Nephrotic Syndrome Associated with Renal Vein Thrombosis:
A report of 3 cases
Article information
Abstract
The coexistence of nephrotic syndrome and renal vein thrombosis has been of medical interest since Rayer’s description in 1840. Renal vein thrombosis has been underdiagnosed because of its variable clinical and radiological findings but it becomes a more frequently recognizable clinical entity since diagnosis can be easily established by modern angiographic techniques.
Generally it has been believed that renal vein thrombosis may cause nephrotic syndrome. But recent articles strongly suggest that renal vein thrombosis is a complication of the nephrotic syndrome rather than a cause. We report three cases of nephrotic syndrome associated with renal vein thrombosis.
INTRODUCTION
Since the association of nephrotic syndrome and renal vein thrombosis was first described by Rayer in 18401), several reviews of this association have been published2–6). With the developement of more advanced radiographic techniques, selective catheterization and more understanding on renal vein thrombosis in nephrotic syndrome, the diagnosis or renal vein thrombosis and studies of its cause and effect have been made with increasing frequency7–13).
We report three cases of renal vein thrombosis associated with nephrotic syndrome which were confirmed by abdominal computed tomographic scan, vena cavography, renal angiography and renal biopsy.
Case 1
A 15-year-old boy was hospitalized for evaluation of left side pain of 2 days duration and intermittent edema for the past 2 years.
He was diagnosed as having membranoproliferative glomerulonephritis when he was 13. There-after he was treated with Cytoxan and Prednisolone for 3 months. Admission physical examination disclosed severe edema on lower extremities and scrotum, hemorrhoid, ascites and moderate knocking tenderness on the left flank. A urinalysis showed 3+ protein, 1+ sugar, 3–4 WBCs and 10–20 RBCs per high power field. Urinary protein excretion showed fluctuation from 7.0 gm/24 hr to 20.3 gm/24 hr. Laboratory data included albumin 1.2 gm%, globulin 1.3 gm%, glucose 90 mg%, BUN 30 mg%, cratinine 1.2 mg% cholesterol 615 mg% and triglyceride 431 mg%. Abdominal computed tomographic scanning showed a hypodense lesion in the left renal vein (Fig. 1), which was confirmed by renal venography. The patient was started on a regimen of Dipyridamol and Aspirin. After 1 week, the pain was being controlled with an improved general condition. The patient was continued on the regimen.
Cases 2
A 27-year-old man was hospitalized for evaluation of left flank pain of 1 week duration. He was diagnosed as having nephrotic syndrome 6 months ago and treated with Prednisolone. The admission physical examination disclosed generalized edema especially in lower extremities. A urinalysis showed 3+ protein, 4–6 RBCs and 7–15 WBCs per high-power field. Urinary protein excretion showed a fluctuation from 3.5 gm%/24 hr to 10.0 gm%/24 hr. Laboratory data showed albumin 1.9 gm%, globulin 1.6 gm%, cholesterol 480 mg% and triglyceride 375 mg%. Differential studies on urine specimens revealed protein 5.8 gm%/24 hr, osmolality 298 mosm/l, Na 62 mEq/l, K 32 mEq/l and CI 46 mEq/l from the left ureter and protein 5.6 gm%/24 hr, osmolality 361 mosm/l, Na 63 mEq/I, K 42 mEq/l and CI 70 mEq/l form the right ureter. Abdominal computed tomographic scanning showed a hypodense lesion in the left kideny and renal venography showed a thrombus in distal renal vein (Fig. 2). The patient was treated with heparin and anticoagulants. On this regimen the pain disappeared and the renal function remained normal.
Cases 3
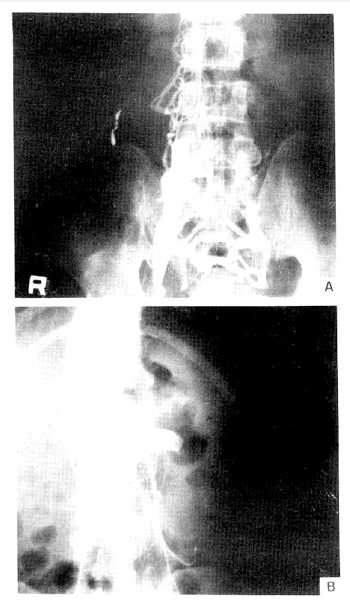
A-47-year-old man was hospitalized for evaluation of right flank pain of 3 days duration. He was otherwise asymptomatic and denied having trauma, edema or renal disease. A urinalysis showed 3+ protein, 1+ sugar, 7–10 RBCs and 8–10 WBCs per high-power field. Urinary protein excretion was 2.1–3.2 gm/24 hr during admission. Laboratory data included albumin 3.9 gm%, globulin 3.3 gm%, glucose 104 mg%, cholesterol 322 mg% and triglyceride 117 mg%. A needle biopsy specimen of the kidney revealed membranous changes. Immunofluorescent study showed linear deposit of IgG. Abdominal computed tomographic scanning showed a large thrombus in inferior vena cava and dilated azygos vein. Inferior vena cavogram showed complete obstruction in iliac vein region and abundant collaterals (Fig. 3). The patient was treated with anticoagulants and continued to do well.
COMMENT
In 1840, Rayer1) decribed 7 cases of renal vein thrombosis, of which 2 had clinical features of the nephrotic syndrome. Since Derow2) described a case of chronic thrombosis of the renal vein and inferier vena cava with the clinical picture of nephrotic syndrome in 1939, there have been a number of reports of the association of renal vein thrombosis and nephrotic syndrome3–6). It is generally agreed that the renal vein thrombosis is responsible for the development of the proteinuria of nephrotic syndrome and renal vein thrombosis is a rare but well-recognized cause of nephrotic syndrome3–5,9,10,14). However several lines of evidence in recent articles have questioned such hypothesis and strongly suggested that renal vein thrombosis is a consequence of the nephrotic syndrome rather than a cause, judging by the increasing number of case reports and various animal experiments15–23).
First, prospective long-term evaluation of nephrotic patients showed normal venogram and subsequent development of renal vein thrombosis18,19,24–26). Second, nephrotic syndrome itself is associated with hypercoagulable state and the patients with the nephrotic syndrome exibit a high incidence of thrombotic phenomena in vessels other than the kidney itself, for examble inferior vena cava, pulmonary artery and mesenteric artery25,27). Third, selective renal function studies in unilateral renal vein thrombosis showed similar total protein excretion and protein selectivity for each kidney21,28). The findings of Case 2 were in agreement with such a concept. Fourth, renal vein obstruction induced in experimental animals caused mild proteinuria and pathologic change in the renal biopsy specimen3,23). Omae et al.29) found that excision of the intact contralateral kidney one week after partial occlusion of one renal vein was followed by development of a nephrotic syndrome with some thickening of glomerular basement membranes visible by light microscopy. Fisher et al.22) confirmed the development of nephrotic syndrome in rats. Although increased permeability of glomerular lamina densa was demonstrated in nephrotic kidneys, deposit or other overt membranous changes were lacking. Harris et al.14) reported thickened basement mambrane and deposit of r-globulin in glomeruli of dogs after total constriction of one renal vein and suggested that the damage to the affected kidney produced an autoimmune reaction in the other. Polenakovic et al.23) found that increased proteinuria did occur during the first 3 days after obstruction of a renal vein to 0.5 mm in rats. However he failed to find any difference from control animals in the amount of proteinuria and any evidence of membranous glomerulitis in renal biopsy specimen.
It is well-known that renal vein thrombosis occurs mainly in membranous glomerulopathy and less frequently in membranoproliferative glomerulonephritis. The incidence of renal vein thrombosis in the retrospective studies of membranous glomerulonephritis and membranoproliferative glomerulonephritis has been found to be 33% by Trew et al.30), 40% by Llach et al.24) and 50 % by Bennet et al.31) Other renal lesions that are associated with renal vein thrombosis are minimal change lesion, focal sclerosis13), rapidly progressive glomerulonephritis, malignancy25), and IgA nephropathy20). Systemic diseases involving kidney associated with renal vein thrombosis are lupus nephritis18), amyloidosis26), diabetic nephropathy, sickle cell anemia, polyarteritis nodosa33), malignant hypertension25), and paroxysmal nocturnal hemoglobulinuria32).
Although the pathogenetic machanism of renal vein thrombosis in nephrotic syndrome is not completely understood, it is established that the nephrotic syndrome is associated with a hypercoagulable state.
Patients with nephrotic syndrome have an increase in the number of platelets and in blood levels of fibrinogen, factor V, combined factors VIII and X, accelerated thromboplastin generation and increased activation of Hagemann factor26,27). The milieu is enhanced further by the urinary loss and depressed serum level of antithrombin III, so critical to the inhibition of several clotting proteases21). Poor fibrinolysis because of increased plasmin inhibitors and reduced blood flow because of decreased plasma volume and cariac output also has a role36). Furthermore the coagulation abnormalities returned to normal with the remission of nephrotic state26,35). In this situation, diruretics, corticosteroids and oral pills which may exert thrombogenic activity should be used with caution22,27,37).
The clinical features are determined by the balance between the acuteness of occlusion, extension of the thrombosis and development of collateral circulation33). Acute presentation of renal vein thrombosis is infrequent and is observed frequently in the younger patients with acute flank pain and marked costoverterbral angle tenderness. Chronic renal vein thrombosis is observed frequently and patients are usually older and relatively asymptomatic. Complaints will be of a chronic nature, that is, nausea, apathy, weakness and generalized edema, or they may be absent completely9,33).
Laboratory findings which may suggest renal vein thrombosis are variability in proteinuria and in creatinine clearance, hematuria, pyuria, glycosuria, and hyperchloremic acidosis. The variability in proteinuria and creatinine clearance also shown in our cases is probably due to varying degree of venous obstruction and recurrent thrombus formation in the renal vein.
Formation of collateral channels and their subsequent thrombus may be a second cause9). Our Case 3 was very unusual in that serum albumin was 3.9 gm% and urinary protein excretion was 2. 1–3.2 gm/24hr. Considering the correlation between serum albumin level and antithrombin III by Kauffmann et al.34) and some animal experiments which showed proteinuria after renal vein obstruction14,22,29), we cannot rule out the possibility that it might be a beginning of development of nephrotic syndrome after longstanding renal vein thrombosis.
Renal vein thrombosis in nephrotic syndrome is thought to be underdiagnosed because it has variable clinical and radiological presentations and no local signs or symptoms at all in many instances24,26,33,38). The early diagnosis of renal vein thrombosis is very important because it is a treatable condition and radiologic evaluation is essential for it. An intravenous pyelogram, usually the initial investigation of choice, can suggest thrombosis but is insufficient for definitive diagnosis. It may reveal asymmetry in kidney size and function if thrombosis is unilateral and notching of the ureter due to dialated collaterals28,33). Renal arteriography with late films of the venous phase can be the first angiographic procedure because it can assess the renal parenchyma, blood flow and presence of collaterals without the risk of dislodging thrombi33,40). But the most definitive diagnostic modality is renal venography. Care must be exercised in its performance because of the risk of dislodging thrombi with resultant pulmonary embolism and in its interpretation because “streaming” artifact made by the normally high rate of blood flow entering the vena cava from the renal vein may lead to an erroneous diagnosis.
Accurate diagnosis can be made if contrast material is visualized surrounding a filling defect in the renal vein10,42). Recently, Doppler ultrasound and abdominal computed tomographic scanning have been used as rapid and safe noninvasive diagnostic measures for visualizing thrombus in renal vein directly39,41,43). Abdominal computed tomographic scanning showed thrombi in all of our cases.
As with renal vein thrombosis, both medical and surgical treatment has been advocated. Although there have been a lot of reports of a favorable outcome after thrombectomy3,7,9,10), the treatment has shifted from a surgical to a medical focus during the last 20 years33,44). The objective of anticoagulant therapy is not only to minimize the occurance of pulmonary embolism but also to retard growth of a renal vein thrombus, thereby helping to preserve renal function and prevent the spread to the vena cava or to the other renal vein8,9,26,44,45). Once the diagnosis has been establish, hepatization followed by warfarin is the initial treatment of cloice33).
On the other hand, thrombectomy might be indicated in unrelenting pulmonary emboli and oliguria refractory to medical therapy from bilateral renal vein thrombosis or thrombosis of a solitary kidney33). Reports of other therapeutic measures have included the administration of Dextran46), Dipyridamol47), and the thrombolytic agents Urokinase and Streptokinase48–50) but they need more extended experience.