INTRODUCTION
Patients with fever and hepatic or splenic lesions should have an abscess ruled out. Traditionally, amebic and pyogenic infections are the two most common causes of liver abscess and the former has decreased with improved public and individual hygiene [
1,
2]. Hepatosplenic fungal infection is another possible diagnosis, particularly in patients with hematologic malignancies such as acute leukemia [
3,
4] or tuberculosis (TB) in Korea where pulmonary and extrapulmonary TB are still common [
5].
A diagnosis of hepatosplenic lesions usually depends on invasive procedures such as sonography-guided biopsy or aspiration with subsequent microbiological confirmation. However, invasive diagnostic procedures are not easy to perform in hematologic patients because of the increased bleeding risk and marked neutropenia following intensive chemotherapy. Therefore, management is largely dependent on clinical diagnosis when few microbiological data are available.
QuantiFERON-TB Gold In-Tube (QFT-GIT, Cellestis Ltd., Victoria, Australia) is one of two interferon-╬│ release assays (IGRAs) that have been approved by the U.S. Food and Drug Administration and recommended by the U.S. Centers for Disease Control and Prevention as an aid to detection of latent TB infection among patients at risk [
6]. Several studies have investigated the diagnostic performance of IGRAs for extrapulmonary TB (E-TB) with some promising results [
7-
9].
In this retrospective study, we investigated the clinical characteristics, causes, and outcomes of hepatic or splenic lesions and evaluated the usefulness of the QFT-GIT for the diagnosis of TB in febrile patients with hematologic diseases.
DISCUSSION
We add an empirical antifungal agent when a hematologic patient develops a neutropenic fever that does not respond to empirical broad spectrum antibacterial therapy for more than 4 to 7 days. The next step is to take a CT scan of the chest or, less commonly, of the abdomen. During the study period, the investigators noticed unexpected hepatic or splenic lesions in some patients on CT scans; thus we evaluated the characteristics of these lesions.
Hepatic and splenic lesions in hematologic patients of infectious and noninfectious origins were difficult to distinguish. Although hypoalbuminemia was more common in the infectious group, laboratory findings were not useful for distinguishing between infectious and noninfectious origins (
Table 1). Concerns regarding postprocedural infection and bleeding limit invasive procedures. Only seven cases of infectious and two cases in the noninfectious group underwent percutaneous biopsy, drainage, or surgery. Hence, many patients received empirical antibiotic treatment and final diagnoses were usually based on other clinical information rather than definitive microbiology.
Among the 26 cases, 17 comprised the infectious group and five (29.4%) had direct microbiological evidence (
Tables 3 and
4) of infection. Most patients (n = 15, 88.2%) had hepatic involvement. Patients with a pyogenic liver abscess have been reported to present with leukocytosis, elevated alkaline phosphatase, hypoalbuminemia, and elevated C-reactive protein [
2,
13,
14]. However, only two (11.8%) had leukocytosis, eight (47.1%) had neutropenia, and seven (41.2%) had elevated alkaline phosphatase level in the present study.
Fungal liver abscesses have been reported mostly in patients with malignancies [
3,
15]. Marcus et al. [
15] reported 17 bacterial and 20 fungal hepatic abscesses in patients with cancer. Among those with fungal abscesses, 15 (75%) had hematological malignancies and 19 (95%) had undergone prior anticancer chemotherapy. Disseminated candidiasis is a well-established etiology of fungal hepatosplenic lesions in hematologic patients. Sallah et al. [
16] reviewed 23 hepatosplenic candidiasis patients with acute leukemia. Microorganisms were identified in 10 cases (43.8%), which were
Candida albicans (n = 6),
C. tropicalis (n = 3), and
C. glabrata (n = 1). We found two probable and one possible disseminated candidiasis case, and two were positive for
C. tropicalis in blood culture.
Case 8 had a large hepatic lesion consisting of a combined
E. faecium abscess with fungal hyphae.
Aspergillus species was considered initially because the branching hyphae had septations with acute angles, and the GM assay was positive. However, the tissue culture was negative for fungus [
17]. Huang et al. [
18] reported that 35 of 153 (22%) patients with a pyogenic hepatic abscesses had a concurrent fungal infection from 1973 to 1993. Hepatobiliary or pancreatic cancers were the most common associated diseases, and hematologic malignancies were not included in their study. Considering that fungal infection is not uncommon in hematologic patients, more aggressive and invasive procedures could identify combined etiologies more frequently.
Llenas-Garc├Ła et al. [
19] investigated 22 cases of splenic abscess and reported that
M. tuberculosis was the most frequent causative microorganism, accounting for eight patients (36.4%), all of whom had acquired immunodeficiency syndrome as a predisposing factor. In the present study, in which hematologic malignancy was a predisposing factor, five of 10 patients with splenic abscesses had TB followed by fungal (n = 4), and bacterial (n = 1) infections.
Primary hepatic TB is very rare and difficult to diagnose [
20-
22]. Chong [
21] reported 14 patients (0.74%) with hepatic TB of 1,888 patients with TB over a 10-year period. Only three patients (0.16%) had isolated hepatic involvement. The overall annual incidence ranged from 0.0% to 1.05% of all TB infections. Some investigators have reported that IGRAs are useful for diagnosing E-TB, which includes TB lymphadenitis most commonly, and pleural, skeletal, central nervous system, and abdominal TB less commonly [
7-
9,
23]. The reported sensitivities and specificities of IGRAs for the diagnosis of E-TB are 69% to 94% and 82% to 88%, collectively, and vary among disease sites [
7-
9]. In patients with suspected TB lymphadenitis, blood IGRA may be useful adjunct assay to diagnose or exclude E-TB [
8,
23], but blood IGRA alone is not useful for diagnosis of TB of the spine or central nervous system [
8,
24]. Previous studies included no or few, if any, hepatic or splenic TB patients and no other studies have evaluated the usefulness of the QFT-GIT for diagnosing hepatic or splenic TB in hematologic patients. In the present study, none of the patients had a history of TB, and QFT-GIT was positive in six of eight TB cases. The sensitivity and specificity of the QFT-GIT were 75% (6/8) and 81.3% (13/16). Excluding concurrent pulmonary TB, four of six cases were positive for QFT-GIT. TB should be considered for those not responding to antibacterial or antifungal drugs and the QFT-GIT may be useful in the differential diagnosis of hepatosplenic lesions in hematologic patients.
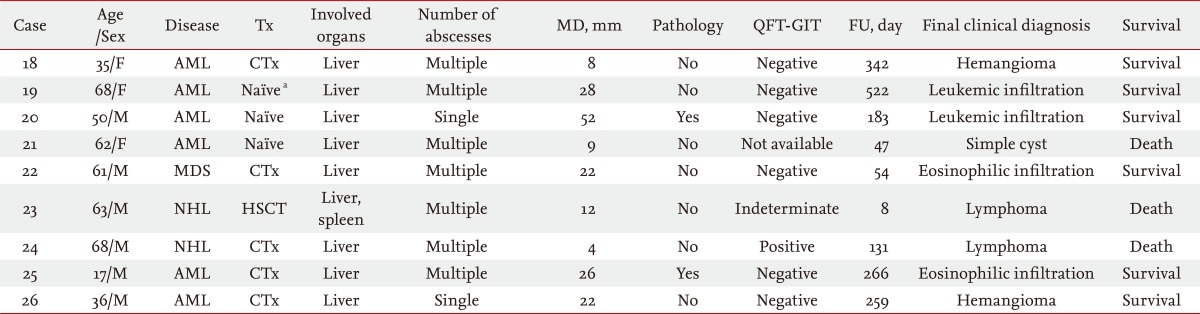
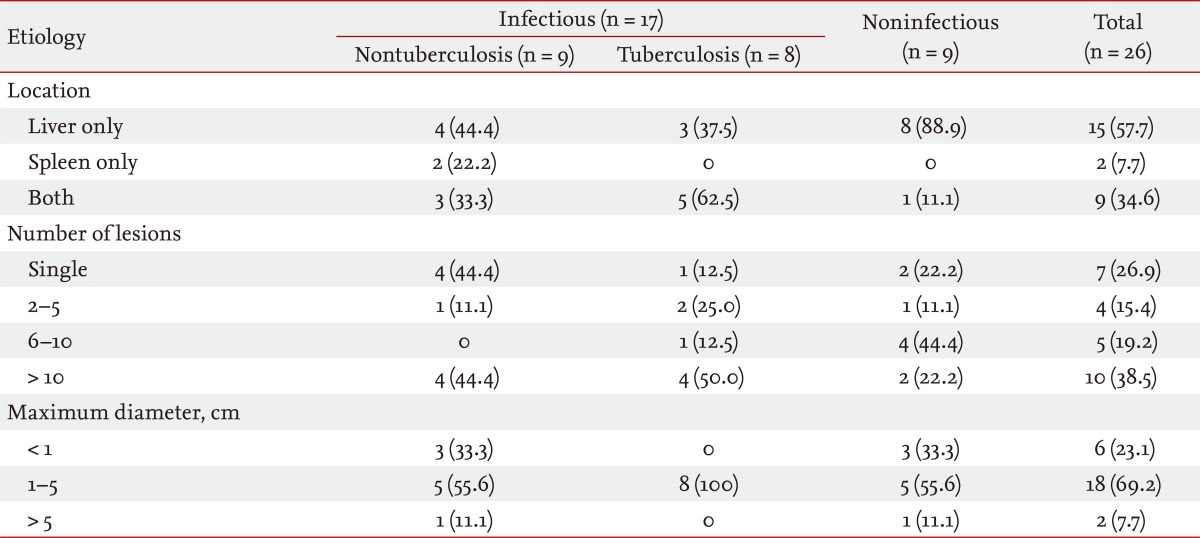
A noninfectious origin accounted for 34.6% of patients. The final diagnosis was based on a response to chemotherapy, underlying disease status, serial radiological findings, and laboratory results except for two pathologically confirmed cases. In contrast, most of the infectious group (n = 8, 88.9%) had isolated hepatic involvement.
Of the 17 infectious cases, the number of cures, improvements, and failures was nine, four, and four, respectively. Although five patients in the infectious group died during the follow-up period, hepatosplenic infections were not fatal and did not directly influence mortality. Those patients died of underlying disease progression (n = 2), another infection (n = 2), or brain hemorrhage (n = 1).
Considering the rarity of hepatosplenic TB, this study included a very small number of patients and was retrospective in nature. Thus, a larger prospective study is required to explore the usefulness of QFT-GIT in hepatosplenic TB.
In summary, causes of hepatic or splenic lesions in Korean hematologic patients are diverse and include bacterial, fungal, TB, and noninfectious origins. Meticulous diagnostic and therapeutic attempts should be made to identify the causative agent. QFT-GIT may be useful for the differential diagnosis of hepatosplenic lesions in hematologic patients, but more research is needed.









 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print



