 |
 |
| Korean J Intern Med > Volume 26(4); 2011 > Article |
|
Abstract
Background/Aims
The aim of this study was to identify changes in left ventricular (LV) performance in patients with a myocardial bridge (MB) in the left anterior descending coronary artery during resting and in an inotropic state.
Methods
Myocardial strain measurement by speckle-tracking echocardiography and conventional LV wall-motion scoring was performed in 18 patients with MB (mean age, 48.1 ± 1.7 years, eight female) during resting and intravenous dobutamine challenge (10 and 20 µg/kg/min).
Results
Conventional LV wall-motion scoring was normal in all patients during resting and in an inotropic state. Peak regional circumferential strain increased dose dependently upon dobutamine challenge. Longitudinal strains of the anterior and anteroseptal segments were, however, reduced at 20 µg/kg/min and showed a dyssynchronous pattern at 20 µg/kg/min. Although there were no significant differences in radial strain and displacement of all segments at rest compared with under 10 µg/kg/min challenge, radial strain and displacement of anterior segments at 20 µg/kg/min were significantly reduced compared with posterior segments at the papillary muscle level (44.8 ± 14.9% vs. 78.4 ± 20.1% and 5.3 ± 2.3 mm vs. 8.5 ± 1.8 mm, respectively; all p < 0.001), and showed plateau (40%) or biphasic (62%) patterns.
Myocardial bridge (MB), a congenital coronary anomaly [1,2], is a clinical condition with several clinical manifestations such as stable or variant angina, myocardial infarction, and sudden death [1-7]. The association of MB with anginal chest pain or abnormal results of noninvasive tests often constitutes an important clinical issue. Although phasic external vessel compression due to MB may induce significant reductions in diastolic coronary diameter [8] and endothelial dysfunction [9], controversy exists concerning the clinical and prognostic relevance of MB and the optimum therapy for symptomatic patients with this anomaly.
If noninvasive investigational tools could help clarify signs of ischemia in patients with MB, especially when the patient had angiographic findings of systolic compression of a coronary vessel only, adequate therapy might be possible. Standard stress echocardiography using visual assessment of wall motion to detect abnormalities is qualitative and subjective, and variability exists among observers and among institutions. Advanced echocardiographic techniques such as strain imaging, which is now widely used in resting echocardiograms, may also be applied to stress studies. This technique may provide a more quantitative and sensitive assessment of abnormalities in myocardial function and therefore reduce the difficulties inherent in stress echo interpretation.
We previously reported a quantitative assessment of myocardial function of symptomatic patients with MB using two-dimensional strain-based on speckle tracking [10]. In this study, we sought to investigate the effects of alterations in the inotropic stimulation induced by dobutamine challenge on myocardial function in patients with MB with speckle-tracking echocardiography strain-derived variables.
Low-dose dobutamine stress echocardiography (DSE) was performed in 18 patients (mean age, 48.1 ± 11.7 years; eight female) with exertional chest pain. Coronary angiography showed only MB of the mid segment of the left anterior coronary artery (LAD) without any significant atherosclerosis in either coronary artery. Quantitative coronary analysis software (Philips Medical System, Veenpluis, Netherlands) showed a more than 50% narrowing of the mid LAD by MB. Patients with hemodynamic and electrical instability and structural heart disease were excluded. None of the patients presented concomitant coronary stenosis or any present or previous cardiac events. All patients had normal conventional wall-motion scoring based on the standards of the American Society of Echocardiography, and echocardiography ruled out concomitant hypertrophic cardiomyopathy in all patients. Demographic data, including age, gender, and cardiovascular risk factors were recorded. The institutional review board of the Maryknoll Medical Center approved the study protocol. All study subjects gave informed consent before enrollment.
A biplane cardio-vascular system with charge-coupled device digital imaging for intervention and diagnosis (INTEGRIS BV 5000, Philips Medical System) was used to visualize the coronary artery. Quantitative measurements were analyzed by a workstation with dedicated software (WIN 32 ver. 3.3). For this purpose, the coronary segment of interest, including the total length of the myocardial bridge with the adjacent non-obstructed proximal and distal segments, was identified. Boundaries of this segment were then detected automatically and corrected manually if necessary. Absolute vessel diameters were determined using the guiding catheter as a reference. The percent diameter stenosis at the most severe site was automatically calculated from the computer estimation of the original dimension of the artery along the MB, defined as an interpolation between proximal and distal reference diameters. Angiographic lumen diameter evaluation was performed at end systole, when the diameter of the vessel was smallest, and during mid-diastolic frames. To determine interobserver variability for quantitative angiographic measurements of systolic and diastolic lumen diameter reductions, images from a random subset of 18 patients were analyzed by two independent observers (SMK and HGL) blinded to each other's results.
Conventional and strain echocardiographic examination were performed on all subjects lying in the left lateral supine position using the 2.5-MHz transducer on the Vivid 7 Dimension ultrasound equipment (General Electric, Horten, Norway). Images from parasternal short-axis views at three levels (mitral valve, papillary muscle, apex), and apical four-chamber, three-chamber (apical long axis), and two-chamber views of the left ventricle (LV) were obtained at end-expiratory apnea and were stored in cineloop format for subsequent offline analysis. Three heartbeats were collected from each view and analyzed off-line with an EchoPAC dimension system (General Electric). The LV was divided into six segments (anterior, inferior, lateral, posterior, septal, anteroseptal), each of which was then subdivided into three segments (basal, medial, apical).
LV images sampled at appropriate frame rates (60/sec) during DSE were post-processed using the speckle-tracking echocardiography software (Echopac 6.0.0, General Electric). Briefly, the displacement of speckles of LV myocardium (the acoustic markers) in each spot was tracked from frame to frame in each of the apical and short-axis views. The software package then automatically tracked the motion through the rest of the cardiac cycle, providing the LV strain (%) profile by default. Radial strain and displacement values were performed step by step by highlighting the key to the respective parameters built into the software. The same procedure was applied at rest, during DSE at 10 µg/kg/min and 20 µg/kg/min, and during the recovery stage. Left ventricular longitudinal data were collected from the bases of the septum, lateral, inferior, and anterior walls. Peak radial strains were obtained by tracking the parasternal short-axis images at the papillary muscle level during the above-mentioned three phases of DSE. The septal-to-posterior delay was measured as the time difference from the onset of the QRS complex and peak systolic radial strain wave between the mid-septal and posterior walls at the parasternal short-axis view by speckle-tracking strain imaging [11].
After conventional transthoracic echocardiography, patients received incremental doses of dobutamine (0, 10, 20 µg/kg/min), and speckle tracking echocardiography (STE)-enhanced DSE was performed. Each stage lasted 5 minutes, with acquisition of echo images during the last 1-2 minutes of each stage. Both systolic and diastolic indices were assessed during each dobutamine stage. All acquired LV images were digitally stored and post-processed on an Echopac BT 6.0.0 work station (General Electric). Frame rates were manually adjusted according to the heart rates during different stages of DSE.
All data are expressed as mean ± SD. Data were analyzed using SPSS version 11.0 (SPSS Inc., Chicago, IL, USA), and comparisons of all measurements were made using a paired Student's t test for continuous variables and chi-square test for categorical variables. A p value < 0.05 was considered to indicate statistical significance.
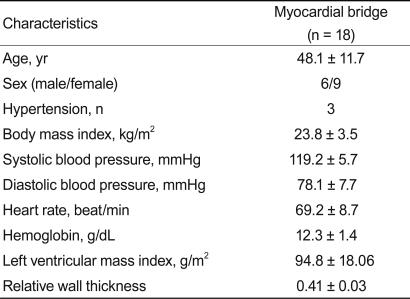
The mean age was 48.1 ± 11.7 years (range, 26 to 65). All patients reported a history of chest pain strongly suggestive of angina pectoris. The mean time interval between first symptoms and angiographic diagnosis of MB was 5.9 ± 6.7 months. Three patients had a history of mild hypertension without echocardiographic evidence of LV hypertrophy. Global LV function was normal in all patients with MB, and there were no signs of LV hypertrophy or hypertrophic cardiomyopathy. Patients' major demographic and clinical characteristics are shown in Table 1.
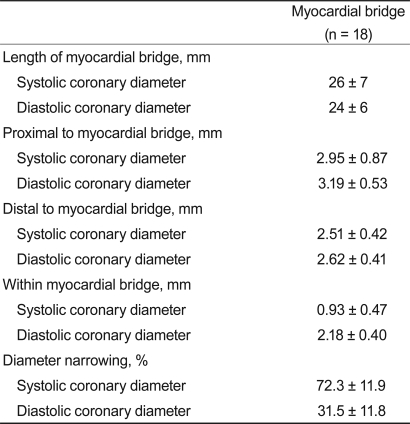
The complete coronary angiographic data are presented in Table 2. The mean percent diameter reduction at the most severe site of the MB during systole was 72.3 ± 11.9%, ranging from 54 to 95%. There was a persistent diastolic lumen diameter reduction of 31.5 ± 11.8%, with a minimum of 20% and a maximum of 57%. The mean absolute systolic diameter within the MB was 0.93 ± 0.47; three patients had a minimal diameter < 0.5 mm. The length of the MB during systole ranged from 19 to 44 mm (mean, 26 ± 7) and was not different from the diastolic values of 24 ± 6 mm (range, 21 to 42; p = not significant).
At rest, the heart rate (bpm) was 69.2 ± 8.7; this increased to 102.4 ± 5.7 after 20 µg dobutamine challenge. Conventional parameters of LV systolic function in all patients were normal at rest and during DSE (Table 3). Of the 18 patients, three had abnormal strain findings at rest, four at 10 µg/kg/min (Fig. 1), and nine at 20 µg/kg/min (Fig. 2). The other two showed a normal strain pattern during DSE (Fig. 3). Abnormal strain findings at rest or with 10 µg/kg/min either remained steady (2/7) or worsened (5/7) with increasing dobutamine dose, and all abnormal strain findings improved during recovery.
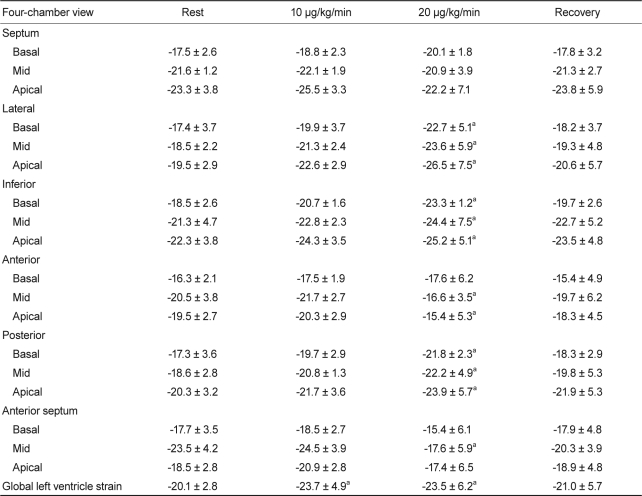
The mean comparative data in 18 patients with MB are presented in Table 4. Using the current software, peak systolic longitudinal strain values at rest were relatively uniform throughout the LV, highest in the inferior segments, and lowest in the anteroseptal segments, but the difference in the strain values between segments was not statistically significant. Peak regional longitudinal strain increased dose dependently on dobutamine challenge. However, that of the anterior and anteroseptal segments was reduced and showed a non-uniform pattern at 20 µg/kg/min. During the recovery period, there was no significant difference among the inter-segmental strain variables.
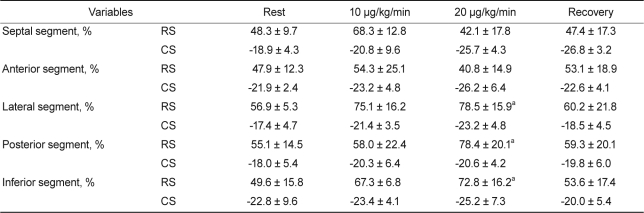
At rest, there were no significant differences in the peak regional circumferential strain (%); these increased dose dependently upon dobutamine challenge (Table 5). Although there were no significant differences in radial strain and displacement of all segments at rest, radial strain and displacement of anterior segments at 20 µg/kg/min were significantly reduced and significantly lower than posterior segments (43.6 ± 19.1% vs. 77.6 ± 17.5% and 5.3 ± 2.3 vs. 8.5 ± 1.8, respectively; all p < 0.001) (Fig. 4) and showed plateau (40%) or biphasic (62%) patterns. During the recovery period, there was no significant difference between the variables. Septal-to-posterior delay, a measurement of systolic dyssynchrony, was noticed simultaneously with abnormal strain pattern (45.6 ± 33.4 ms at 20 µg vs. 11.7 ± 20.3 ms at rest; p < 0.05), which increased with increasing dobutamine dose without remarkable QRS change on electrocardiography. Time from R wave on electrocardiography to transition from regional systole to early diastolic lengthening (Tr) was significantly delayed at 20 µg compared with at rest (446 ± 22.7 ms vs. 345 ± 25.9 ms; p < 0.05) (Fig. 5).
Inter- and intra-observer variability was analyzed by two independent observers (KIc and SMK) and by repeated measurement of these segments on another occasion by the same observer (KIc). Inter-observer variability was less than 20%, and intra-observer variability was 12%. The main reason for interobserver variability was a different location of the sample volume. Once sample volume was placed on a mutually agreed location within the myocardium, measurements became virtually identical.
MB occurs when a band of cardiac muscle overlies an intramural segment of a coronary artery, the intramural segment being referred to as a "tunneled" artery [1,2]. Until recently, visual interpretation of coronary angiograms revealed only the milking effect or systolic narrowing induced by significant MB. Normally, only 15% of coronary blood flow occurs during systole, and because MB is a systolic event on angiography, its clinical significance and relevance have been questioned. Quantitative coronary angiography and intravascular ultrasound (IVUS) clearly demonstrate that the phasic systolic vessel compression visualized on angiograms is coupled with a persistent diastolic diameter reduction. Intracoronary Doppler reveals increased flow velocities, retrograde systolic flow, and reduced coronary flow reserve [12,13]. The presence of tachycardia may unmask the ischemic effect of an MB by shortening the diastolic period and increasing the importance of systolic blood flow [14]. Also, tachycardia may worsen ischemia due to decreased diastolic filling time [6,15,16] and coronary fractional flow reserve (FFR), a measure of the ability to augment coronary blood flow under stress) [8,17-19]. So, symptomatic provocation of MB is induced by tachycardia without apparent wall-motion abnormality, which may differ from fixed LAD stenosis.
Assessing the functional significance of moderate coronary disease causes particular difficulties in day-to-day practice. Stress echocardiography is the cornerstone of diagnosis of coronary artery disease (CAD) by revealing the supply-demand mismatch of the LV during stress, classically at peak stress except in cases of viability assessment. Advanced echocardiographic techniques such as strain imaging, which is now widely used for evaluation of subclinical LV dysfunction [20-23], may also be applied to stress studies. Strain parameters have been correlated with FFR within the left coronary system [24], and in ischemic myocardium, strain decreases with stress [25]. Our data, collected using STE with dobutamine stress, suggest that patients with MB with ischemic insult have decreased regional longitudinal and radial strain (%) during low-dose DSE. Eighty-nine percent (16/18) of patients with MB in our study had symptoms compatible with ischemia during low-dose DSE. All patients had no chest pain at rest, which was different from our previous study, which investigated symptomatic MB patients with parameters of myocardial deformation at rest [10]. According to that study, radial strain and displacement by STE in LAD territories were reduced in symptomatic patients with MB. Myocardial strain is relatively independent of translational motion and other through-plane motion effects and should be relatively uniform throughout the normal LV myocardium. In contrast to normal hearts, the LV of MB was characterized by a marked non-uniformity of myocardial systolic strain. Reduced peak systolic longitudinal strain in LAD territories means reduced shortening or stretching. This was in contrast to the non-ischemic region, where near-normal shortening was observed. Global LV longitudinal strain showed the best correlation with conventional wall-motion analysis [26], although the overall correlation was rather modest. In the present study, our patients showed preserved and slightly increased circumferential strain (%) during low dose DSE, probably as a compensatory response. Due to the difficulty of speckle tracking at increasing heart rate, we focused on this important aspect and investigated LV motion at the moderately higher heart rates obtained with low-dose DSE to maintain the superior signal-to-noise ratio at frame rates appropriate for the currently available Echopac software. The importance of analyzing the intermediate stages of stress data, however, has not been substantiated. Recent data have shown that the acquisition and interpretation of intermediate stages of exercise in addition to peak exercise improves the detection of CAD and allows a better physiologic evaluation of the severity of coronary stenosis [27]. Our data on low-dose DSE support this concept.
Time to onset of regional relaxation has been proposed as a parameter of regional myocardial function and is defined as the time from the R wave of the electrocardiographic trace to the transition point from contraction to relaxation [28]. In healthy volunteers, it is shorter in the mid segments compared with apical segments (344 vs. 360 msec; p < 0.001). In this study, prolongation of time to onset of regional relaxation in patients with MB during DSE suggests MB-induced ischemia. Systolic dyssynchrony measured by septal-to-posterior delay was noticed simultaneously with abnormal strain pattern and increased with increasing dobutamine dose. Post-systolic compression, defined as myocardial compression occurring after the end of the LV ejection period, was suggested as an indicator of ischemia and also a marker for recovery of function after reperfusion. In this study, patients with MB during low-dose DSE showed sustained myocardial compression in LAD territories after the end of the LV ejection period; this was a plateau or biphasic phenomenon. We also have found a specific sign of peak strain (biphasic or plateau phenomenon), as described previously. Moreover, presence of the biphasic or plateau phenomenon was found at rest in 17% (3/18) of the patients. This may be because compression of the bridging segment was severe enough to induce the hemodynamic disorder that leads to formation of the biphasic phenomenon at rest. However, the presence of the echocardiographic biphasic or plateau phenomenon seemed not to be highly specific for the existence of MB, as it was also found in normal patients.
This study has some limitations. First, tracking of the region of interest is still suboptimal in some patients with hyperdynamic LV function and a poor echocardiographic image. It still takes from 5 to 10 minutes to achieve satisfactory tracking, and analysis is not performed in real-time. Patient selection was confined to those undergoing coronary angiography; thus the inferences from this study are limited to these patients. Finally, the lack of controls precludes provision of normal strain imaging data during STE-DSE.
In conclusion, low-dose dobutamine infusion provoked subtle changes in systolic and diastolic segmental function in patients with MB without notable LV functional impairment on conventional echocardiography. These changes were able to be detected by speckle-tracking techniques.
References
1. Angelini P, Trivellato M, Donis J, Leachman RD. Myocardial bridges: a review. Prog Cardiovasc Dis 1983;26:75–88PMID : 6346395.


2. Bourassa MG, Butnaru A, Lesperance J, Tardif JC. Symptomatic myocardial bridges: overview of ischemic mechanisms and current diagnostic and treatment strategies. J Am Coll Cardiol 2003;41:351–359PMID : 12575960.


3. Tauth J, Sullebarger T. Myocardial infarction associated with myocardial bridging: case history and review of the literature. Cathet Cardiovasc Diagn 1997;40:364–367PMID : 9096936.


4. Bauters C, Chmait A, Tricot O, Lamblin N, Van Belle E, Lablanche JM. Images in cardiovascular medicine: coronary thrombosis and myocardial bridging. Circulation 2002;105:130. PMID : 11772888.


5. Gowda RM, Khan IA, Ansari AW, Cohen RA. Acute ST segment elevation myocardial infarction from myocardial bridging of left anterior descending coronary artery. Int J Cardiol 2003;90:117–118PMID : 12821227.


6. Schwarz ER, Klues HG, vom Dahl J, Klein I, Krebs W, Hanrath P. Functional, angiographic and intracoronary Doppler flow characteristics in symptomatic patients with myocardial bridging: effect of short-term intravenous beta-blocker medication. J Am Coll Cardiol 1996;27:1637–1645PMID : 8636548.


7. Schwarz ER, Klues HG, vom Dahl J, Klein I, Krebs W, Hanrath P. Functional characteristics of myocardial bridging: a combined angiographic and intracoronary Doppler flow study. Eur Heart J 1997;18:434–442PMID : 9076380.


8. Klues HG, Schwarz ER, vom Dahl J, et al. Disturbed intracoronary hemodynamics in myocardial bridging: early normalization by intracoronary stent placement. Circulation 1997;96:2905–2913PMID : 9386156.


9. Kuhn FE, Reagan K, Mohler ER 3rd, Satler LF, Lu DY, Rackley CE. Evidence for endothelial dysfunction and enhanced vasoconstriction in myocardial bridges. Am Heart J 1991;122:1764–1766PMID : 1957772.


10. Cho KI, Park JH, Park JR, et al. Assessment of left ventricular function in symptomatic patients with myocardial bridge using two-dimensional strain. Korean Circ J 2006;36:617–625.

11. Tops LF, Suffoletto MS, Bleeker GB, et al. Speckle-tracking radial strain reveals left ventricular dyssynchrony in patients with permanent right ventricular pacing. J Am Coll Cardiol 2007;50:1180–1188PMID : 17868811.


12. Ge J, Erbel R, Rupprecht HJ, et al. Comparison of intravascular ultrasound and angiography in the assessment of myocardial bridging. Circulation 1994;89:1725–1732PMID : 8149538.


13. Ge J, Erbel R, Gorge G, Haude M, Meyer J. High wall shear stress proximal to myocardial bridging and atherosclerosis: intracoronary ultrasound and pressure measurements. Br Heart J 1995;73:462–465PMID : 7786662.



14. Rossi L, Dander B, Nidasio GP, et al. Myocardial bridges and ischemic heart disease. Eur Heart J 1980;1:239–245PMID : 7274234.


15. Pichard AD, Casanegra P, Marchant E, Rodriguez JA. Abnormal regional myocardial flow in myocardial bridging of the left anterior descending coronary artery. Am J Cardiol 1981;47:978–982PMID : 6782851.


16. Gallet B, Adams C, Saudemont JP, Fruchaud J, Hiltgen M. Myocardial bridge of the left anterior descending coronary artery and myocardial infarction: does coronary spasm play a part? Arch Mal Coeur Vaiss 1991;84:517–523PMID : 1676583.

17. Frazier OH, Macris MP, Myers TJ, et al. Improved survival after extended bridge to cardiac transplantation. Ann Thorac Surg 1994;57:1416–1422PMID : 8010782.


18. Ge J, Jeremias A, Rupp A, et al. New signs characteristic of myocardial bridging demonstrated by intracoronary ultrasound and Doppler. Eur Heart J 1999;20:1707–1716PMID : 10562478.


19. Escaned J, Cortes J, Flores A, et al. Importance of diastolic fractional flow reserve and dobutamine challenge in physiologic assessment of myocardial bridging. J Am Coll Cardiol 2003;42:226–233PMID : 12875756.


20. Kukulski T, Jamal F, D'Hooge J, Bijnens B, De Scheerder I, Sutherland GR. Acute changes in systolic and diastolic events during clinical coronary angioplasty: a comparison of regional velocity, strain rate, and strain measurement. J Am Soc Echocardiogr 2002;15:1–12PMID : 11781548.


21. Stoylen A, Heimdal A, Bjornstad K, et al. Strain rate imaging by ultrasonography in the diagnosis of coronary artery disease. J Am Soc Echocardiogr 2000;13:1053–1064PMID : 11119272.


22. Edvardsen T, Urheim S, Skulstad H, Steine K, Ihlen H, Smiseth OA. Quantification of left ventricular systolic function by tissue Doppler echocardiography: added value of measuring pre- and postejection velocities in ischemic myocardium. Circulation 2002;105:2071–2077PMID : 11980687.


23. Abraham TP, Nishimura RA, Holmes DR Jr, Belohlavek M, Seward JB. Strain rate imaging for assessment of regional myocardial function: results from a clinical model of septal ablation. Circulation 2002;105:1403–1406PMID : 11914244.


24. Dagdelen S, Yuce M, Emiroglu Y, et al. Correlation between the tissue Doppler, strain rate, strain imaging during the dobutamine infusion and coronary fractional flow reserve during catheterization: a comparative study. Int J Cardiol 2005;102:127–136PMID : 15939109.


25. Weidemann F, Jung P, Hoyer C, et al. Assessment of the contractile reserve in patients with intermediate coronary lesions: a strain rate imaging study validated by invasive myocardial fractional flow reserve. Eur Heart J 2007;28:1425–1432PMID : 17504804.


26. Reisner SA, Lysyansky P, Agmon Y, Mutlak D, Lessick J, Friedman Z. Global longitudinal strain: a novel index of left ventricular systolic function. J Am Soc Echocardiogr 2004;17:630–633PMID : 15163933.


Figure 1
Radial strain during dobutamine stress echocardiography at parasternal short-axis view showing a dyssynchronous strain pattern at 10 µg/kg/min.

Figure 2
Radial strain during dobutamine stress echocardiography at parasternal short-axis view showing a dyssynchronous strain pattern at 20 µg/kg/min.
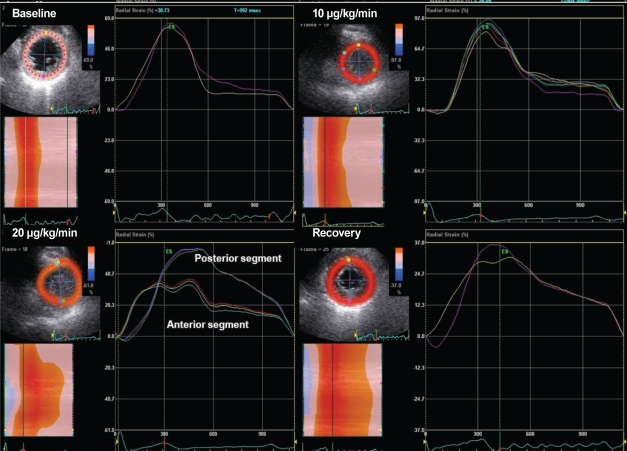
Figure 3
Radial strain during dobutamine stress echocardiography at parasternal short-axis view showing a normal strain pattern during dobutamine stress echocardiography.

Figure 4
Comparison of radial strain and displacement during dobutamine stress echocardiography. Radial strain and displacement of anterior segments at 20 µg/kg/min were significantly reduced and significantly lower than those of posterior segments. LV, left ventricle. ap < 0.001.
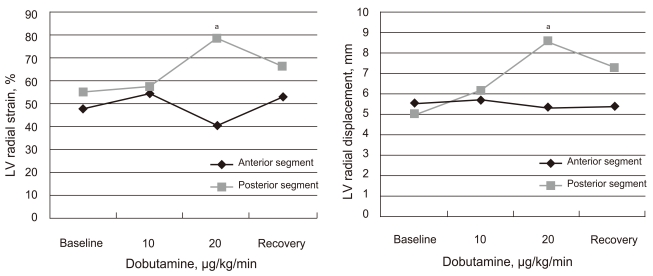
Figure 5
Comparison of time from R wave on electrocardiography to transition from regional systole to early diastolic lengthening (Tr). (A) Tr in controls, which was constant throughout the myocardium. (B) Tr of inferior segments of myocardial bridge (MB) (patients with mb ). (C) Tr of anterior segments of MB, which was significantly delayed in comparison with A and B.
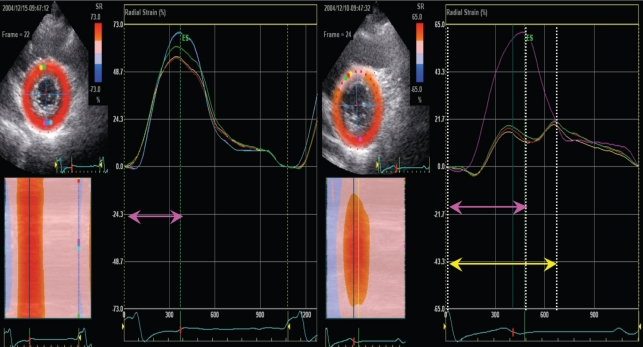
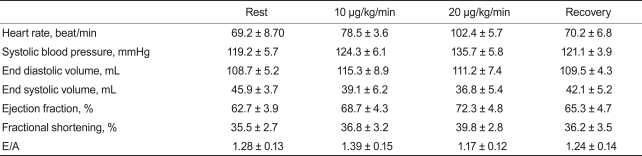
Table 3
Clinical and conventional echocardiographic parameters during dobutamine challenge and recovery state



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



