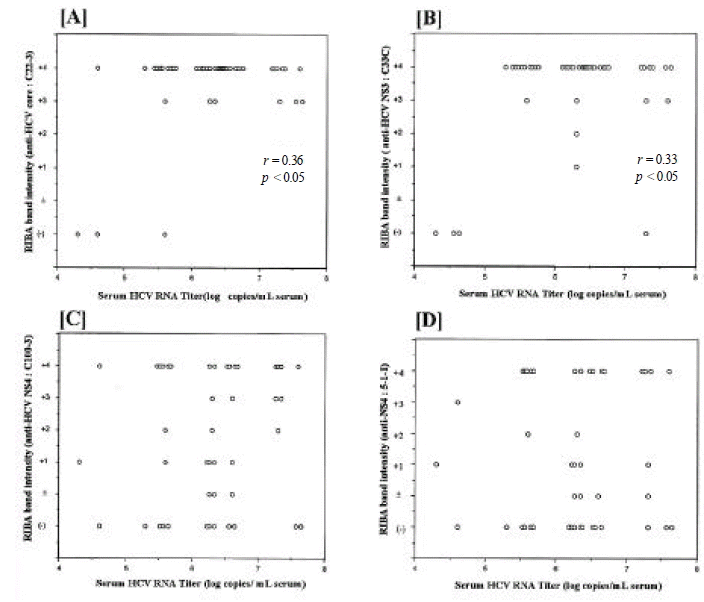
In regard to the reactivity of antibody in relation to serum HCV RNA levels, the intensity of antibodies to C22-3 and C33C in RIBA-2 test was closely correlated with the HCV RNA levels(r=0.36, p<0.05; r=0.33, p<0.05, respectively) (Figure 3A and B), but no correlation was seen between the intensity of antibodies to C100-3 and 5-1-1, and HCV RNA levels (Figure 3C and D). However, even in some patients with low HCV titers, antibodies to C22-3 and C33C strong intensity.
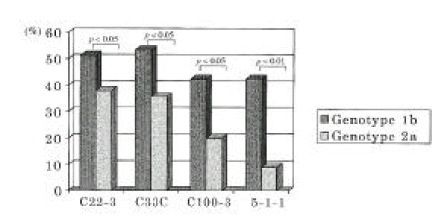
Serum HCV RNA level in patients with HCV genotype 1b and 2a was 6.48┬▒0.63 and 6.14┬▒0.81, respectively, among 44 patients whose HCV genotype was identified, but no significant difference was seen between both groups. As regards the frequency of antibodies to the four recombinant proteins in relation to HCV genotype, antibodies to C22-3 in HCV genotype 1b and 2a were found in 23 of 44 (52.3%) and 17 of 44 (38.6%), respectively. Antibodies to C33C in HCV genotype 1b and 2a were detected in 24 of 44 (54.5%) respectively, antibodies to C100-3, 19 of 44 (43.2%) and 9 of 44 (20.5%) respectively and antibodies to 5-1-1, 19 (43.2%) and 4 of 44 (9.1%) respectively (Figure 4). From these results, antibody response to each regional specific protein was correlated with the HCV genotype.
DISCUSSION
It has been reported that the molecular characteristics of HCV is closely related to important clinical issues, such as serodiagnosis22,23), the natural course of HCV-related chronic liver diseases13,24) outcome of interferon therapy25,26) and histological activity in chronic hepatitis C27,28).
Previous reports revealed the close correlation between the viremia and the presence of the HCV antibodies in chronic liver disease or asymptomatic HCV carriers17,29,30). Yuki et al. suggested that HCV antibodies might serve as sensitive markers for detecting HCV infection in chronic hepatitis C patients with a highly viremic level, but not sensitive enough for asymptomatic HCV carriers17).
In this study, we analyzed the antibody responses to regional specific proteins in the HCV genome in relation to virological characteristics of HCV under molecular level. In RIBA-2 test, the induction of HCV antibodies varied with each regional specific protein. The detection rate of the antibodies to C22-3 and C33C was higher than those to C100-3 and 5-1-1 in all the patients. In detail, HCV antibodies to C22-3 and C33C were detected in nearly all patients with high HCV viremic levels compared to those with low HCV viremic levels. However, the antibodies to C100-3 and 5-1-1 were found with similar percentages in both groups, irrespective of serum HCV RNA levels. Furthermore, a considerable number among patients with high viremic levels had poor antibody responses to NS4 protein. These results support previous findings that the HCV core and NS3 proteins are highly immunogenic compared to NS4 and NS5 proteins30,31). Also, well-conserved nucleotide sequence of a core region may contribute to the high induction of antibodies26,32). There are several reasons for poor detection of antibodies to NS4. The first is due to the diverse amino acid sequence in the NS4 region because the diversity in nucleotide sequences of the HCV genome may alter the antigenicity of viral proteins. The second is due to poor exposure to the host immune system. The third is due to its weak immunogenicity. Further study is needed to clarify this point. Interestingly, the seropositivity of antibodies to C22-3 and C33C was predominantly higher than that of antibodies to C100-3 and 5-1-1 in patients with HCC. However, this significant discrepancy was not observed in patients with chronic hepatitis. Therefore, these results imply that HCV core and NS3 protein may be related to hepatocarcinogenesis. Indeed, recent reports demonstrate that the HCV core protein had oncogenic potential in cooperation with the H-ras oncogene33) and that transgenic mice with HCC induced by HCV core protein were developed34). As regards NS3 protein in hepatocarcinogenesis, Sakamuro et al. reported that NIH3T3 cell was transformed to tumorigenic phenotype by the HCV NS3 protein and this transformation may be attributable to the proteinase activity of that protein35). However, its oncogenic role in hepatocarcingenesis is still controversial because it has not been demonstrated in the primary cells. Further study is required to address these mechanisms.
In Korea, two major HCV genotypes are genotype 1b and 2a, and genotype 1b is the more prevalent, followed by genotype 2a11). It has been reported that patients with genotype 1b have less sensitivity to interferon therapy than those with genotype 2a14,26). We have evaluated HCV replication and antibody responses in relation to the HCV genotype. Serum HCV RNA levels were not correlated with the HCV genotype, but the antibody responses to four recombinant proteins were more predominant in patients infected with genotype 1b than in those infected with genotype 2a, and these results were consistent with the previous study32). However, because the number of patients in this study was limited, further extensive study is required. Also, to confirm the HCV infection, RT-PCR techniques are necessary, because the antibody detection among lower viremic HCV carriers was less frequently detected. We quantified serum HCV RNA by competitive RT-PCR and this method was designed to overcome the drawbacks of the previously reported technique36,37). However, competitive RT-PCR assay is complicated, highly expensive and time-consuming and, therefore, an easier, less costly and time-saving method needs to be deveolped.
In conclusion, these results suggest that antibody detection of HCV may depend on the virological characteristics of HCV, the levels of HCV replication and HCV genotype and, therefore, HCV RNA detection using RT-PCR technique are necessary for confirmatory diagnosis of HCV infection. Furthermore the higher expression of HCV core or NS3 proteins compared to NS4 proteins in patients with HCC imply that the genes encoding such proteins may play a important role in hepatocarcinogenesis.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





