 |
 |
| Korean J Intern Med > Volume 25(4); 2010 > Article |
|
Abstract
Thrombocytopenia is included in the classification criteria for systemic lupus erythematosus (SLE). However, severe thrombocytopenia causing spontaneous bleeding is rare. Here, we describe a 22-year-old woman who presented with spontaneous hemoperitoneum as the first manifestation of SLE. Laboratory findings compatible with SLE included positive antinuclear antibody and a false-positive venereal disease research laboratory. Symptoms suggesting the disease were not prominent early after admission, but headache and seizures that developed on the 3rd day of admission led to the diagnosis of SLE. The brain magnetic resonance imaging and angiography findings were compatible with the neuropsychiatric manifestations of SLE. High-dose steroid and monthly intravenous cyclophosphamide pulse therapy were effective at improving the headache and seizure, as well as the hemoperitoneum.
Systemic lupus erythematosus (SLE) is an autoimmune disease with diverse clinical manifestations [1]. Mild symptoms, such as arthritis and skin rash, predominate in frequency, but life-threatening manifestations requiring aggressive immunosuppressive therapy can also develop.
Thrombocytopenia may precede the other manifestations of SLE [2], but severe thrombocytopenia accompanying spontaneous bleeding is rare. As other diseases can cause thrombocytopenia, thrombocytopenia alone in the absence of other symptoms of SLE may cause the physician to delay in starting aggressive therapy.
Here, we report the case of a 22-year-old woman who suffered from spontaneous hemoperitoneum as the initial manifestation of SLE.
A 22-year-old woman suffering from vaginal bleeding was referred to our hospital from a local clinic. After admission in the gynecology department, she complained of diffuse abdominal pain, fatigue, and weakness. The vaginal bleeding had continued for more than 10 days after her last menstruation. The patient's body temperature, blood pressure, pulse rate, and respiratory rate were 36.9℃, 140/80 mm/Hg, 88/minute, and 22/minute, respectively. Her conjunctivae looked pale. Petechiae were found on the entire body, but there was no specific tender point on her abdomen.
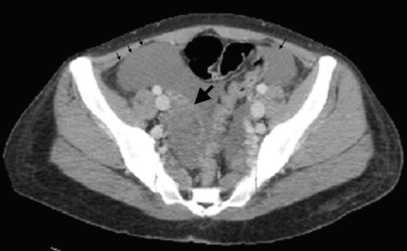
The complete blood count showed a white blood cell count of 8,960/µL (85.5% neutrophils, 11.9% lymphocytes, 1.5% monocytes), hemoglobin 6.7 g/dL, hematocrit 22.4%, and platelet count 7,000/µL. The values of coagulation tests were within normal limits. Since the pelvic ultrasound suggested a large amount of fluid, computed tomography (CT) of the abdomen and pelvis was performed, and demonstrated a large amount of blood with a 4.5 × 4 cm ill-defined mass-like lesion in the right adnexa suggesting a ruptured hemorrhagic corpus luteal cyst (Fig. 1). Given the severe thrombocytopenia, emergency surgery was delayed and a blood transfusion was started. Evaluating the possible causes of thrombocytopenia, the gynecologists consulted us for rheumatologic causes. We considered SLE and idiopathic thrombocytopenic purpura (ITP) as possible causes of thrombocytopenia.
Additional laboratory findings were as follows: increased antinuclear antibody titer (over 1:320, speckled pattern); false-positive venereal disease research laboratory (VDRL; FTA-ABS and TPHA tests were negative); decreased complement fractions (complement 3: 69 mg/dL [normal, 90 to 180], complement 4: 10 mg/dL [normal, 10 to 40]); positive platelet associated immunoglobulin G (IgG) antibody. The anti-dsDNA antibody, anti-Smith antibody, antibodies targeting extractable nuclear antigens, anticardiolipin antibody (IgG and IgM), and lupus anticoagulant were negative. Serologic tests for Epstein-Barr virus, cytomegalovirus, and human immunodeficiency virus (HIV) were all negative. A bone marrow biopsy revealed increased megakaryocytes, suggesting peripheral destruction or sequestration. Findings compatible with SLE were clear, but were insufficient to conclude that SLE was the cause of the thrombocytopenia; ITP seemed to be a more likely cause.
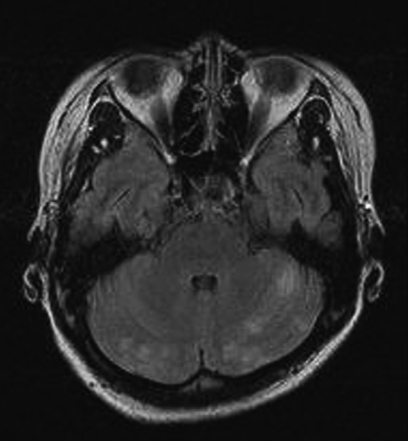
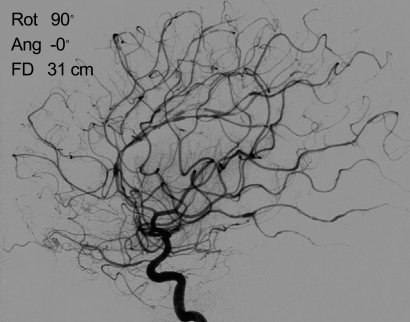
On the 3rd day of admission, she suffered from a severe headache and generalized seizure lasting for 1 minute. We performed brain magnetic resonance imaging (MRI), which showed multifocal cortical and subcortical hyperintensities in both cerebral and cerebellar hemispheres (Fig. 2). Angiography revealed multifocal stenosis and post-stenotic dilatation of the cerebral arteries compatible with vasculitis (Fig. 3). Those findings led us to conclude that the patient had SLE and she was transferred to our rheumatology department.
Since the patient's thrombocytopenia was severe, we administered intravenous (IV) immunoglobulin first, and then started intravenous steroid pulse therapy (1 g/day) for 3 consecutive days. After the therapy, we recommended monthly cyclophosphamide (CYC) pulse therapy (750 mg/m2) because of her life-threatening manifestat-ions: severe thrombocytopenia and cerebral vasculitis.
The petechiae disappeared and the platelet count increased to 229,000/µL after the therapy. The complement 3 and 4 levels were increased to 97 and 15 mg/dL, respectively. Pelvic ultrasound performed after the therapy showed only a scant amount of fluid.
As the improvements in her symptoms and laboratory findings were marked, we discharged the patient and recommended she take prednisolone at a dose of 1 mg/kg. After discharge, she underwent monthly CYC pulse therapy twice without severe adverse events.
Thrombocytopenia lower than 100,000/µL during the course of SLE is found in about 20% of cases [3], but severe thrombocytopenia causing spontaneous bleeding is rare. In this case, there was severe thrombocytopenia, but other symptoms suggesting SLE were not prominent initially. Although laboratory findings, including a false-positive VDRL and high antinuclear antibody titer, supported the diagnosis of SLE, they were insufficient to declare that the patient had SLE. Alternatively, the positive platelet-associated IgG antibody and bone marrow findings suggested the diagnosis of ITP. However, the development of a seizure and the MRI and angiographic findings confirmed the diagnosis of SLE.
Approximately 3 to 16% of patients with ITP not meeting the American College of Rheumatology criteria for SLE ultimately evolve into SLE [4], emphasizing the need for further monitoring of patients who seem to have ITP.
The neuropsychiatric syndromes of SLE (NPSLE) include 19 manifestations [5], including psychosis and seizures, as classification criteria [6]. Although severe neurological manifestations of SLE mandate immediate therapy, only one randomized controlled trial of the effectiveness of intravenous CYC for NPSLE has been conducted [7]. At present, even without evidence, CYC seems to be the most effective drug for severe, inflammatory neuropsychiatric lupus [7]. Based on studies of the effectiveness of CYC for severe thrombocytopenia and NPSLE [7,8], we treated the patient with IV CYC with high-dose steroid and she improved.
Many cases with a ruptured corpus luteum and hemoperitoneum are reported in the general population [9], but only one case of spontaneous ovarian rupture with hemoperitoneum has been reported in an SLE patient [10]. We experienced a patient with SLE, presenting with spontaneous hemoperitoneum due to severe thrombocytopenia as the first manifestation.
In conclusion, severe thrombocytopenia accompanying spontaneous bleeding can be the initial manifestation of SLE. An effort to discover symptoms, signs, and laboratory findings associated with the disease should be made so appropriate therapy is not delayed.
References
1. Hahn BH. In: Kasper DL, Fauci AS, Hauser SL, Longo DL, Jameson JL, eds. Systemic lupus erythematosus. Harrison's Principles of Internal Medicine. 2005;16th ed. New York: McGraw-Hill, 1960–1967.

2. Mestanza-Peralta M, Ariza-Ariza R, Cardiel MH, Alcocer-Varela J. Thrombocytopenic purpura as initial manifestation of systemic lupus erythematosus. J Rheumatol 1997;24:867–870PMID : 9150074.

3. Wallace DJ. In: Hochberg MC, Silman AJ, Weisman MH, Weinblatt ME, Smolen JS, eds. Severe lupus. Rheumatology. 2003;3rd ed. Edinburgh: Mosby, 1419–1425.
5. The American College of Rheumatology nomenclat-ure and case definitions for neuropsychiatric lupus syndromes. Arthritis Rheum 1999;42:599–608PMID : 10211873.
6. Hochberg MC. Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 1997;40:1725. PMID : 9324032.


7. Barile-Fabris L, Ariza-Andraca R, Olguin-Ortega L, et al. Controlled clinical trial of IV cyclophosphamide versus IV methylprednisolone in severe neurological manifestations in systemic lupus erythematosus. Ann Rheum Dis 2005;64:620–625PMID : 15769918.



8. Boumpas DT, Barez S, Klippel JH, Balow JE. Intermittent cyclophosphamide for the treatment of autoimmune thrombocytopenia in systemic lupus erythematosus. Ann Intern Med 1990;112:674–677PMID : 2334081.


-
METRICS

-
- 0 Crossref
- 0 Scopus
- 9,506 View
- 40 Download
- Related articles
-
A Case of Gastric Adenocarcinoma Presenting as Meningeal Carcinomatosis2007 December;22(4)
A Case of Pulmonary Vein Tumor Presenting as a Left Atrial Mass2007 March;22(1)
TNFB Gene Polymorphism in Patients with Systemic Lupus Erythematosus in Korean1995 July;10(2)
A Case of Hypothermia Combined with Systemic Lupus Erythematosus2001 March;16(1)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print


