 |
 |
| Korean J Intern Med > Volume 31(3); 2016 > Article |
|
Abstract
Background/Aims:
Sirolimus (SRL) is a promising immunosuppressant replacingcalcineurin inhibitors (CNIs). This study was performed to evaluate the safetyand immunologic benefits of conversion to SRL in stable kidney transplant (KT)recipients exposed to CNIs for long periods.
Methods:
Fourteen CNI-treated KT recipients with stable renal function for morethan 10 years were included. Either 2 or 3 mg per day of SRL was administeredwhile CNIs were reduced by half starting on day 1, and then stopped 2 weeks afterSRL introduction. The safety of SRL conversion was assessed considering thegraft function, acute rejection, and graft loss. Immunologic alterations were measuredvia serial changes of T cell and B cell subsets after SRL conversion. Adverseeffects of SRL conversion were also evaluated.
Results:
Conversion to SRL was successful in nine patients (64.2%). Conversionto SRL preserved graft function as compared to the baseline value (p = 0.115). Noacute rejection or allograft loss was observed during the follow-up period. Immunemonitoring of T and B cells revealed a regulatory T cells increase after SRL conversion (p = 0.028). Most adverse events developed within 6 weeks after SRLconversion, and oral mucositis was the main cause of SRL withdrawal.
Calcineurin inhibitors (CNIs) are indispensable immunosuppressive agents in kidney transplantation (KT). However, CNI-associated adverse events such as nephrotoxicity, increase of diabetes mellitus, and secondary malignancy limit the use of these drugs [1-3]. To overcome such limitations, CNI minimization with non-nephrotoxic immunosuppressant is recommended in clinical practice.
Sirolimus (SRL), a type of mammalian target of rapamycin inhibitor, was introduced in the late 1990s and regarded as a promising immunosuppressant for replacing CNIs in KT patients. Compared to CNI, SRL causes less nephrotoxicity and has anticancer effects [4]. In addition, SRL provides an immunologic advantage by increasing regulatory T cells (Treg) [5,6] and may prevent the development of chronic allograft nephropathy by suppressing the proliferation of smooth muscle cells and fibroblasts [7].
All these findings suggest that SRL may be beneficial for long-term CNI-exposed KT patients. However, most studies on CNI-to-SRL conversion have investigated the early post-transplant period [8-11], and there is little information on SRL conversion in patients with long follow-up periods. Therefore, we evaluated the safety and immunologic advantages of SRL conversion in long-term CNI-exposed KT recipients with stable graft function.
Inclusion criteria included patients who had been followed-up for more than 10 years after KT; no history of rejection; estimated glomerular filtration rate (GFR) more than 50 mL/min/1.73 m2 via modification of diet in renal disease (MDRD) with renal function change within 10% of baseline value in the past year; no immunosuppressive agent change during the past year; and proteinuria less than 0.3 protein (g)/creatinine (g) in spot urine. This study was approved by the Institutional Review Board (KC11OIS0917) of the Seoul St. MaryŌĆÖs Hospital, and all the patients provided written informed consent. All clinical investigations were conducted according to the principles expressed in the Declaration of Helsinki. The study is registered at www.ClinicalTrials.gov (Identifier: NCT01592253).
We started patients on 2 or 3 mg/day of SRL and reduced CNI dose to 50% of the baseline value at the same time. After 2 weeks, we stopped CNIs entirely and titrated the SRL dose to maintain the blood levels between 3 and 8 ng/mL. We discontinued other immunosuppressive agents such as enteric-coated mycophenolate sodium, azathioprine, or mizoribine till 3 months after conversion, but maintained low-dose steroids [12].
We evaluated the safety of SRL conversion using allograft function (estimated GFR via MDRD) at 2, 6, 12, and 24 weeks after conversion. Acute rejection was suspected if serum creatinine increased to more than 30% of the baseline value after SRL conversion. Rejection was confirmed via biopsy. Graft loss was defined as declining graft function that required dialysis, retransplantation, or death with functioning graft. We measured trough level of CNIs at baseline and 2 weeks after conversion. We checked SRL levels and performed laboratory tests including complete blood count, blood chemistry, urinalysis, and urine chemistry at 2, 6, 12, and 24 weeks after conversion.
We sampled peripheral blood before and 6 months after conversion to SRL. Peripheral blood mononuclear cells (PBMCs) were isolated, and cell cultures were performed as described previously [13]. Flow cytometric study of PBMCs was performed to analyze human intracellular cytokine production. The PBMCs were stimulated with phorbol myristate acetate and ionomycin in the presence of GolgiStop (BD Biosciences, San Diego, CA, USA) for 4 hours. For surface staining, cells were stained with combinations of the following monoclonal antibodies: CD4-PE/Cy7 (BioLegend, San Diego, CA, USA); CD45RAFITC (BD Pharmingen, San Diego, CA, USA); CD8-APC (Pharmingen), and CD25-APC (Pharmingen). Staining for chemokine receptor CCR7 was performed using monoclonal antibodies to it. Cells were washed, fixed, permeabilized, and stained to detect intracellular cytokines with monoclonal antibodies specific to interferon ╬│ (IFN-╬│, eBioscience); interleukin 4 (IL-4, eBioscience); IL-17 (FITC, eBio64DEC17, IgG1, ╬║; eBioscience); Foxp3 (FITC, PCH101, IgG2a, ╬║; eBioscience); IFN-╬│ (PE, B27, IgG1, ╬║; Pharmingen), and IL-10-APC (JES3-19F1, IgG2a, ╬║; Pharmingen). Appropriate isotype controls were used for gate setting for measuring cytokine expression. Cells were analyzed on a FACS Calibur flow cytometry system (BD Biosciences).
During each outpatient clinic visit, we examined adverse events that developed after SRL conversion. These included mucositis, folliculitis, dermatitis, or any signs of infection. We monitored the following: development of proteinuria as spot urine protein-to-creatinine ratio (PCR), diabetes mellitus via fasting glucose level, dyslipidemia via fasting lipid level or lipid lowering agents, leukopenia, anemia, thrombocytopenia, increasing aspartate or alanine aminotransferase, and requirement of antihypertensive medication. We defined the patientŌĆÖs situation as tolerable when the patient had successfully received SRL for 6 months without any serious adverse events.
Statistical analysis was performed using SPSS version 18.0 (SPSS Inc., Chicago, IL, USA). The comparison of numerical variables at baseline, 2, 6, 12, and 24 weeks from conversion was performed using the Friedman test. The comparison of numerical variables before and 24 weeks after conversion was performed using the Wilcoxon signed-rank test. The results are presented as mean ┬▒ standard deviation or standard error, counts and percentages, or median with ranges depending on the data type. The p values < 0.05 were considered significant.
A total of 45 KT patients met the inclusion criteria in Seoul St. MaryŌĆÖs hospital. Among them, 14 patients (31%) agreed to participate in this study, and they were ultimately enrolled. The mean duration from KT to initiation of the study was 14.7 ┬▒ 2.9 years (median, 13.5; range, 12 to 19.5). The mean MDRD-GFR was 72.2 ┬▒ 20.2 mL/min/1.73 m2. Only one patient was highly sensitized (her flow cytometric crossmatch was positive for B cells), so she had taken plasmapheresis three times before KT. Other baseline patient characteristics are presented in Table 1. Of the 14 patients, eight (57%) were receiving cyclosporine (CsA) with a median dosage of 150 mg (range, 75 to 175); the mean blood trough level was 95.8 ┬▒ 58.4 ng/mL. The remaining patients (n = 6, 43%) were receiving tacrolimus (TAC) with a median dosage of 2 mg (range, 2 to 4); the mean blood trough level was 4.2 ┬▒ 2.1 ng/mL. The patientsŌĆÖ immunosuppressive regimens are also shown in Table 1.
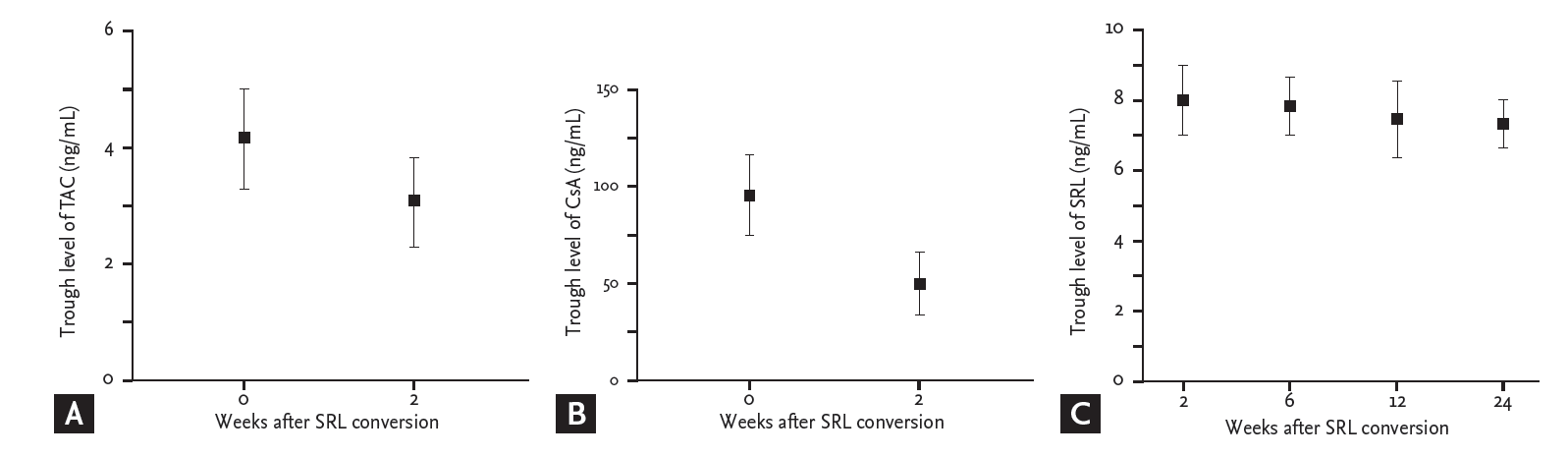
The 6-month conversion success rate was 64.2% (n = 9), while 35.8% of patients (n = 5) ceased receiving SRL. Renal allograft function at baseline and 2, 6, 12, and 24 weeks after SRL conversion was not significantly different (71.2 ┬▒ 17.6, 71.0 ┬▒ 17.1, 72.0 ┬▒ 16.7, 71.2 ┬▒ 17.6, and 67.7 ┬▒ 14.6 mL/min/1.73 m2 via MDRD-GFR respectively), indicating good graft function preservation after SRL conversion (p = 0.115) (Fig. 1). There was no acute rejection or graft loss after SRL conversion. Fig. 2 shows trough levels of TAC and CsA before and 2 weeks after SRL conversion and SRL trough levels at 2, 6, 12, and 24 weeks after SRL conversion. The 50% dosage reduction of CsA or TAC caused the trough level to decrease by 48.7% and 27.2%, respectively (Fig. 2A and 2B). Levels of SRL were variable in the early period of conversion but gradually stabilized and reached the target level (3 to 8 ng/mL) by 12 weeks post-conversion (mean trough level, 7.4 ng/mL). The levels were not different statistically (p = 0.919), but showed decreasing pattern throughout the study periods (Fig. 2C).
Figs. 3 and 4 show the immunologic changes in six of the nine successfully converted patients. Three of them had received CsA, while the remaining three had received TAC before SRL conversion.
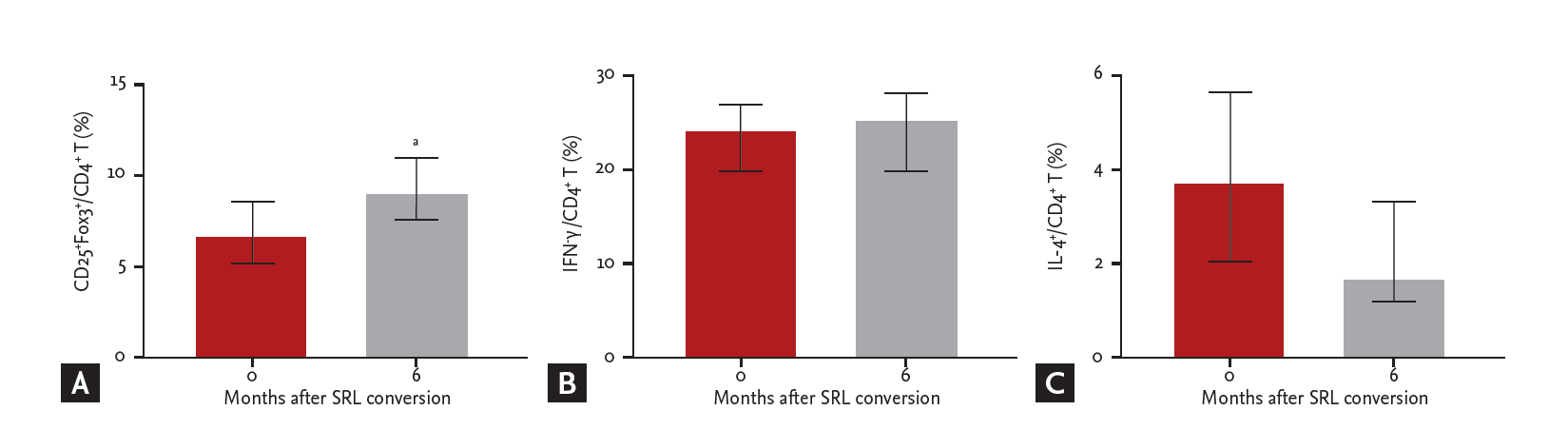
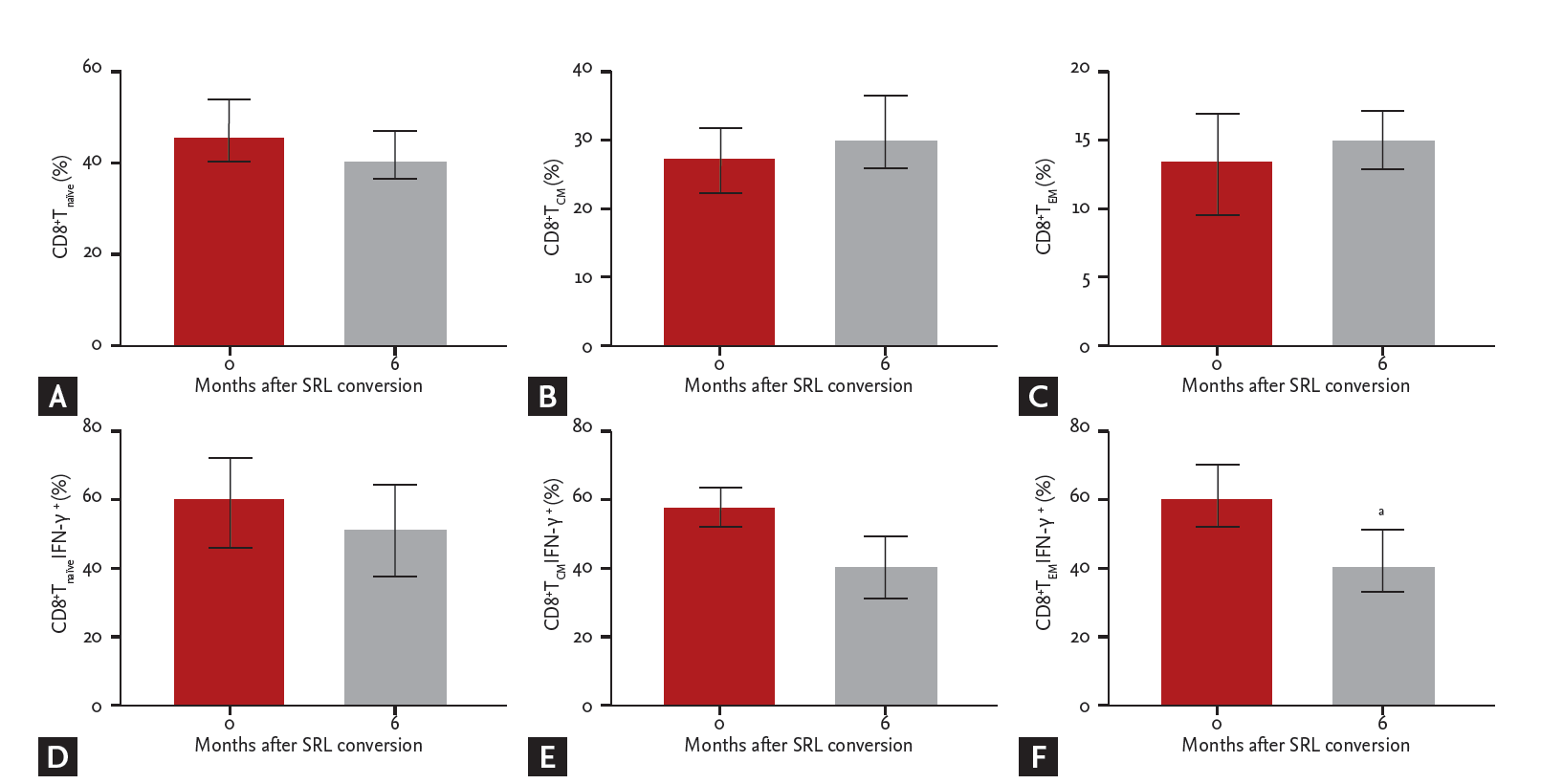
The percentage of CD4+ Treg increased at 24 weeks after SRL conversion (6.3% ± 3.2% vs. 8.6% ± 5.4%, p = 0.028) (Fig. 3A). There were no differences in the percentages of Th1 (23.4% ± 9.8% vs. 24.1% ± 10.4%, p = 0.917), Th2 (3.5% ± 4.2% vs. 1.3% ± 1.2%, p = 0.6), or Th17 (1.3% ± 0.6% vs. 2.1% ± 1.1%, p = 0.249) (Fig. 3B-3D). The percentage of CD8+ Tnaïve (44.0% ± 13.8% vs. 39.8% ± 9.0%, p = 0.462), CD8+ central memory T cells (TCM) (27.1% ± 10.5% vs. 30.6% ± 12.7%, p = 0.753) or CD8+ effector memory T cells (TEM) (13.0% ± 9.3% vs. 15.3% ± 4.2%, p = 0.6) also did not alter after SRL conversion (Fig. 4A-4C). The percentage of IFN-γ producing CD8+ Tnaïve (59.7% ± 26.1% vs. 50.2% ± 41.8%, p = 0.6) and TCM (57.4% ± 15.1% vs. 38.1% ± 24.7%, p = 0.075) did not change (Fig. 4D and 4E), but the percentage of IFN-γ producing CD8+ TEM reduced after conversion (58.5% ± 18.9% vs. 37.9% ± 25.4%, p = 0.046) (Fig. 4F). No significant difference was seen between B cell subsets. The percentage of memory B cells (22.6% ± 11.5% vs. 30.9% ± 11.1%, p = 0.345), mature B cells (39.1% ± 9.8% vs. 35.1% ± 11.3%, p = 0.293), and immature B cells (5.1% ± 3.6% vs. 9.7% ± 9.3%, p = 0.345) did not change 24 weeks after SRL conversion.
Total cholesterol, low-density lipoprotein, and triglyceride levels increased after SRL conversion (178 ┬▒ 22 mg/dL vs. 223 ┬▒ 58 mg/dL, p < 0.001; 97 ┬▒ 28 mg/dL vs. 149 ┬▒ 45 mg/dL, p < 0.001; and 94 ┬▒ 38 mg/dL vs. 114 ┬▒ 57 mg/dL, p = 0.018; respectively). Urine PCR also increased after conversion (0.08 ┬▒ 0.08 vs. 0.39 ┬▒ 0.40, p = 0.026). Of the 14 patients, 11 (79.6%) experienced mucocutaneous adverse events. Oral mucositis (n = 7), dermatitis (n = 4), facial and leg edema (n = 3), folliculitis (n = 1), acne (n = 1), and diarrhea (n = 1) were all recorded. Most events occurred within 6 weeks after conversion and led to withdrawal. The main cause of discontinuation was intolerable oral mucositis (n = 3). Other causes were facial dermatitis (n = 1) and diarrhea (n = 1). Development of leukopenia, anemia, thrombocytopenia, abnormality of liver function tests, increase of fasting glucose, or infections was not observed.
The results of our study clearly demonstrated that SRL conversion is safe in long-term (mean, 14.7 years) CNI-exposed KT recipients with stable graft function. Conversion to SRL did not affect graft function, and there were no episodes of acute rejection or graft loss. Furthermore, conversion to SRL provided immunologic benefits by increasing Treg. These findings suggest that conversion to SRL is recommendable in long-term CNI-exposed KT patients with stable graft function.
First, we evaluated whether conversion to SRL is actually safe in long-term CNI-exposed KT patients. Although graft function was stable and no acute rejection episodes were noted after SRL conversion, we did not observe further improvement of graft function after SRL, as observed in other studies of early SRL conversion [14,15]. This may be related to the minimal dose of CNIs received by patients in our study, which infers minimal toxicity before SRL conversion. The lack of acute rejection episodes in this study seems to be related to the conversion timing. Our patients were also immunologically stable before conversion; therefore, conversion to SRL may not have affected the overall immune status. Taken together, our study suggests that SRL conversion is safe without leading to deteriorating graft function, development of acute rejection, or graft loss.
Treatment with CNIs induces the production of proinflammatory cells, such as Th17, and reduces that of anti-inflammatory phenotypes, such as Treg, by blocking the transcription of the gene encoding IL-2 [16,17]. We reported previously that SRL treatment decreased Th17 and increased Treg in vitro and in vivo [18]. Therefore, we expected that SRL conversion would provide immunologic advantages by reciprocal regulation of the Th17/Treg axis. In our study, SRL conversion increased the proportion of Treg but did not change the proportion of Th17. Additionally, IFN-╬│ producing CD8+ TEM decreased, which was associated with late allograft dysfunction in our previous study [19]. Based on these immunologic findings, SRL may have higher favorable effects by regulating the Th17/Treg axis and by decreasing IFN-╬│ producing CD8+ TEM in KT recipients when compared to current CNI therapy. In B cell subpopulations, however, SRL conversion did not induce any change. This may be because of our patientsŌĆÖ stable immune status before conversion.
The SRL conversion was successful in nine of 14 patients (64.2%). However, the five patients (35.8%) who withdrew did so primarily owing to mucocutaneous inflammation, mostly within 6 weeks after conversion. The conversion rate and adverse events were similar to previous studies [9,10,15,20], but serious adverse events such as pneumonitis did not occur in our study. The leading cause of SRL discontinuation was oral mucositis, experienced by half of the enrolled patients. It was thought that trough level of SRL was relatively high in early period (2 weeks vs. 6 months, 7.9 ng/mL vs. 7.3 ng/mL, respectively). A previous report suggested that 3 to 7 days of topical clobetasol application was an effective treatment for SRL-induced aphthous ulcers [21]. Close monitoring of mucocutaneous complications and treatment with topical steroid ointment might be helpful, but as these patients were unable to tolerate these adverse events, we decided to withdraw these patients during the early period of SRL conversion. In addition, SRL caused hyperlipidemia and proteinuria, but the degree of proteinuria in our study was not clinically significant (PCR, 0.39 ┬▒ 0.40).
Our study had some limitations. First, the number of enrolled patients was small (31% participation rate) in spite of a detailed explanation of the advantages of SRL. Eligible patients were required to have received CNIs for more than 10 years. Therefore, it was difficult for clinicians to introduce new immunosuppressant to stable KT recipients who were also reluctant to change it. Second, there was no control group for comparing the change of renal function and adverse events after conversion. Third, the follow-up duration (6 months) was too short to observe any potential anticancer effect of SRL. A larger number of patients and long-term follow-up are needed in further studies.
In summary, SRL conversion in long-term CNI-exposed KT recipients with stable graft function is a safe and immunologically beneficial switch in terms of graft function, acute rejection and changes of T cell subsets. Drawbacks included intolerably severe mucocutaneous adverse events, ultimately resulting in study withdrawal. Close monitoring and effective treatment of mucocutaneous adverse events is required in the early period after SRL conversion to ensure success.
Acknowledgments
This study was supported by a grant from the Korean Health Technology R&D Project, Ministry for Health and Welfare, Republic of Korea (HI09C1555).
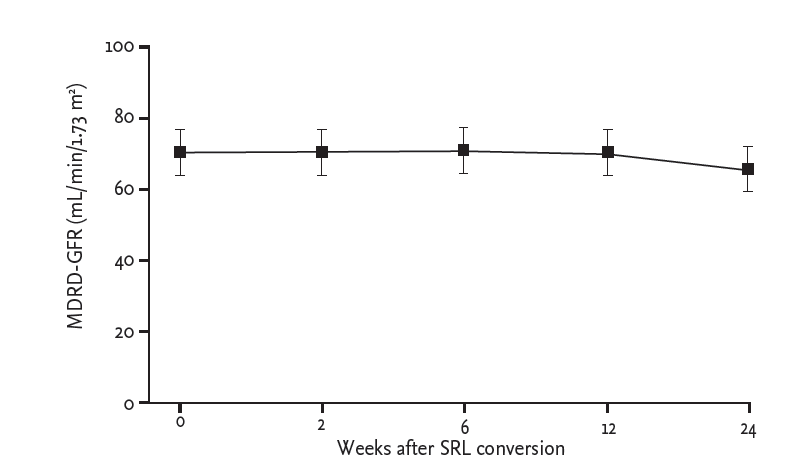
Figure┬Ā1.
Renal allograft function during 24 weeks after sirolimus conversion (n = 9, p = 0.115). Note no significant change of graft function after sirolimus (SRL) conversion. Black dots indicate means; error bars indicate standard errors. MDRD, modification of diet in renal disease; GFR, glomerular filtration rate.
Figure┬Ā2.
Trough level of (A) tacrolimus (TAC), and (B) cyclosporin (CsA) before and 2 weeks after sirolimus (SRL) conversion, (C) trough level of sirolimus at 2, 6, 12, and 24 weeks after SRL conversion. Black dots indicate means; error bars indicate standard errors.
Figure┬Ā3.
Effect of conversion from calcineurin inhibitors to sirolimus on CD4+ T lymphocyte subpopulations within the peripheral blood mononuclear cell population isolated from kidney transplant recipients (n = 6). The percentage of (A) regulatory T cells (Treg), (B) Th1, (C) Th2, and (D) Th17 cells before and after 6 months sirolimus (SRL) conversion were compared. Note significant increase of CD25+ Foxp3+/CD4+ T cells (Treg) after SRL conversion (6.3% ┬▒ 3.2% vs. 8.6% ┬▒ 5.4%). IFN-╬│, interferon ╬│; IL-4, interleukin 4. ap 0.028, Wilcoxon signed-rank test.
Figure┬Ā4.
Effect of conversion from calcineurin inhibitors to sirolimus (SRL) on CD8+ T lymphocyte subpopulations within the peripheral blood mononuclear cell population isolated from kidney transplant recipients (n = 6). The percentage of (A) CD8+ Tnaïve, (B) CD8+ TCM, (C) CD8+TEM, and those of interferon γ (IFN-γ) producing cells (D, E, F) before and after 6 months SRL conversion were compared. Note significant decrease of IFN-γ producing CD8+ TCM cells after SRL conversion (58.5% ± 18.9% vs. 37.9% ± 25.4%). TCM, central memory T cells; TEM, effector memory T cells. ap 0.046, Wilcoxon signed-rank test.
Table┬Ā1.
Baseline characteristics of patients
REFERENCES
1. Li C, Yang CW. The pathogenesis and treatment of chronic allograft nephropathy. Nat Rev Nephrol 2009;5:513ŌĆō519.


2. Kasiske BL, Snyder JJ, Gilbertson DT, Wang C. Cancer after kidney transplantation in the United States. Am J Transplant 2004;4:905ŌĆō913.


3. Vincenti F, Friman S, Scheuermann E, et al. Results of an international, randomized trial comparing glucose metabolism disorders and outcome with cyclosporine versus tacrolimus. Am J Transplant 2007;7:1506ŌĆō1514.


4. Stallone G, Schena A, Infante B, et al. Sirolimus for KaposiŌĆÖs sarcoma in renal-transplant recipients. N Engl J Med 2005;352:1317ŌĆō1323.


5. Saemann MD, Haidinger M, Hecking M, Horl WH, Weichhart T. The multifunctional role of mTOR in innate immunity: implications for transplant immunity. Am J Transplant 2009;9:2655ŌĆō2661.


6. Zhao T, Yang C, Qiu Y, et al. Comparison of regulatory T cells and FoxP3-positive T-cell subsets in the peripheral blood of renal transplant recipients with sirolimus versus cyclosporine: a preliminary study. Transplant Proc 2013;45:148ŌĆō152.


7. Stallone G, Infante B, Schena A, et al. Rapamycin for treatment of chronic allograft nephropathy in renal transplant patients. J Am Soc Nephrol 2005;16:3755ŌĆō3762.


8. Schena FP, Pascoe MD, Alberu J, et al. Conversion from calcineurin inhibitors to sirolimus maintenance therapy in renal allograft recipients: 24-month efficacy and safety results from the CONVERT trial. Transplantation 2009;87:233ŌĆō242.


9. Weir MR, Mulgaonkar S, Chan L, et al. Mycophenolate mofetil-based immunosuppression with sirolimus in renal transplantation: a randomized, controlled Spare-the-Nephron trial. Kidney Int 2011;79:897ŌĆō907.


10. Guba M, Pratschke J, Hugo C, et al. Early conversion to a sirolimus-based, calcineurin-inhibitor-free immunosuppression in the SMART trial: observational results at 24 and 36months after transplantation. Transpl Int 2012;25:416ŌĆō423.


11. Soleimani AR, Kamkar I, Nikoueinejad H, Moraweji AR. Comparison of cyclosporine and sirolimus effects on serum creatinine level over five years after kidney transplantation. Transplant Proc 2013;45:1644ŌĆō1647.


12. Diekmann F, Campistol JM. Conversion from calcineurin inhibitors to sirolimus in chronic allograft nephropathy: benefits and risks. Nephrol Dial Transplant 2006;21:562ŌĆō568.


13. Alvarez-Lara MA, Carracedo J, Ramirez R, et al. The imbalance in the ratio of Th1 and Th2 helper lymphocytes in uraemia is mediated by an increased apoptosis of Th1 subset. Nephrol Dial Transplant 2004;19:3084ŌĆō3090.


14. Lebranchu Y, Thierry A, Toupance O, et al. Efficacy on renal function of early conversion from cyclosporine to sirolimus 3 months after renal transplantation: concept study. Am J Transplant 2009;9:1115ŌĆō1123.


15. Guba M, Pratschke J, Hugo C, et al. Renal function, efficacy, and safety of sirolimus and mycophenolate mofetil after short-term calcineurin inhibitor-based quadruple therapy in de novo renal transplant patients: one-year analysis of a randomized multicenter trial. Transplantation 2010;90:175ŌĆō183.


16. Li Y, Shi Y, Huang Z, et al. CNI induced Th17/Treg imbalance and susceptibility to renal dysfunction in renal transplantation. Int Immunopharmacol 2011;11:2033ŌĆō2038.


17. Chung BH, Kim KW, Kim BM, et al. Dysregulation of Th17 cells during the early post-transplant period in patients under calcineurin inhibitor based immunosuppression. PLoS One 2012;7:e42011.



18. Kim KW, Chung BH, Kim BM, Cho ML, Yang CW. The effect of mammalian target of rapamycin inhibition on T helper type 17 and regulatory T cell differentiation in vitro and in vivo in kidney transplant recipients. Immunology 2015;144:68ŌĆō78.



19. Yap M, Boeffard F, Clave E, et al. Expansion of highly differentiated cytotoxic terminally differentiated effector memory CD8+ T cells in a subset of clinically stable kidney transplant recipients: a potential marker for late graft dysfunction. J Am Soc Nephrol 2014;25:1856ŌĆō1868.






 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



