 |
 |
| Korean J Intern Med > Volume 20(4); 2005 > Article |
|
Abstract
Background
The aim of this study was to analyze the prevalence and clinical characteristic of the metabolic syndrome of adults, over 40 years old, living in Korea.
Methods
This study was carried out for 2 years, 2003-2004, on total 5,330 individuals (2,197 men and 3,133 women) selected by the stratified random cluster sampling among adults over 40 years old. Metabolic syndrome was defined based on both the NCEP-ATP III criteria and Modified ATP III criteria applying the WHO-APR (Asian Pacific Region)'s abdominal obesity criteria (waist circumference > 90 cm in men, 80 cm in women) instead of NCEP-ATP III criteria.
Results
Using NCEP-ATP III criteria, the age-adjusted overall prevalence of metabolic syndrome was 24.8% (17.6% in men, 30.0% in women). Age-adjusted overall prevalence of metabolic syndrome as defined by modified-ATP III criteria was 34.3% (26.3% in men, 40.1% in women). The prevalence of metabolic syndrome for each age group (40-49, 50-59, 60-69, Ōēź 70) in men was as follows: 18.8%, 17.4%, 18.3%, 14.5%. In women: 22.3%, 32.7%, 39.9%, 39.3%. The prevalence of hypertriglyceridemia (triglycerides Ōēź 1.7 mmol/l) was well correlated with the changing pattern of the prevalence of metabolic syndrome both in men and women.
Conclusions
The peak age of metabolic syndrome in men was age 40 through 49, and the prevalence decreased with aging. Therefore, early intervention for risk factors of metabolic syndrome might be required in men. On the other hand, prevention for cardiovascular disease will be needed for perimenopausal women due to considerably increased prevalence in the age 50 through 59.
Metabolic syndrome is designated as syndrome X by Reaven1) in 1988 as the risk factors for cardiovascular diseases like dyslipidemia, hypertension, and hyperglycemia were detected as clustering in same individual, and subsequently it was referred to as insulin resistance syndrome2) as these diseases have the common causality, insulin resistance. In 19983), WHO recommended the designation the metabolic syndrome as it has been reported that all factors in the insulin resistance syndrome could not be attributed to insulin resistance, and the NCEP ATP III manual published in 20014) introduced the metabolic syndrome as the second important goal for the reduction of the risk of cardiovascular diseases.
Recently, in the USA, calculated prevalence of the metabolic syndrome by summing all epidemiological data, 23.7% of the entire population of the USA and 43.5% over 60 years are reported to be metabolic syndrome5). Although the accurate data are not available, considering that the number of patients with metabolic syndrome was increased by 51% since 1991, the number of the metabolic syndrome patients may be increased by tens of millions in the last decades.
Several studies about the prevalence of the metabolic syndrome have been reported in Asian population including Korea6-8). However depending on the definition of the metabolic syndrome or study subjects, prevalence of the metabolic syndrome was somewhat different in each studies. And data from large scaled population based study was quite few. Thus, we performed this study to clarify the prevalence and clinical characteristic of the metabolic syndrome in middle aged Korean adults through large scaled population based study.
This study was performed from February to April in 2003 and 2004 on adults over 40 years living in the Chungju city area. One hundred sixty three districts were selected by the stratified random cluster sampling and the list of residents over 40 years living in the selected district was prepared and initially by the telephone visit of the investigators, the purpose of the study was explained and they were persuaded to participated in the study. One day prior to the examination, they were reminded of the preparation of the test. Of total 12,772 individuals, 5,330 persons (male: 2,197 persons, females: 3,133 persons) visited the health center and the participation rate was 41.7%. This study was approved by IRB at Kangnam St. Mary's hospital and informed consent was obtained from all participants.
All investigators were educated sufficiently in relation to the study prior to physical examination and the questionnaire. On the day of the investigation, the detailed data about medical history, family history, medication, life style, drinking habit, etc. of the subjects were obtained and physical examination was performed. Physical examination was performed by measuring height, weight, the waist and hip circumference according to the standardized method, and body mass index was calculated by weight (Kg)/height (m)2. Prior to measuring blood pressure, the subjects were asked to rest for 10 minutes and while seated, systolic blood pressure and diastolic blood pressure were measured. The blood pressure on the right upper arm was measured twice and if the difference of diastolic blood pressure were less than 5 mmHg, the average of two measurements was obtained. Prior to blood sampling, all subjects were fasted over 12 hours, and blood analysis was performed in a central laboratory (Samkwang Medical Laboratories, Seoul, Korea) for the accuracy and consistency. Total serum cholesterol and triglyceride were measured by an enzymatic calorimetric test, high density lipoprotein cholesterol was measured by selective inhibition method, and low density lipoprotein cholesterol was calculated by Friedewald formula. For the measurement of fasting plasma glucose, sodium fluoride tubes were used and measured by the hexokinase method. Serum insulin was measured by RIA kit (Dainabot, Japan). Insulin resistance was examined using the homeostasis (HOMA) and calculated by applying the following formula.
HOMA-IR= fasting insulin(┬ĄIU/mL) ├Ś fasting glucose(mmol/l)/22.5
Metabolic syndrome according to NCEP-ATP III criteria was defined if three or more of the following criteria were satisfied: 1) Abdominal obesity; Waist circumference (WC) in men > 102 cm and in women > 88 cm. 2) Hypertriglyceridemia; Ōēź 1.7 mmol/l. 3) Low HDL cholesterol; < 1.03 mmol/l in men and < 1.29 mmol/l in women. 4) High blood pressure; Ōēź 130/85 mmHg. 5) High fasting plasma glucose; Ōēź 6.1 mmol/l. We also applied WHO-APR (World Health Organization-Asian Pacific Region) criteria for abdominal obesity (WC in men > 90 cm and in women > 80 cm) instead of NCEP-ATP III criteria (so called, modified ATP III criteria).
SAS version 8.01 was applied. To compare the prevalence of metabolic syndrome among countries, ages were adjusted by Segi's standard world population9). The change of the pattern of the diagnostic factors of the metabolic syndrome according to the increase of age, 40-49 years, 50-59 years, 60-69 years and over 70 years was changed to a categorical parameter, and the distribution pattern of various factors was analyzed by Mantel-Haenszel Žć2 test. The groups were compared by t-test and ANOVA. The risk of the metabolic syndrome of HOMA-IR and the fasting insulin quartile groups was analyzed by logistic regression analysis and estimated by odds ratio. p<0.05 was considered as statistically significant.
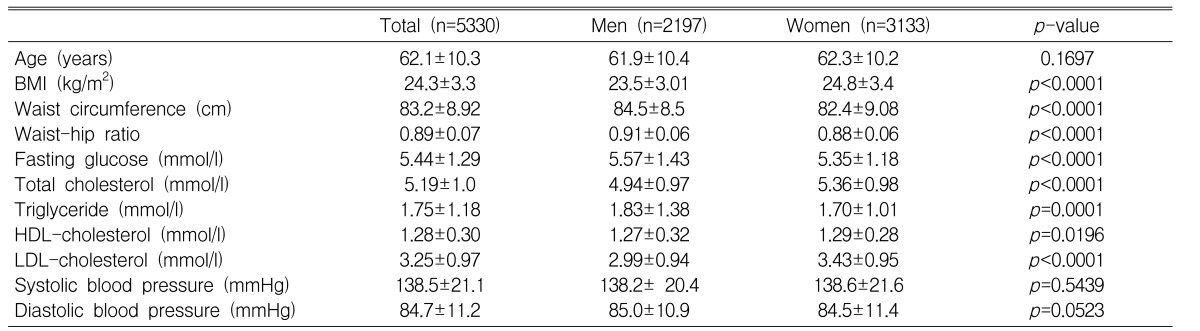
The mean age of the study population was 62.1┬▒10.3 years, and the age distribution of them in 40s, 50s, 60s and over 70 years was 26.2%, 21.9%, 30.7%, and 21.6%, respectively, which was similar to the age distribution of the population over 40 years in this area. In regard to body mass index, total cholesterol, HDL cholesterol, and LDL cholesterol, they were significantly higher in women than men (p<0.0001) (Table 1). The waist circumference, the waist-hip ratio, fasting blood glucose level, triglyceride, and diastolic blood pressure in men were significantly higher than women. The mean body mass index of the study subjects was 24.3┬▒3.3 kg/m2, which was overweight (BMI Ōēź23 kg/m2) according to the WHO-APR criteria, and in women, the average waist-hip ratio was 0.88┬▒0.06, which was within the abdominal obesity range (Waist-hip ratio Ōēź0.85).
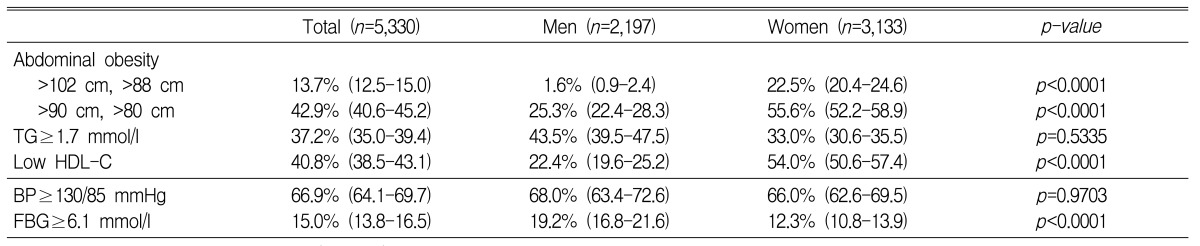
The age-adjusted prevalence of the metabolic syndrome according to the NCEP-ATP III criteria was 24.8% of the total study population, and the prevalence in men and in women was 17.6% and 30.0%, respectively (Table 2). On the other hand, the age-adjusted prevalence of the metabolic syndrome according to modified ATP III criteria was 34.3% of the total study population, and in men and in women was 26.3% and 40.1%, respectively.
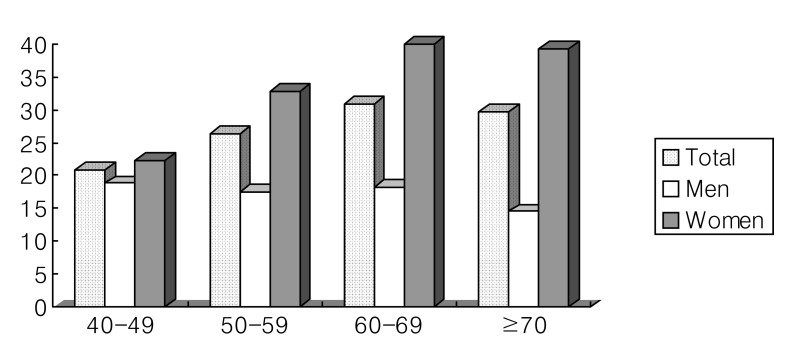
Examining the prevalence of the metabolic syndrome and their age distribution, in the total study population, 20.8% in 40-49 years, 26.4% in 50-59 years, 30.8% in 60-69 years, and 29.7% in over 70 years, which shows that the prevalence of the metabolic syndrome increases as age increases (Figure 1). Interestingly, in men, the prevalence was highest in their 40s and afterwards, it decreased as age increased (40-49 years; 18.8%, 50-59 years; 17.4%, 60-69 years; 18.3%, over 70 years; 14.5%). Using modified ATP III criteria, this changing pattern is more evident (40-49 years; 29.3%, 50-59 years; 25.7%, 60-69 years; 24.5%, over 70 years; 20.8%). In women, the prevalence of the metabolic syndrome increased abruptly in their postmenopausal period (50-59 years) and afterwards, the prevalence increased gradually as age increased (40-49 years; 22.3%, 50-59 years; 32.7%, 60-69 years; 39.9%, over 70 years; 39.3%). The prevalence of the metabolic syndrome defined as by modified ATP III criteria had similar pattern as that by NCEP ATP III criteria (40-49 years; 28.7%, 50-59 years; 40.1%, 60-69 years; 42.0%, over 70 years; 43.8%).
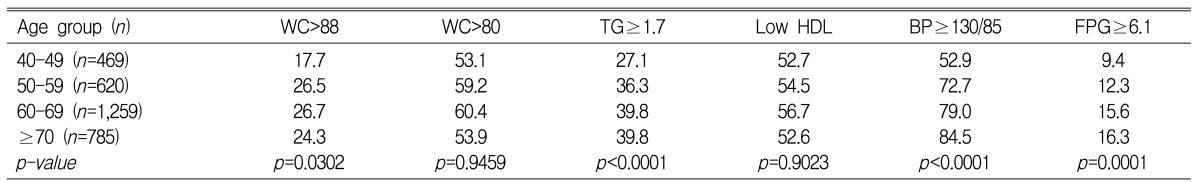
Assessing the prevalence of various factors relating with metabolic syndrome after the age adjustment, the prevalence of abdominal obesity and low HDL cholesterol in women was significantly higher than men (p<0.0001), but the prevalence of hypertriglyceridemia and high blood pressure in men and women was not significantly different (Table 3). When two different criteria, the NCEP-ATP III criteria and the WHO-APR criteria, were applied for abdominal obesity, the prevalence was 1.6% and 25.3% in men and 22.5% and 55.6% in women, respectively. So, there was a big difference between them, the prevalence of abdominal obesity by WHO-APR criteria was 16 times higher than by NCEP-ATP III criteria in men and 2 times higher in women. Applying the NCEP-ATP III criteria, the order of factors with high prevalence in men was high blood pressure, hypertriglyceridemia, low HDL cholesterol, high fasting plasma glucose, and abdominal obesity. In women, the order was high blood pressure, low HDL cholesterol, hypertryglyceridemia, abdominal obesity, and high fasting plasma glucose.
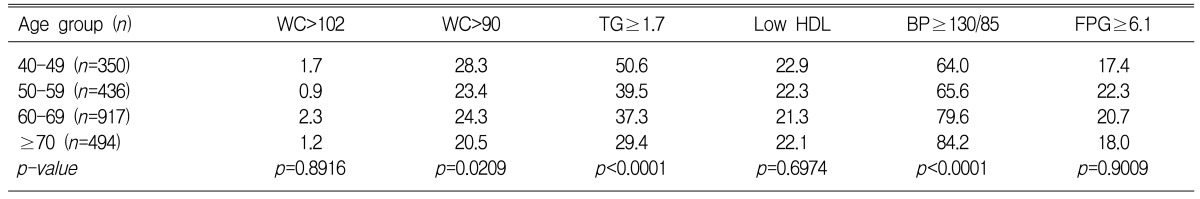
The changing pattern of the prevalence of each components of the metabolic syndrome according to the age distribution was examined. In men, high blood pressure (systolic and diastolic pressureŌēź130/85 mmHg) was increased with age while hypertriglyceridemia decreased with age (p<0.0001) (Table 4). When abdominal obesity was defined as by the NCEP-ATP III criteria, the significant difference in the changing pattern with age was not observed (p=0.8916). Applying the WHO-APR criteria (waist circumference > 90 cm), on the other hand, the prevalence was decreased with age (p=0.0209). In women, the prevalence of high blood pressure, high fasting plasma glucose and hypertriglyceridemia was increased as age increased (p<0.0001) (Table 5). In addition, applying NCEP-ATP III criteria for abdominal obesity, the prevalence increased as age increased (p=0.0302) and when we applied the WHO-APR criteria (waist circumference > 90 cm), the significant difference with age was not observed (p=0.9459).
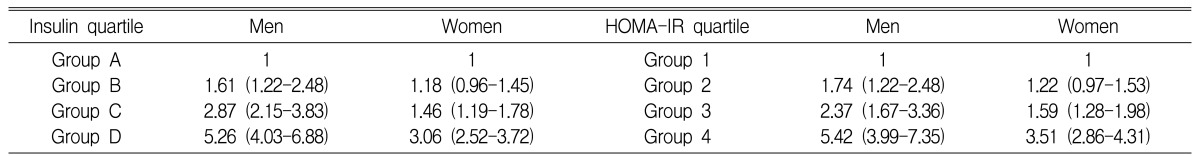
The association of insulin resistance and the relative risk of metabolic syndrome was analyzed by assessing the quartiles of fasting insulin and HOMA-IR (Table 6). As insulin resistance increased, the relative risk of metabolic syndrome determined as by the NCEP-ATP III criteria and the Modified ATP III criteria (data not shown) was increased.
In this study, we analyzed the prevalence of the metabolic syndrome and its clinical characteristics in the population over 40 years living in a rural area. In general, the prevalence of the metabolic syndrome varies widely and, especially, the difference within the same population is evident depending on the diagnostic criteria applied. The criteria currently used widely are the WHO criteria3), the EGIR criteria10), the NECP-ATP III criteria4), and the AACE criteria11). Among them, the WHO criteria and the NCEP-ATP III criteria are well known, and the latter is the most widely used term in practice as it is easy to apply. Abdominal obesity is considered as most important factor for metabolic syndrome defined as by NCEP-ATP III criteria. Recently, it has been frequently suggested that the application of the criteria for abdominal obesity, men > 102 cm and women > 88 cm, to Asians is not appropriate12-14). It has been well known that in Asians, even if their body mass index and waist circumference are equivalent as Caucasians, their visceral obesity is more severe compared with that of Caucasians15-17). In 2001, WHO-APR recommended the application of the different diagnostic criteria for abdominal obesity for Asian-Pacific region18). In our results, the prevalence of abdominal obesity diagnosed as by the NCEP-ATP III criteria in men was 1.6% and in women was 24.7%. Applied the WHO-APR criteria, it was 23.9% in men and 57.2% in women, so the prevalence of abdominal obesity in men was 17 times higher with WHO-APR criteria than NCEP-ATP III criteria. Thus, in defining abdominal obesity as the diagnostic criteria for metabolic syndrome, application of appropriate criteria suitable to Asian-Pacific region may be important to assess the prevalence of metabolic syndrome more accurately. We determined the cut-off value for abdominal obesity in this study subjects as 85 cm in males and 85 cm in females using ROC curve analysis (data not shown).
The most interesting finding in our study results was the trends of decrement in the prevalence of the metabolic syndrome in men as their age increased. Most reported studies on the prevalence of the metabolic syndrome5, 8), in both men and women, as their age increased, the prevalence of the metabolic syndrome increased. In addition, in women, the prevalence increased abruptly after menopause. The reason why prevalence of the metabolic syndrome increased due to aging is still not clear, but some factors like sex hormone deficiency19, 20), increment of risk factors for the metabolic syndrome might play a role in the development of insulin resistance of aged population. Our data showed that the changing pattern of prevalence of the metabolic syndrome is quite similar as previous reports in women, but not in men. And this changing pattern of men was consistent findings of two consecutive years in the survey of our study population. There can be some hypotheses to explain for this unique findings. First, this findings were due to early death of high risk population having more components of the metabolic syndrome in men. Thus, the more components of the metabolic syndrome they have, the earlier they die. Second, there were so many differences of their life styles between two generations (40-60 years and 60-70 years) that younger generation had more risk factors in the metabolic syndrome. This might be based on the thrifty genotype hypothesis21, 22). So it can be predicted that when the current 40-50s become 60-70s, the pattern of the prevalence of the metabolic syndrome become similar to the Westerners in two decades. In addition, if it were the case, this may allow to explain the reason why obesity as well as various diseases related to the metabolic syndrome has increased explosively in the past several decades in Korea as well as East Asians including China.
Furthermore, an additional important findings of our study was that a similar pattern is observable in the prevalence of hypertriglyceridemia. This may indicate the close association of hypertriglyceridemia to abdominal obesity or insulin resistance23, 24), and according to our recent studies25), triglyceride is highly correlate to body mass index in Koreans. In addition, considering that insulin resistance highly correlates to triglyceride26, 27), in Asians who have relatively high risk of insulin resistance in comparison with Westerners, triglyceride may be a candidate of a single factor that predicts the risk of metabolic syndrome.
In conclusion, this study was performed to examine the prevalence of the metabolic syndrome in middle-aged adults living in a rural area. In regard to the changing pattern of the prevalence according to age, in women, as they aged, the prevalence was increased, particularly it was increased abruptly in postmenopausal women. In men, the prevalence was highest in the 40-49 years, and afterwards, as they aged, triglyceride and the prevalence of abdominal obesity together with the prevalence of the metabolic syndrome decreased. Thus, in men, the aggressive prevention of various cardiovascular diseased before 30-40s might be necessary. In women, as the risk of abdominal obesity and metabolic syndrome increased after menopause, the precaution from late 40s may be necessary.
ACKNOWLEDGEMENTS
This study was supported by the grants from 2003-2004 Korea Health Promotion Research Program of the Ministry of Health and Welfare, Republic of Korea.
References
1. Reaven GM. Role of insulin resistance in human disease. Annu Rev Med 1993;44:121ŌĆō131PMID : 8476236.


2. DeFronzo RA, Ferrannini E. Insulin resistatnce: a multifaceted syndrome responsible for NIDDM, obesity, hypertension, dyslipidemia and atherosclerotic cardiovascular disease. Diabetes Care 1991;14:173ŌĆō194PMID : 2044434.


3. Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications: part 1. diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 1998;15:539ŌĆō553PMID : 9686693.


4. Expert Panel on Detection Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive summary of the third report of the National Cholesterol Education Program (NECP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA 2001;285:2486ŌĆō2497PMID : 11368702.

5. Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults: findings from the Third National Health and Nutrition Examination Survey. JAMA 2002;287:356ŌĆō359PMID : 11790215.


6. Cameron AJ, Chaw JE, Zimmet PZ. The metabolic syndrome: prevalence in worldwide populations. Endocrinol Metab Clin North Am 2004;33:351ŌĆō375PMID : 15158523.


7. Ramachandran A, Snehalatha C, Satyavani K, Sivasnakari S, Vijay V. Metabolic syndrome in urban Asian Indian adults: a population study using modified ATP III criteria. Diabetes Res Clin Pract 2003;60:199ŌĆō204PMID : 12757982.


8. Lee WY, Park JS, Noh SY, Rhee EJ, Kim SW, Zimmet PZ. Prevalence of the metabolic syndrome among 40,698 Korean metropolitan subjects. Diabetes Res Clin Pract 2004;65:143ŌĆō149PMID : 15223226.


9. King H, Rewers M. Global estimates for prevalence of diabetes mellitus and impaired glucose tolerance in adults. Diabetes Care 1993;16:157ŌĆō177PMID : 8123057.


10. Balkau B, Charles MA. Comment on the provisional report from the WHO consultation. Diabet Med 1999;16:442ŌĆō443PMID : 10342346.


11. Einhorn D, Reaven GM, Cobin RH, Ford E, Ganda OP, Handelsman Y, Hellman R, Jellinger PS, Kendall D, Krauss RM, Neufeld ND, Petak SM, Rodbard HW, Seibel JA, Smith DA, Wilson PW. American College of Endocrinology position statement on the insulin resistance syndrome. Endocr Pract 2003;9:237ŌĆō252PMID : 12924350.


12. Ramachandran A, Snehalatha C, Satyavani K, Sivasankari S, Vijay V. Metabolic syndrome in urban Asian Indian adults: a population study using modified ATP III criteria. Diabetes Res Clin Pract 2003;60:199ŌĆō204PMID : 12757982.


13. World Health Organization Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004;363:157ŌĆō163PMID : 14726171.


14. Tan CE, Chew SK, Ma S, Tai ES, Wai D. Can we apply the National Cholesterol Education Program Adult Treatment Panel definition of the metabolic syndrome to Asians? Diabetes Care 2004;27:1182ŌĆō1186PMID : 15111542.


15. McKeigue PM, Shah B, Marmot MG. Relation of central obesity and insulin resistance with high diabetes prevalence and cardiovascular risk in South Asians. Lancet 1991;337:382ŌĆō386PMID : 1671422.


16. Wang J, Thornton JC, Russell M, Burastero S, Heymsfield S, Pierson RN Jr. Asians have lower body mass index (BMI) but higher percentage body fat than do whites: comparisons of anthropometric measurements. Am J Clin Nutr 1994;60:23ŌĆō28PMID : 8017333.


17. Deurenberg P, Deurenberg-Yap M, Guricci S. Asians are different from Caucasians and from each other in their body mass index/body fat percent relationship. Obes Rev 2002;3:141ŌĆō146PMID : 12164465.


18. WHO/IASO/IOTF. The Asia-Pacific perspective: redefining obesity and its treatment. 2000;Health Communications Australia Pty Ltd.
19. Laaksonen DE, Niskanen L, Punnonen K, Nyyssonen K, Tuomainen TP, Valkonen VP, Salonen R, Salonen JT. Testosterone and sex hormone binding globulin predict the metabolic syndrome and diabetes in middle-aged men. Diabetes Care 2004;27:1036ŌĆō1041PMID : 15111517.


20. Carr MC. The emergence of the metabolic syndrome with menopause. J Clin Endocrinol Metab 2003;88:2404ŌĆō2411PMID : 12788835.


21. Joffe B, Zimmet P. The thrifty genotype in type 2 diabetes: an unfinished symphony moving to its finale? Endocrine 1998;9:139ŌĆō141PMID : 9867247.


22. Lev-Ran A. Human obesity: an evolutionary approach to understanding our bulging waistline. Diabetes Metab Res Rev 2001;17:347ŌĆō362PMID : 11747140.


23. Olefsky JM, Farquhar JW, Reaven GM. Reappraisal of the role of insulin in hypertriglyceridemia. Am J Med 1974;57:551ŌĆō560PMID : 4372881.


24. Garg A. Insulinn resistance in the pathogenesis of dyslipidemia. Diabetes Care 1996;19:387ŌĆō389PMID : 8729169.


25. Chang SA, Kim HS, Yoon KH, Ko SH, Kwon HS, Kim SR, Lee WC, Yoo SJ, Son HS, Cha BY, Lee KW, Son HY, Kang SK. Body mass index is the most important determining factor for the degree of insulin resistance in non-obese type 2 diabetic patients in Korea. Metabolism 2004;53:142ŌĆō146PMID : 14767863.


Figure┬Ā1
Prevalence of the metabolic syndrome according to NCEP-ATP III criteria in age distribution.
Table┬Ā2
Age-adjusted prevalence of the metabolic syndrome according to NCEP-ATP III & Modified ATP III criteria (Mod ATP III)




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



