Middle East respiratory syndrome: what we learned from the 2015 outbreak in the Republic of Korea
Article information
Abstract
Middle East Respiratory Syndrome coronavirus (MERS-CoV) was first isolated from a patient with severe pneumonia in 2012. The 2015 Korea outbreak of MERSCoV involved 186 cases, including 38 fatalities. A total of 83% of transmission events were due to five superspreaders, and 44% of the 186 MERS cases were the patients who had been exposed in nosocomial transmission at 16 hospitals. The epidemic lasted for 2 months and the government quarantined 16,993 individuals for 14 days to control the outbreak. This outbreak provides a unique opportunity to fill the gap in our knowledge of MERS-CoV infection. Therefore, in this paper, we review the literature on epidemiology, virology, clinical features, and prevention of MERS-CoV, which were acquired from the 2015 Korea outbreak of MERSCoV.
INTRODUCTION
Middle East respiratory syndrome coronavirus (MERSCoV) was first isolated from a patient with severe pneumonia in September 2012 [1]. Since then, as of 31 January 2018, the World Health Organization (WHO) has been notified of 2,143 laboratory-confirmed cases of MERSCoV infection, including at least 750 deaths, from 27 countries (Fig. 1) [2]. Most of MERS-CoV human infections have occurred in the Arabian Peninsula. Saudi Arabia reported 1,783 cases, including 726 deaths (fatality rate, 40.7%) [3]. A recent article summarized the current knowledge on the epidemiology, virology, human pathogenesis, clinical management, and prevention of MERS-CoV infection [4]. Another comprehensive review article on risk factors and determinants of transmission of MERS-CoV from human to human in the community and hospital settings has been published recently [5]. Public Health England also published an extensive review of literature for clinical decision-making support for treatment of MERS-CoV patients [6].

Confirmed global cases of Middle East respiratory syndrome coronavirus reported to World Health Organization (WHO) as of November 17, 2017 (n = 2,103). Other countries: Algeria, Austria, Bahrain, China, Egypt, France, Germany, Greece, Iran, Italy, Jordan, Kuwait, Lebanon, Malaysia, the Netherlands, Oman, Philippines, Qatar, Thailand, Tunisia, Turkey, United Arab Emirates, United Kingdom, United States of America, Yemen. Adapted from World Health Organization [2].
The 2015 Korea outbreak of MERS-CoV is the largest outside the Arabian Peninsula and provides a unique opportunity to fill the gap in our knowledge about MERS-CoV infection. Since it has now been almost 3 years since the 2015 MERS outbreak in the Republic of Korea, we reviewed the literature to summarize the lessons we have learned from the Korea outbreak.
SEARCH STRATEGY
PubMed databases were searched for studies on MERS cases during the 2015 outbreak in the Republic of Korea. The search terms used were combinations of ‘Middle East respiratory syndrome’ in all fields and ‘Korea’ in all fields. As of 31 January 2018, a total of 221 articles were retrieved, and 216 of them were written in English. The full texts of the English articles were reviewed and critically assessed.
EPIDEMIOLOGY
Summary of the Korea outbreak
The 2015 Korea outbreak of MERS-CoV resulted in 186 cases including 38 fatalities [7]. The index case was a returning traveler from the Middle East. The infection had spread within the hospital, and subsequently to other hospitals because of patient movement, resulting in nosocomial transmission at 16 clinics and hospitals. The epidemic lasted for 2 months, with the government declaring a “virtual” end to the epidemic on July 6, 2015. In order to control the outbreak, the government quarantined 16,993 individuals for 14 days, and the economic loss was estimated at 9.311 trillion Korean won (8.5 billion US dollars) [8].
The first case of MERS
The first patient (index case) with MERS-CoV infection was a 68-year-old Korean man returning from the Middle East. He ran a commercial greenhouse business in Bahrain. He flew from Seoul to Bahrain on April 24, 2015, and traveled through the United Arab Emirate and the Kingdom of Saudi Arabia, and came back to Seoul on May 4, 2015. During his 10-day business trip, he did not visit a camel farm or a hospital. He did not eat camel meat or any other camel products. He did not remember meeting any persons with respiratory symptoms [9-12].
Seven days after returning home, on May 11, he developed fever and myalgia. He visited a local clinic on May 12, 14, and 15. His symptoms, however, did not improve and a new non-productive cough developed on 15th May. He visited Pyeongtaek St. Mary’s (PTSM) Hospital (65 km south from Seoul), a secondary hospital in Gyeonggi Province. His chest X-ray showed a consolidation in the upper zone of right lung, and he was admitted to the hospital for pneumonia on May 15. Ceftriaxone and amikacin were started, but his pneumonia progressed despite the antibiotic treatment. He was transferred to the Samsung Medical Center (SMC), a university-affiliated tertiary hospital in Seoul on May 17 [9]. An infectious disease physician suspected MERS pneumonia and requested a laboratory test from the Korea Centers for Disease Control (CDC). MERS-CoV was confirmed on May 20.
The chain of transmission/hospital to hospital transmission
The chain of transmission was identified in all 186 MERS patients [13,14]. Of the 86 healthcare institutions that had taken in MERS-CoV-infected patients, nosocomial transmission occurred in 12 hospitals and four clinics (plus two ambulances) [13,15,16]. The epidemiological characteristics are summarized in Table 1 [17]. The epidemic curve is shown in Fig. 2.
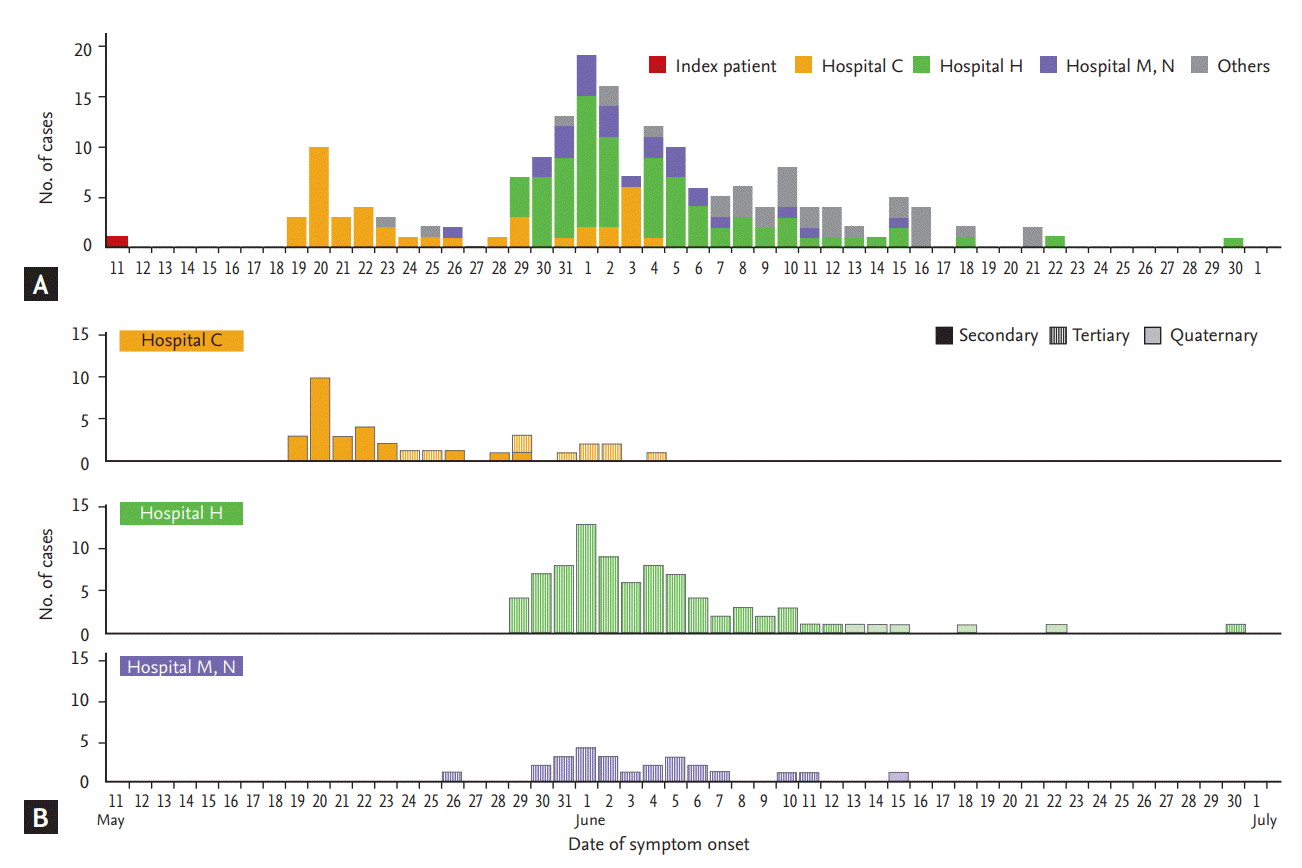
Epidemiological curve for the 2015 Middle East respiratory syndrome coronavirus (MERS-CoV) outbreak in the Republic of Korea. (A) Overall epidemiologic curve by date of symptom onset. Red color denotes the index patient. (B) Epidemic curves for each of the three main clusters. Outbreaks at Hospital C, Hospital H, and Hospital M and N are depicted in yellow, green, and purple color, respectively. Adapted from Korea Centers for Disease Control and Prevention [7].
The first wave of the epidemic: outbreak at PTSM Hospital
During his admission from May 15 to 17 at PTSM Hospital, the first patient was unknowingly spreading MERSCoV. Patients, visitors, and healthcare workers (HCWs) were exposed to MERS-CoV. Therefore, by May 20, when the Korea CDC noticed the importation of MERSCoV into the Republic of Korea, individuals staying on the same floor as the first case had already been exposed to MERS-CoV. As a result, a total of 36 MERS cases occurred at PTSM Hospital. Of them, 26 patients developed symptoms within 14 days after exposure, suggesting they were first-generation cases; the remaining 10 patients may be second-generation cases [7,10].
The mode of transmission of MERS-CoV at PTSM Hospital remains uncertain. In addition to family members of the first patient, only one patient shared the same room (#8104) with him; all the other cases stayed in other rooms, which were located > 2 m apart from room #8104. All patient rooms were equipped with an air ventilating system except for room #8104. A recent study using a multi-agent modeling framework suggested the transmission occurred via a long-range airborne route or via a combination of a long-range airborne route and direct contact transmission [18]. A chest computed tomography (CT) scan taken in the early stages (day 1 or 2) of illness showed very small, ground glass nodules in the periphery of the lungs, suggesting inhalation of airborne particles [19].
The index case for the outbreak at the SMC
The index case (superspreader-1) of the outbreak at the SMC was a 35-year-old man who had been exposed to MERS-CoV at PTSM Hospital during May 15 to 17 [19,20]. He developed a fever on May 21. Despite antibiotic treatment, his pneumonia became aggravated and tachypnea developed, so he eventually visited the emergency room (ER) at SMC on May 27. During his 58-hour stay at the ER, he experienced vigorous coughing and watery diarrhea. On May 29, the Korea CDC found he was staying there. A laboratory test confirmed MERS-CoV infection and he was transferred to the Seoul National University Hospital, a government-designated isolation facility on May 30.
The second wave of the epidemic: the outbreak at SMC
Many individuals had been exposed to the superspreader-1 at the ER, and contact tracing identified 675 patients, an estimated 683 visitors, and 218 HCWs as contacts of superspreader-1. Of them, 278 were quarantined and 617 were under active monitoring. As a result of exposure to superspreader-1, 82 had laboratory-confirmed MERSCoV infection, and an additional 10 were secondarily infected from them [20,21].
The outbreaks in Daejeon: Daechung & Geonyang Hospitals
The index case (superspreader-2) for the Daejeon (100 km south from Pyeontaek city) outbreak was infected at PTSM Hospital. He developed symptoms on May 20 and was admitted to Daechung Hospital on May 22. As his pneumonia progressed despite the treatments, he was transferred to Geonyang Hospital on May 28. A total of 25 secondary cases (14 in Daechung Hospital and 11 in Geonyang Hospital) were detected. Although superspreader-2 caused the two hospital outbreaks, the median time of incubation (8.8 days vs. 4.6 days), secondary attack rates (4.7% vs. 3.0%), and case fatality rate (28.6% vs. 63.6%) were different between the two outbreaks. The high fatality rate was associated with pre-existing pneumonia or poor underlying pulmonary function [22-24].
One patient traveled to China
A 44-year-old male, who had been exposed to the first index case on May 16, developed back pain on May 21. He is a son of the third MERS case. His sister had also been exposed to MERS-CoV and was confirmed to have an MERS-CoV infection on May 25. On May 26, against medical advice, he flew to Hong Kong and subsequently travelled to Huizhou through an entry point in Shenzhen City, Guangdong Province. The Korea CDC notified the WHO of his travel, and the Chinese health authority found him on May 27 and immediately isolated him. He was confirmed to have MERS-CoV infection on May 29. The Chinese authority identified 78 close contacts. After 14 days of quarantine, none of the contacts presented symptoms and all tested negative for MERS-CoV [25,26].
Epidemiological characteristics
Epidemiological characteristics have been reported by several groups (Table 2) [7,16,20,21,23,27-30]. The defining epidemiological characteristics were superspreading events at hospitals [30-32]. Early superspreading events generated a disproportionately large number of secondary infections, and the transmission potential decreased sharply in subsequent generations [30,33]. A total of 83% of transmission events were due to five superspreaders, and 44% of the 186 MERS cases were in-patients who had been exposed within the hospitals [7]. The spreaders transmitted MERS-CoV from days 1 to 11 of their illness (median, 7 days), and the number of patients infected by each spreader ranged from 1 to 84 (interquartile range, 1 to 12) [27].
The median incubation period and serial interval was 7 days and 12.5 days, respectively [7,34]. R0 ranged from 2.5 to 7.2, higher than the previous estimate of < 1 [35]. It was estimated at 4.04 for the outbreak cluster in PTSM Hospital, and 5.0 for the outbreak in SMC [36]. A mathematical modeling study demonstrated that although R0 < 1 overall, cluster sizes of over 150 cases are not unexpected for MERS-CoV infection [37].
Compared with the non-spreaders, the spreaders had a higher frequency of fever (≥ 38.5°C) and chest infiltrates in more than three lung zones, and longer non-isolated in-hospital days [27]. The spreaders had higher viral load in sputum samples with the cycle thresholds for the upE and ORF1a genes of 22.7 vs. 27.2 and 23.7 vs. 27.9, respectively. The spreaders with more than three transmissions had higher numbers of contacts and ER visits [38]. A brief exposure of a 10-minute stay and 2 minutes of talking was enough for the transmission of MERS-CoV [39].
VIROLOGY
Characterization of the MERS-CoV isolates
The whole genome sequences of MERS-CoV isolated from the Korea outbreak were reported [26,40-43]. The virus most similar to the Korean isolates was a camel virus (Camel/Riyadh/Ry159/2015) that belonged to lineage 5, a recombinant of lineage 3 and 4 [44,45]. Viruses from lineage 5 had been predominant in Saudi Arabian camels since November 2014, but human viruses of this lineage were reported from February 2015 [44]. A phylogenetic study of spike glycoprotein genes also showed the Korean strains were closely related to the viral strains from Riyadh, Saudi Arabia [46]. In a molecular study, 11 of 13 MERS-CoV genome had an I529T mutation and one D510G mutation in the receptor binding domain of viral spike protein, resulting in reduced affinity to the human cognate receptor, CD26 [47]. Heterogeneity analysis revealed the combined frequency of I529T and D510G was high (87.7%), although the frequency of both mutations varied greatly among specimens [48].
Another genome sequence study also reported deletions of 414 and 419 nucleotides between ORF5 and the E protein, suggesting that the virus might be defective in its ability to package MERS CoV [49]. A microevolution study found no evidence of changes in the evolutionary rate [43]. However, whether the transmissibility and virulence of the Korean isolates are different from those of the previous isolates from the Kingdom of Saudi Arabia remains to be determined by phenotypic assays.
Kinetics of virus shedding
A viral shedding study showed that the copies of MERSCoV RNA detected by real-time reverse transcription polymerase chain reaction (rRT-PCR) in respiratory samples peaked during week 2, and the median value was 7.21 log10 in the severe group and 5.54 log10 in mild cases [50]. The study also showed that viral titers were higher in throat samples than in nasopharyngeal samples. Another study also demonstrated higher viral loads were associated with severity and mortality [51].
Antibody response kinetics
After MERS-CoV infection, antibody responses developed by the third week of illness in most patients [52]. Seroconversion rates increased with the increase of disease severity. In a serologic study of 42 MERS patients, the seroconversion rate was 0% in asymptomatic infection, 60.0% in symptomatic infection without pneumonia, 93.8% in pneumonia without respiratory failure, and 100% in pneumonia with respiratory failure [53]. The serological response remained detectable for > 12 months in all survivors (11/11) who had severe disease. Antibody titers were not detectable in four of six patients who had mild pneumonia, suggesting that MERS-CoV seroepidemiological studies may underestimate the extent of mild and asymptomatic infection [54].
CLINICAL FEATURES
Clinical manifestations
The Korean Society of Infectious Diseases compiled the clinical data of the 186 MERS patients [55]. The median age was 55 years (range, 16 to 86). The male to female ratio was 3:2. The most common coexisting medical conditions were hypertension (31.7%), diabetes (18.8%), solid organ malignancy (13.4%), and chronic lung disease (10.2%). Patients with MERS-CoV infection developed a spectrum of illnesses, ranging from asymptomatic to fulminant pneumonia with fatal outcome. The respiratory symptoms were similar to other acute viral respiratory infections. At the time of presentation, fever had developed in 81.7%, cough in 56.7%, and sputum in 39.8% of patients. Symptoms of upper respiratory-tract infections were infrequent: sore throat was present in 9.1% and rhinorrhea in 1.6% of patients. Gastrointestinal symptoms were also observed: diarrhea was present in 19.4%, nausea or vomiting in 14.0%, and abdominal pain in 8.1% of patients. Diarrhea may be due to the side effect of lopinavir/ritonavir, as 87% of the patients received antiviral drugs for MERS-CoV treatment [55]. In the early stages of illness, cough and sputum were not prominent even in patients who later developed overt pneumonia [56]. At admission, 68% (123/180) of patients had abnormalities on chest radiographs, while 80.8% (147/182) of them developed the abnormalities during the course of the disease [55]. Sudden progression of pneumonia occurred around day 7 of illness [50,57]. Predictive factors for development of pneumonia included older age, high fever, thrombocytopenia, lymphopenia, C-reactive protein (CRP) ≥ 2 mg/dL, and a high viral load in sputum (threshold cycle value of rRT-PCR < 28.5) [58]. Forty-five patients (24.5%) were treated with mechanical ventilation and 15 patients (8.2%) needed extracorporeal membrane oxygenation [55]. The typical course of pneumonia is shown in Fig. 3.
Acute kidney injury (AKI) developed in 14.0% of the patients, 42.7% (44/103) had proteinuria, and 35.0% (36/103) had hematuria. Fifteen patients were treated with renal replacement therapy [55]. Old age is an independent risk factor for the occurrence of AKI [59]. Neuromuscular manifestations were not uncommon; hypersomnolence, weakness and tingling in the extremities were reported during the treatment of MERS, suggesting Guillain-Barré syndrome or virus-related sensory neuropathy [60].
Radiological findings
Serial changes in chest radiographs was reported in five patients [56]. Chest CT scans revealed rapidly developed multifocal nodular consolidations with ground-glass opacity halo and mixed consolidation, mainly in the dependent and peripheral areas [61].
Laboratory findings
There are few laboratory findings specific to MERS-CoV infection, although monocytosis with normal white blood cell count and low CRP level were more common in MERS patients at initial presentation [57,62].
Laboratory diagnosis of MERS-CoV
The guidelines for the molecular diagnosis of MERSCoV infection have been published by the Korean Society for Laboratory Medicine [63,64]. Specimen type and quality is important in the laboratory diagnosis of MERS-CoV infection. Lower respiratory-tract samples, such as sputum and tracheal aspirates, have higher viral loads than upper respiratory-tract samples [50]. However, MERS patients may not shed the virus during the early stage of their illness. Therefore, initial negative results should not rule out the possibility of MERS [65], and patients suspected of having MERS-CoV infection should be retested using a lower respiratory-tract sample [63,66]. When sputum cannot be obtained, throat swabs may be an alternative source of diagnostic samples [50]. Special attention should be given to diagnosing MERS-CoV infection in immunocompromised patients, as they may present with atypical features, such as a longer incubation period, a longer period from initial PCR positivity to symptom onset, and persistent viral shedding [67].
Antiviral treatment
An antiviral treatment guideline has been published by the writing committee with support from the Korean Society of Infectious Diseases and the Korean Society for Chemotherapy [68]. The guideline recommended a triple combination regimen of type 1 interferon, ribavirin, and lopinavir/ritonavir for 10 to 14 days. However, the guideline was mostly based on expert opinions and further study for the optimal antiviral treatment in MERS is warranted.
Risk factors for mortality and prognosis
The median duration of fever was 8 days. The median time to negative conversion of MERS-CoV in sputum samples by rRT-PCR was 17 days (range, 4 to 45) [55].
The median time from symptom onset to death was 14 days. The case fatality rate was 20.4% (38/186) (Fig. 4). The in-hospital mortality, 7-day mortality, and 28-day (from symptom onset) mortality were 19.4% (36/186), 3.8% (7/186), and 17.7% (33/186), respectively [55].
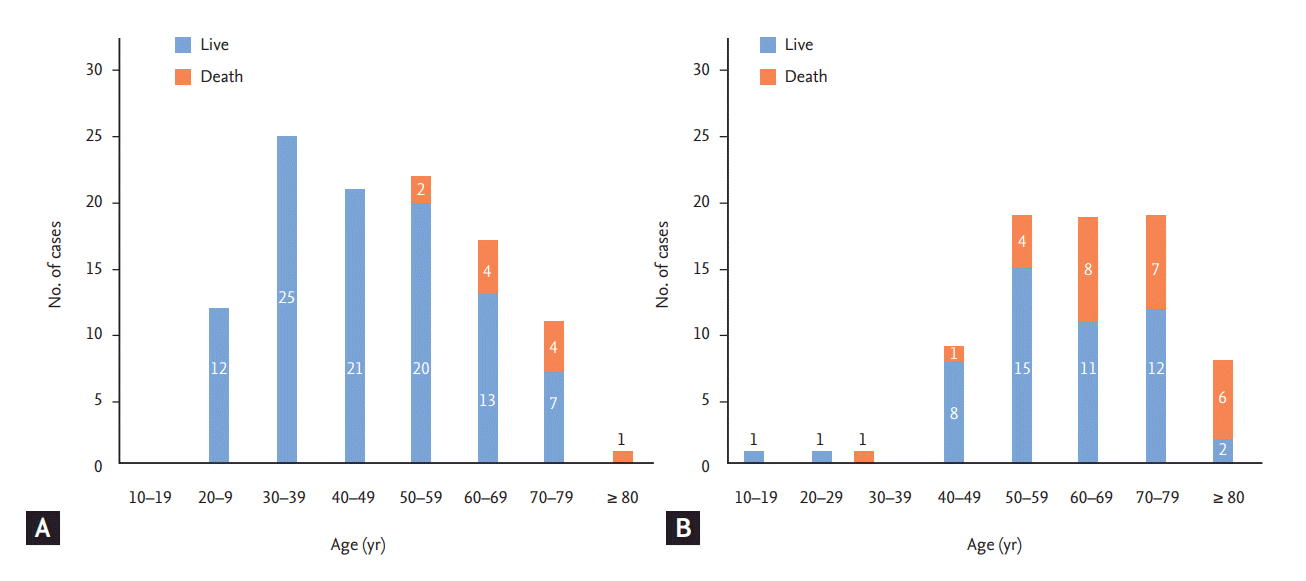
Case fatality ratio of Middle East respiratory syndrome during the 2015 Korea outbreak. Case fatality ratio was 10.1% (11/109) in patients without underlying diseases (A), and 35.1% (27/77) with underlying diseases (B). Overall case fatality ratio was 20.4% (38/186).
Host factors associated with mortality were old age (> 60 years), smoking history, pre-existing pneumonia, abnormal renal function, and comorbid conditions [24,69-71]. Low albumin, altered mentality, and high pneumonia severity index score at admission were risk factors for mortality [69]. MERS-CoV RNA in blood samples was detected in 33% (7/21) of patients at presentation, and it was associated with a worse clinical outcome [72]. A shorter incubation period was also associated with an increased risk of death [24,73].
A pregnant woman infected with MERS-CoV in her 35 weeks of gestational age developed dyspnea and her chest radiograph showed diffuse infiltrates in the left lower lung zone. She recovered from the infection and delivered a healthy full-term baby without vertical MERS-CoV transmission [74].
A patient developed organizing pneumonia 7 days after the resolution of MERS-CoV infection. He was successfully treated with corticosteroids [75].
In a mental health study, 7.6% of 1,656 patients who were quarantined showed symptoms of anxiety, and 6.4% reported feelings of anger during the 2 weeks of quarantine [76]. Mental health support, accurate information, and appropriate supplies, including food, clothes, and accommodation, should be provided to isolated persons [76]. A case of possible transfusion-related acute lung injury following transfusion of convalescent plasma was also reported [77].
INFECTION CONTROL AND PREVENTION
Guidelines for infection control and prevention
A comprehensive “MERS infection prevention and control guideline for healthcare facilities” was drafted by the guideline development committee with generous support from Korean Academic Societies [78]. The guideline included practical aspects of infection control and prevention based on the experience from the Korea outbreak, such as the composition of members for the MERS emergency committee, a space plan for an anteroom for donning and doffing, isolation of in-patients and HCWs in a hospital affected by an outbreak, and management of the deceased and autopsy [78].
The hemodialysis unit may become an epicenter for MERS-CoV outbreak because hemodialysis patients must receive renal replacement therapy even during the outbreak, and the risk of exposure to MERS-CoV continues. During the Korea outbreak, a hemodialysis unit was found to have a MERS patient, and a total of 104 patients and 18 HCWs were exposed to MERS-CoV. With support from the Korean Society of Nephrology, the dialysis unit could continue to operate while the exposed patients were isolated in the unit. Fortunately, no further transmission occurred at the unit [79]. After this successful experience, the Society published a clinical practice guideline for hemodialysis facilities dealing with MERS patients [80].
The Korea outbreak was driven by the superspreaders who visited multiple healthcare facilities; thus, generating a large number of secondary cases. Limiting unnecessary contacts with patients with respiratory symptoms in healthcare settings, especially in emergency departments, is of critical importance [33].
Environmental contamination
MERS-CoV could survive for longer than 48 hours at 20°C and 40% of relative humidity, suggesting contact or fomite transmission might occur in healthcare settings [81]. MERS-CoV was detected by rRT-PCR in specimens taken from the medical equipment [82-84]. MERSCoV was also isolated by cell culture of the air and swab samples taken from a MERS isolation unit, suggesting extensive contamination of the isolation unit [85,86]. Of the 186 cases, 23% were infected by undocumented contact between cases (i.e., indirect transmission of MERS-CoV via environmental contact) [87]. Therefore, fomites with possible MERS-CoV contamination should be sanitized, and a minimum room ventilation rate of six air changes per hour should be implemented to minimize recirculation of pathogen-bearing droplets. Meticulous environmental cleaning may be important for preventing transmission in healthcare settings.
Healthcare workers and MERS-CoV infection
There was a case of a 39-year-old female nurse who was infected with MERS-CoV during a cardiopulmonary resuscitation lasting 1 hour for a MERS patient who had pneumonia and hemoptysis [88]. Serological surveillance conducted after the MERS outbreak for asymptomatic infection among HCWs involved in the direct care of MERS patients showed that 0.3% (2/737) of them were MERS-CoV IgG positive by an indirect immunofluorescent assay. Among the HCWs who did not use appropriate personal protective equipment (PPE), seropositivity was 0.7% (2/294) compared with 0% (0/443) in HCWs with appropriate PPE use [89]. Another serological survey also showed that none of the 285 HCWs were positive for MERS-CoV immunoglobulin G, although 38.2% (109/285) of the HCWs reported experiencing MERS-like symptoms while caring for the MERS patients [90]. In a third study, 0 of 189 HCWs showed seroconversion by a plaque reduction neutralization test, although 20% to 25% of HCWs reported MERS-like symptoms [91].
During the outbreak in SMC, all HCWs assigned to MERS patients were screened for MERS-CoV, regardless of the presence or absence of symptoms. Of the 591 HCWs, three (0.5%) asymptomatic HCWs (two nurses and one physician) were found to be MERS-CoV (+), but they did not transmit the virus to others [21]. In another study, an asymptomatic nurse without PPE contacted 82 HCWs, including 33 close contacts who were exposed within 2 m from the index nurse and were not using PPE. None of the exposed HCWs were infected [92].
However, the potential for transmission from asymptomatic rRT-PCR positive individuals is still unknown. Therefore, asymptomatic HCWs who are rRT-PCR-positive for MERS-CoV should be isolated and should not return to work until two consecutive respiratory-tract samples test negative on rRT-PCR [93].
Control of the outbreak by private-public collaboration
The government requested the Korean Society of Infectious Diseases to participate in the control of the MERS outbreak. On June 8, 2015, the Society organized the Rapid Response Team, consisting of 15 infectious-disease doctors and two infection-control professionals [94]. Critical suggestions to prevent future epidemics were made regarding a rapid alerting system for index cases, provision of a sufficient airborne infection isolation facility, education and training of HCWs for important infectious diseases, and overcrowding and visitor control in the hospital [95].
CONCLUSIONS
The 2015 Korea outbreak was the largest outbreak outside of the Middle East. Researchers had a unique opportunity to compare the nature of MERS-CoV infection with the Middle East experience. The outbreak unveiled the weak points of infrastructure in our medical system, especially of preparedness for emerging global infectious diseases. Nosocomial transmission was one of the core features of MERS-CoV infection. The introspection for loose medical referral systems, overcrowding at the ER, a lack of expert resources and infection control infrastructure, and lack of organized preparedness for medical crises prompted the government to reform the healthcare system, and healthcare sectors to invest further in infectious diseases and infection control. Although the improvement is still ongoing, the speed and content are still currently insufficient. International cooperation to prepare for and defeat emerging infectious diseases should also be emphasized. Lessons we learned from the outbreak are summarized in Table 3.
Notes
No potential conflict of interest relevant to this article was reported.



