INTRODUCTION
Internal jugular vein stenosis is a rare condition that can manifest with facial edema. Most cases are related to the previous placement of catheters accompanied by thrombosis.
Pulmonary tuberculosis is very common in Korea. Despite treatment, chronic inflammation can continue, resulting in varying degrees of cicatrization and bronchovascular distortion. Up to 40% of patients with postpulmonary tuberculosis have a marked fibrotic response [1]. Although several cases of mediastinal tuberculosis presenting as superior vena cava syndrome have been reported [2-4], we describe jugular vein stenosis due to fibrotic traction in a tuberculosis-destroyed lung for the first time.
CASE REPORT
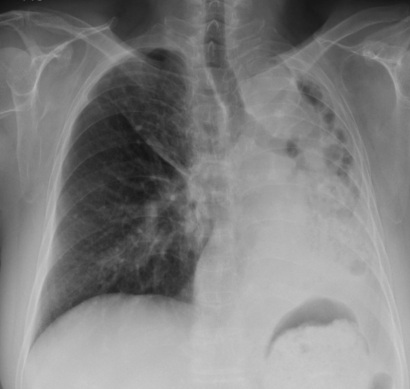
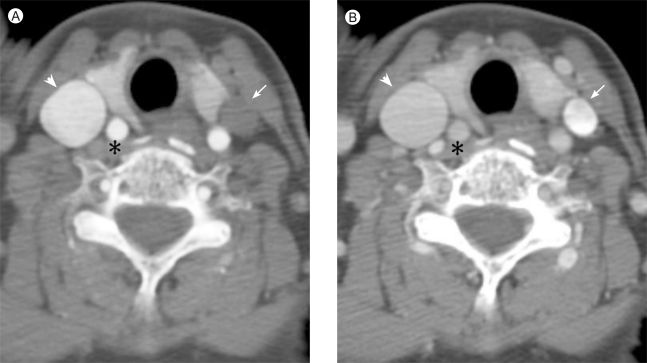
A 65-year-old woman presented with a 1-week history of left facial edema. She had a history of pulmonary tuberculosis 30 years earlier and bacterial pneumonia 1 year earlier. She was taking medication for hypertension, and had never smoked. The physical examination revealed left facial edema. The left arm was not edematous. Her blood pressure was measured at 130/70 mmHg. Routine laboratory tests revealed only mild leukocytosis (white blood cell count 10,570/mm3), with normal liver function, normal renal function, and normal coagulation tests. The chest X-ray revealed complete collapse of the left lung resulting in left-deviation of the mediastinal structures (Fig. 1). There was no active infiltration or lymph node enlargement. Computed tomographic venography showed delayed enhancement of the left internal jugular vein (Fig. 2). The right common femoral vein was punctured for venography. The collapsed left lung resulted in the innominate vein's being pulled leftward, leading to severe kinking and stenosis of the internal jugular vein at the level of insertion of the innominate vein (Fig. 3). Percutaneous transluminal angioplasty was performed. Even after serial balloon dilatation, a stenotic lesion was still observed and the pressure gradient was 9 mmHg; thus, stent insertion was indicated. The inserted stent was expanded fully, which decreased the pressure gradient to 3 mmHg and improved the facial edema.
DISCUSSION
Internal jugular vein stenosis can develop with various mechanical injuries. The most common cause is the previous placement of central venous catheters. Glisson traction [5], carotid endarterectomy [6], and shiatsu massage [7] can also result in internal jugular vein thrombosis. The presenting symptom is usually edema distal to the stenosis, which is dependent upon the site and chronicity of the lesion and the collateral system. Venography is mandatory for diagnosis and intervention. As restenosis after transluminal angioplasty of a central vein can reach 75% [8], stent placement is usually indicated. When endovascular treatment fails, surgical repair can be performed.
In this case, complete destruction of an entire lung caused a marked shift of the innominate vein to the left, resulting in stenosis of the internal jugular vein. Stent insertion after angioplasty successfully improved the edema.




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print





