Fecal microbiota transplantation for marked colonic dilatation
Article information
A 59-year-old, chronically bedbound woman with cerebral palsy was admitted to a long-term care facility with fever and abdominal distension. Examination revealed marked abdominal distension without peritoneal signs, and imaging revealed severe diffuse colonic distension without mechanical obstruction (Fig. 1A). Conservative management included bowel rest, rectal and nasogastric decompression, and intravenous fluid and metoclopramide administration. Empiric metronidazole for suspected Clostridioides difficile was discontinued after a negative assay, whereas piperacillin-tazobactam was administered for urinary tract infection (days 3–10).
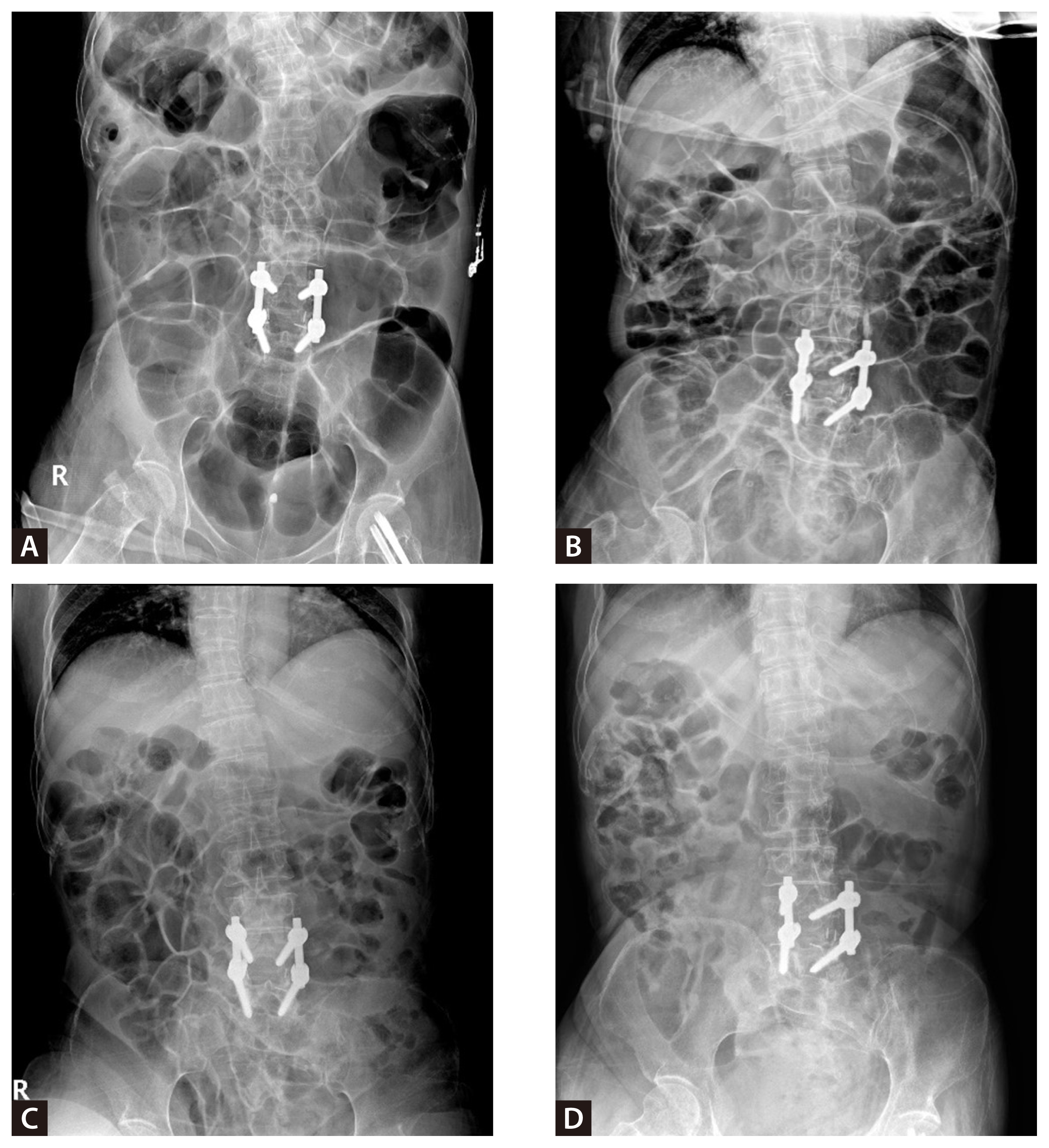
Abdominal radiographs demonstrate resolution of colonic pseudo-obstruction following fecal microbiota transplantation (FMT): (A) before FMT on the day of admission, (B) one day before FMT, (C) three days after FMT, and (D) seven days after FMT.
Despite five days of therapy, there was no clinical or radiographic improvement; tense distension and decreased bowel sounds persisted, with serial radiographs showing diffuse dilatation consistent with colonic pseudo-obstruction (Fig. 1B). After ≥72 hours of failed conservative therapy, fecal microbiota transplantation (FMT) was performed on day 6. Bowel preparation was not feasible because of severe colonic distention despite rectal enema attempts. To optimize luminal distribution, FMT was administered via colonoscopy (100 mL into the transverse colon) and duodenoscopy (150 mL into the duodenum) (Fig. 2).
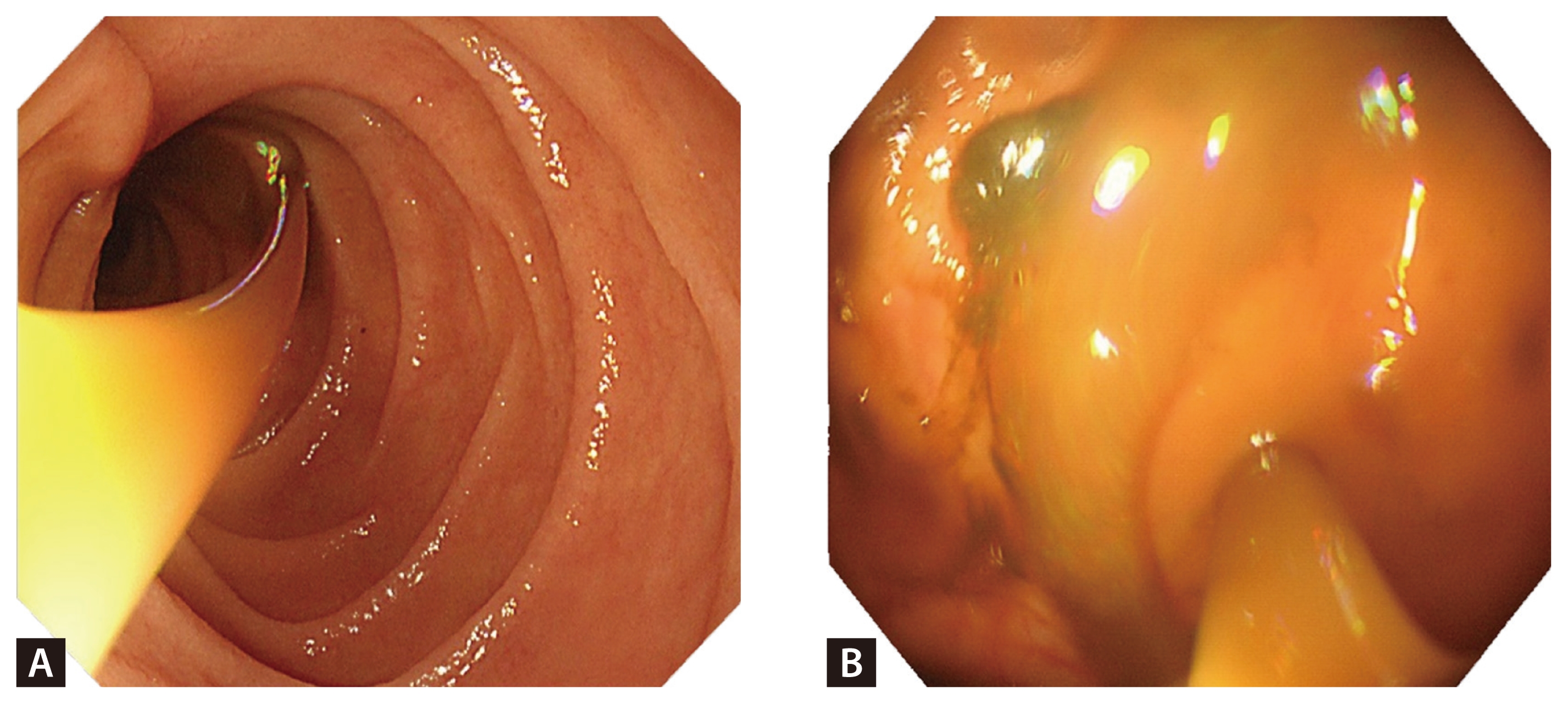
Fecal microbiota transplantation is delivered to the second duodenal portion (A) and transverse colon (B) to enhance delivery under suboptimal bowel preparation.
Clinical improvement was rapid. Bowel sounds recovered within 24 hours, allowing resumption of enteral nutrition. Normal defecation commenced within four days, allowing rectal tube removal. Follow-up radiographs demonstrated near-complete resolution of the colonic dilatation with minimal residual gas (Fig. 1D).
This case demonstrates FMT efficacy for refractory colonic pseudo-obstruction without C. difficile infection. Previous reports on acute and chronic intestinal pseudo-obstruction have suggested that FMT reduces intestinal bacterial overgrowth and improves motility [1,2] . A recent review framed colonic pseudo-obstruction as a dysbiosis-associated disorder that supports microbiome-targeted therapy [3] . Moreover, a randomized trial demonstrated that capsule FMT improved symptoms and microbial diversity compared to a placebo [4] . Overall, these findings support FMT as a promising therapeutic option if conservative measures fail to treat colonic pseudo-obstruction.
Notes
Acknowledgments
The authors are grateful to a patient whose case was used in this study.
CRedit authorship contributions
Eunseo Cho: conceptualization, investigation, data curation, writing - original draft, visualization; Jung-Hwan Lee: conceptualization, methodology, data curation, formal analysis, writing - original draft, writing - review & editing, project administration, funding acquisition; Ji-Taek Hong: resources, investigation; Kye Sook Kwon: resources, investigation; Yong Woon Shin: writing - review & editing
Conflicts of interest
The authors disclose no conflicts.
Funding
This study was supported by grants from 2024 Research Support Program of SD Medical Institute and Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: RS-2024-00410513).
